
- +94 77 288 4021

Assignment Lanka
Assignment lanka- best assignment help in sri lanka, assignment lanka assignments thesis project work reports dissertations.

What Is Assignment Lanka?
We are Sri Lanka’s best Academic Writing firm with top talented writers. At Assignment Lanka, We thrive to deliver the best quality Assignments and Researches at a very affordable price. We cater to an array of subjects. Click here to find out the subjects we offer. We have been in the industry for more than 10 years and we are trusted by thousand of students. We offer assignment help service in a variety of programs . We have been the pioneers in the Assignment Writing genre and have helped thousands of needy students.
Our Assignment writers are just the best experts in the field and we make sure that they are the cream of the class. Our able writers are being tested throughout their tenure with us to provide the best service for our valuable customers. Our elite proofreading panel evaluates them on a quarterly basis to assess their development. Read about Assignment Lanka here . Check Our Facebook Page for our community attraction.
You have nothing to worry as thousands of students have recommended us for our exquisite service. Click here to find out some of those.
Click to look at our Academic Writing and Academic Coaching Features .
Why Should you select assignment lanka?
Our assignment help features, talented writers.
Our writer squad consists of skillful assignment help experts with years of experience. We test them frequently to keep up our quality.
Best quality assignment help
Our assignment help hub is rich in all the resources in the world. We ensure zero plagiarism and error-free documents.
Payments and Quotes
Get a free assignment help quote instantly. Our payment options are secure. Your information is safe with our SSL protection.
Customer Service
Our customer service agents are available via Messenger, Instagram. Assignment Lanka's Assignment Help WhatsApp line is open 24/7.
assignment help Reviews
Our assignment help reviews prove that you are already in the right place. We have 4.8 stars out of 5 in our customer review scheme.
we are just a call away
Our assignment help online team is always on standby. We always update the progress from our end.
Subjects we offer in Assignment help

What is assignment help?
Assignment Lanka offers an array of content creation assistance. We have been offering assignment help for students from a long time. Therefore, unlike other firms, we know what we are doing. Our academic assistance experts are very knowledgeable and you will not regret choosing us. Assignment Lanka Writing Service is the all-in-one assignment help hub you have been looking for…!!.
Here are some of the services we offer;
Assignment Help
Our assignment writers, research help, proofread content, data analysis, data wizards, coaching sessions, one on one coaching, our assignment help specialties, on time in full delivery.
We are the best assignment help service in Sri Lanka. Its because of our quality works, delivered on time. We will never break your heart.
Zero Plagiarism Detected
The project is ensured to be free from any plagiarism. Be it an MBA, SLIM, PQHRM, PhD or HND, the document is with zero plagiarism.
Guaranteed Satisfaction
Our Assignment help reviews suggest the best imaginable satisfaction for our clients.
Private & Confidential
Your details are entirely safe with us. Therefore, no information will leak to a third party. We even encrypt the document with our assignment help writers to hide your personal information.
Our Assignment Help Impressions up-to Date
Our assignment helping programs.

Assignment Help Consultations
Timely delivery, 𝗕𝗲𝗮𝘂𝘁𝘆 𝗼𝗳 𝗔𝘀𝘀𝗶𝗴𝗻𝗺𝗲𝗻𝘁 𝗪𝗿𝗶𝘁𝗶𝗻𝗴 𝗦𝗲𝗿𝘃𝗶𝗰𝗲 😍.
𝗙𝗲𝗮𝘁𝘂𝗿𝗲𝘀 𝗼𝗳 𝗘𝗱𝘂𝗰𝗮𝘁𝗶𝗼𝗻 𝗖𝗼𝗮𝗰𝗵𝗶𝗻𝗴 𝗦𝗲𝗿𝘃𝗶𝗰𝗲 😍

Kindly recheck your contact number before sending, so we can contact you ASAP.
Need help? Call our award-winning support team 24/7 at +94 77 288 4021

We are the best Academic Writing service provider in Sri Lanka. Our customers have not seen an “F”. Our quality, superior service and timely delivery would testify for the authenticity of our work.
Get your quotation
Book a call.

Rated 4.8/5
Out of 578 Reviews

Dedicated Customer Care
Trained Customer Care Agents to Guide You Through

Free Turnitin Report
Free turnitin Report on Request. We also do Customized Manual Plagiarism and Similarity Checks

Our Contents are Well Researched. Zero Plagiarism and Low Similarity is Guaranteed.
Many reasons to
Why choose us.
Webster's ultimate easy to use and customizable UI elements make it most customizable template on the market.
Plagiarism Free Service
Confidentiality guaranteed.
- Direct Access
- Flexible Payment
We pass every conference paper, journals, report, essay, assignment, coursework, personal statements and CV through our plagiarism checkers to ensure that they are plagiarism free.
Be assured that your privacy will not be breached. We do not divulge any information about you to anyone for whatsoever reason.
Our emails are working round the clock, be rest assured that you can send us an email at any time of the day and expect a reply between a few minutes to the next few hours.
Direct Access to Experts
Get direct access to our academic experts and build a personal relationship with them via skype calls, emails or face to face
Flexible Payment Option
For writing related projects that are more than 20 days, we allow a flexible payment structure to be determined with the academic researchers, professional writers, study abroad consultants, cv writing experts or tutors assigned to you.
How we are the best!
How we work.
Truly ideal solutions for your business. Create a website that you are gonna be proud of.
- Upload Work
- Await Estimate
- Half Payment
- Draft Request
- Work is Ready
Many Style Available
First place an order with the relevant information regarding your academic research paper, conference paper, journals, report, essay, assignment, coursework, dissertation, thesis, personal statement, motivational statement, reference letter review and Curriculum Vitae (CV) needs for computer science, information technology, software engineering, business management, mathematics, physics, biology, microbiology, geology, geoscience, geography, statistics, chemical science, education, medical science, biomedical science, biochemistry, health & social care, economics, sociology, psychology, philosophy, mechanical engineering, acoustical engineering, mechatronics engineering, civil engineering, aerospace engineering, electrical/electronics engineering, chemical/petroleum engineering, history, political science, english literature and law.
After you have uploaded your work, our team of academic researchers, professional writers, study abroad consultants, cv writing experts or tutors will evaluate your requirements and get back to you with an estimated cost as well as how long it will take to complete it.
You will need to make at least a 50% deposit before we start working on your order except for orders that are more than 20 days which might require a lesser payment.
The academic researchers, professional writers, study abroad consultants, cv writing experts or tutors assigned to you will give you an update whenever you ask for it before the deadline or at a previously agreed time.
Once the work is ready, our team will contact you to make a final deposit before sending you the work. We can also send half of the completed work if you request to see it before proceeding to make the other payment
If you have feedback about part of the work that needs correction or does not meet the requirement you have stated, or you want to change some information, we will be glad to do it at no cost. An exception to this will be writing entirely new additional content that was not previously agreed.
For your benefit
Find academic resources, research paper, conference paper, journals, report, dissertation, thesis, essay, coursework, assignment, tutoring, curriculum vitae (cv), study abroad application, proofreading & editing help.
Sometimes students often find it difficult to grasp the core concept of a module or understand an assignment brief, at other times, they might just lack the initiative to start, here is where we can render our expertise. Our team of academic research expert and professional writers can help you write plagiarism-free academic research paper, conference paper, journals, report, assignments, essays, coursework, thesis & dissertations in the following fields:
- Information Technology & Computer Science Coursework
- Information Technology & Computer Science Proposal, Dissertations & Thesis
- Business Management Assignments & Essays
- Business Management Proposal, Dissertations & Thesis
- Law Assignments & Essays
- Law Proposal, Dissertations & Thesis
- Mathematics Assignments, Coursework & Essays
- Mathematics Proposal, Dissertations & Thesis
- Accounting & Finance Assignments & Essays
- Accounting & Finance Proposal, Dissertations & Thesis
- English Literature Assignments & Essays
- English Literature Proposal, Dissertations & Thesis
- Statistics Assignments, Coursework & Essays
- Statistics Proposal, Dissertations & Thesis
- Physics Assignments, Coursework & Essays
- Physics Proposal, Dissertations & Thesis
- Geology Assignments, Coursework & Essays
- Geology Proposal, Dissertations & Thesis
- GeoPhysics Assignments, Coursework & Essays
- GeoPhysics Proposal, Dissertations & Thesis
- GeoScience Assignments, Coursework & Essays
- GeoScience Proposal, Dissertations & Thesis
- Geography Assignments, Coursework & Essays
- Geography Proposal, Dissertations & Thesis
- Biological Science Assignment & Essays
- Biological Science Proposal, Dissertations & Thesis
- Microbiology Assignment & Essays
- Microbiology Proposal, Dissertations & Thesis
- Chemical Science Assignments & Essays
- Chemical Science Proposal, Dissertations & Thesis
- Education Assignments & Essays
- Education Proposal, Dissertations & Thesis
- Medical Science Assignments & Essays
- Medical Science Proposal, Dissertations & Thesis
- Biomedical Science Assignments & Essays
- Biomedical Science Proposal, Dissertations & Thesis
- Biomchemistry Assignments & Essays
- Biomchemistry Science Proposal, Dissertations & Thesis
- Health & Social Care Assignments & Essays
- Health & Social Care Proposal, Dissertations & Thesis
- Economics Assignments & Essays
- Economics Proposal, Dissertations & Thesis
- Political Science Assignments & Essays
- Political Science Proposal, Dissertations & Thesis
- History Assignments & Essays
- History Proposal, Dissertations & Thesis
- Sociology Assignments & Essays
- Sociology Proposal, Dissertations & Thesis
- Psychology Assignments & Essays
- Psychology Proposal, Dissertations & Thesis
- Agricultural Science Assignments & Essays
- Agricultural Science Proposal, Dissertations & Thesis
- Philosophy Assignments & Essays
- Philosophy Proposal, Dissertations & Thesis
- Architecure Assignments, Coursework & Essays
- Architecure Proposal, Dissertations & Thesis
- Mechanical Engineering Assignments, Coursework & Essays
- Mechanical Engineering Proposal, Dissertations & Thesis
- Civil Engineering Assignments, Coursework & Essays
- Civil Engineering Proposal, Dissertations & Thesis
- Mechatronics Engineering Assignments, Coursework & Essays
- Mechatronics Engineering Proposal, Dissertations & Thesis
- Electrical & Electronics Engineering Assignments, Coursework & Essays
- Electrical & Electronics Engineering Proposal, Dissertations & Thesis
- Chemical & Petroleum Engineering Assignments, Coursework & Essays
- Chemical & Petroleum Engineering Proposal, Dissertations & Thesis
- Acoustical Engineering Assignments, Coursework & Essays
- Acoustical Engineering Proposal, Dissertations & Thesis
- Aerospace Engineering Assignments, Coursework & Essays
- Aerospace Engineering Proposal, Dissertations & Thesis
We are confident we can deliver academic research paper, conference paper, journals, report, essay, assignment, coursework, dissertation & thesis with in-depth research, perfect sentence structure, impeccable grammar, in-text citation, flowing paragraphs and recent scholarly sources and references; we are fully conversant with various referencing style such as MLA, OSCOLA, Vancouver, IEEE, APA, Chicago, Harvard etc. Kindly note that our model academic research paper, conference paper, journals, report, essay, assignment, coursework, dissertation & thesis are not to be submitted as your work but only serve as a model to work with in writing your own academic research paper, conference paper, journals, report, essay, assignment, coursework, dissertation or thesis
Our information technology, computer science, software engineering & computing related tutoring services cover various areas like:
- Programming
- Cloud Computing
- Software Engineering
- Database Management
- Formal Design
- Artificial Intelligence
- Web Development
- Mobile Development
- Network Design & Management
- Distributed Systems and Networks
- Interaction Design
- Computer Architecture
- Operating System
- Computer Vision
- Embedded Systems
- Game Design and Development
- Data Visualisation & Data Mining
- Cyber Security & Forensic Science
- Data Analysis
- Data Structure & Algorithm
- Automata & Model Checking
- Edexcel & Cambridge O-Level & A-Level Computing
Our business administration, management & accounting related tutoring services cover various areas like:
- Project Management
- Management Analysis
- Operational Management
- Supply Chain Management
- Business Analysis
- Leadership & Organizational Behaviour
- Retail Management
- Game Theory for Business
- Business Analytics
- Digital Marketing for Business
- Management Ethics
- Organisation and Management
- Corporate Governance
- Management Accounting
- Financial Accounting
- Financial Market
- Audit & Taxation
- Futures and Options
- International Banking
- Knowledge Management
- Risk Management
- Strategic Management
- Software for Data Analysis & Modelling
- Financial Analysis, Information & Markets
- Edexcel & Cambridge O-Level & A-Level Business Studies
- Edexcel & Cambridge O-Level & A-Level Accounting
Our law, history, psychology & english related tutoring services cover various areas like:
- General Law
- Business & Mercantile Law
- Commercial Law
- Taxation Law
- Contract Law
- Criminal Law
- Business and Corporate Law
- Economic and Commercial Law
- Administrative & Constitutional Law
- Judiciary Examination
- Law Entrance Examination
- Insolvency Law
- Public International Law
- Commercial Arbitration Law
- Equity and Trusts
- Legal Research and Writing
- The Law of Torts
- Contract & Tort
- Employment Law
- Data Protection Law
- Intellectual Property Law
- Psychology of Attractiveness
- Research Methods & Data Analysis
- Human Origins
- Criminology
- The Psychology of Mental Health
- Health Psychology
- Cognitive Neuroscience
- Social Psychology
- Perception Psychology
- Language & Memory
- Empirical Studies
- Developmental Psychology
- Social & Psychological Approaches to Understanding Sexual Health
- Social & Affective Neuroscience
- Self-Conscious Emotions
- Psychology of Advertising
- Perspectives in Human Animal Interactions
- Relations and Interpersonal Influence
- Educational Psychology
- Human Learning
- Developmental Psychopathology
- Childhood Maltreatment & Mental Health
- Advanced Quantitative Research Skills
- Clinical Psychology
- Advanced Research Methods
Our mathematics & statistics related tutoring services cover various areas like:
- Trigonometry
- Differential Equation
- Mathematical Modelling
- Set & Number System
- Real Analysis
- Operational Research
- Financial Mathematics
- Probability
- Statistical Distribution Theory
- Group Theory
- Statistical Modelling
- Mathematical Programming
- Numerical Methods
- Statistical Inference
- Simulation & Queues
- Structure and Dynamics of Networks
- Optimisation
- Mathematical Finance
- Integral Transform Methods
- Hilbert Spaces
- Galois Theory
- Advanced Fluid Dynamics
- Algebraic Topology
- Actuarial Mathematics
- Complex Analysis
- Computer-based statistical modelling
- Stochastic Processes
- Edexcel & Cambridge O-Level & A-Level Mathematics
- Edexcel & Cambridge O-Level & A-Level Statistics
Our philosophy, politics & economics related tutoring services cover various areas like:
- Macroeconomics
- Statistics for Economics
- Microeconomics
- International Relations
- Mathematics for Economics
- Political Inquiry & Theory
- American Political Thought
- Children and Human Rights
- Chinese Politics
- Comparative Party Politics
- Contemporary Theories of Justice
- Democratic Theory
- Development Economics
- Diaspora Politics in Transnational Space
- Epistemology
- Ethics of Global Poverty
- Ethics of Public Policy
- European Security Governance
- Gender, Power and Politics
- Globalisation and World Politics
- Industrial Economics
- Econometrics
- Philosophical Logic
- Metaethics & Metaphysics
- Moral Philosophy
- Philosophy of Language, Mind & Religion
- Public Policy Analysis
- Politics & International Relations
- Realism and Idealism in International Relations
- Reason and Argument
- The Politics and Governance of the EU
- Theorising International Politics
- Understanding Modern China
- Action, Reason and Ethics
- Classical Indian Philosophy
- Party Politics
- Philosophy of Sex
- Politics and Protest
- The Ethics of Belief
- Wittgenstein's Later Philosophy
Our medical science, health & social care related tutoring services cover various areas like:
- Cardiopulmonary (CP)
- Endocrinology and the Life Cycle
- Research for Medicine and Health
- Renal & Urinary Systems
- Nervous System
- Gastrointestinal (GI)
- Medicine and Elderly Care
- Primary Medical Care
- Long Term Conditions
- Surgery and Orthopaedics
- Obstetrics and Gynaecology
- Clinical Ethics & Law
- Child Health
- Global and Public Health
- Mental Health
- Health Sciences for Nursing
- Clinical Assessment and Planning Care for Children
Our biomedical science, biochemistry, microbiology, biology & chemistry related tutoring services cover various areas like:
- Chemistry of Life
- The Human Genome & Disease
- The Molecular and Structural Basis of Disease
- Neuroscience
- Selective Toxicity
- Regulation of Gene Expression
- Neuropharmacology of CNS Disorders
- Neuropharmacology
- Cell Signalling
- Bioinformatics
- Systems Biology
- Data Management & Linear Modelling for Biologists
- Biomedical Parasitology
- Biofilms & Microbial Communities
- Pharmacology
- Immunology, Infection & Inflammation
- Medical Microbiology
- Exploring Proteins
- Vertebrate Development
- Cancer Chromosome Biology
- Biomedical Technology
- Origins of Biodiversity
- Population Ecology
- Environmental Pollution
- Environmental Microbiology
- Quantitative Methods in Biological Science
- Plant Development and Function
- Cell and Developmental Biology
- Molecular Recognition
- Cellular Signalling in Health & Disease
- Organic Chemistry
- Inorganic Chemistry
- Mathematical Methods in Chemistry
- Analytical Chemistry
- Solid State & Organometallic Chemistry
- Organic Reaction Mechanisms
- Coordination Chemistry
- Change & Equilibrium
- Atomic & Molecular Interactions
- Aspects of Organic Synthesis
- Physical Chemistry
- Chemical Biology
- X-Ray Crystallographic Techniques
- Supramolecular Chemistry
- Sustainable Chemistry
- Nuclear Magnetic Resonance Spectroscopy
- Medicinal Chemistry
- Macrocyclic & Bio-inorganic Chemistry
- Atoms, Molecules & Spins
- Spectroscopy and Applications
- Edexcel & Cambridge O-Level & A-Level Chemistry
- Edexcel & Cambridge O-Level & A-Level Biology
Our physics, geoscience, geophysics, geology & geography related tutoring services cover various areas like:
- Electricity & Magnetism
- Energy and Matter
- Mathematical Methods For Physical Scientist
- Motion and Relativity
- Programming and Data Analysis
- Waves, Light and Quanta
- Astronomy and Space Science
- Basin Analysis
- Classical Mechanics
- Electromagnetism
- Quantum Physics
- Statistical Mechanics
- Wave Physics
- Energy in The Environment
- Nanoworld & Nanoscience
- Medical Physics
- Practical Photonics
- Stellar Evolution
- Space Plasma Physics
- Photons in Astrophysics
- Particle Physics
- Lasers, Light & Matter
- Physics of the Ocean
- Coherent Light, Coherent Matter
- Earth and Ocean System
- Modelling Coastal Processes
- Seafloor Exploration & Surveying
- Global Climate Change
- Nuclear Physics
- Matter, Space and Time
- Nuclei and Particles
- Crystalline Solids
- Atomic Physics
- Volcanic and Mantle Processes
- Palaeoclimate Change
- Environmental & Engineering Geology
- Global Tectonics
- Geophysical Field Methods
- Applied & Marine Geophysics
- Structural Geology & GIS
- Igneous & Metamorphic Petrology
- Geochemistry
- Exploration Geophysics & Remote Sensing
- Ocean Biogeochemistry
- Dynamic Landscapes
- Cultural Geography
- Economic Geography
- Geographies of Wellbeing
- Global Water Resources
- Quaternary Environmental Change
- Remote Sensing for Earth Observation
- Biogeography
- Geohazards & Earth Resources
- Palaeobiology
- Ocean Data Analysis and Modelling
- Monitoring Coastal and Estuarine Environments
- Environmental Radioactivity and Radiochemistry
- Petroleum Geology & Mineral Resources
- Environmental Law & Management
- Edexcel & Cambridge O-Level & A-Level Physics
Our acoustic engineering, mechanical engineering, architecture & civil engineering related tutoring services cover various areas like:
- ThermoFluids
- Electrical and Electronics Systems
- Mechanics, Structures & Materials
- Engineering Management & Law
- Thermodynamics
- Finite Element Analysis in Solid Mechanics
- Control and Instrumentation
- Biomaterials
- Automobile Systems
- Advanced Partial Differential Equations
- Manufacturing and Materials
- Systems Design and Computing
- Sustainable energy systems, resources and usage
- Surface Engineering
- Orthopaedic Biomechanics
- Microstructural and Surface Characterisation
- Materials for Transport Applications
- Human Factors in Engineering
- Biomedical Implants and Devices
- Biomedical Application of Signal and Image Processing
- Vehicle Powertrain, Noise and Vibration
- Heat Transfer and Applications
- Electronics, Drives and Control
- Audio and Signal Processing
- Acoustics & Electroacoustics
- Signal Processing
- Ocean Acoustics & Biomedical Ultrasound
- Numerical Methods for Acoustics
- Mathematical methods for acoustics
- Architectural and Building Acoustics
- Active Control of Sound and Vibration
- Noise Control Engineering
- Human Responses to Sound and Vibration
- Acoustical Engineering Design
- Mechanics, Machines & Vibration
- Fluid Mechanics
- Waste Resource Management
- Transport, Energy and the Environment
- Transport Management and Safety
- Energy Resources and Engineering
- Energy Performance Assessment of Buildings
- Earthquake Engineering and Seismic Design of Steel Buildings
- Composites Engineering Design and Mechanics
- Advanced Finite Element Analysis
- Urban Design
- Structural Engineering
- Geotechnical Engineering
- Structural Design and Materials
- Structural Analysis
- Soil Mechanics
Our electrical & electronics engineering, mechatronics engineering & aerospace engineering related tutoring services cover various areas like:
- Digital Systems and Microprocessors
- Solid State Devices
- Electronic Systems
- Electronic Circuits
- Electrical Machines, Materials & Fields
- Computer Engineering
- Power Electronics and Drives
- Power Circuits and Transmission
- Electromagnetism for EEE
- Electrical and Electronic Engineering Design
- Digital Systems and Signal Processing
- Control and Communications
- Digital Systems Synthesis
- Embedded Processors
- Nanofabrication & Microscopy
- Microsensor Technologies
- Microfluidics & Lab-on-a-Chip
- Microfabrication
- High Voltage Insulation Systems
- Cryptography
- Wireless and Optical Communications
- Web and Cloud Based Security
- Signal and Image Processing
- Robotic Systems
- Real-Time Computing & Embedded Systems
- High Voltage Engineering
- Green Electronics
- Embedded Networked Systems
- Digital IC, Digital Control & Systems Design
- Digital Coding and Transmission
- Control System Design
- Analogue & Mixed Signal Electronics
- Optical Fibres
- Wireless Transceiver Design & Implementation
- Wireless Networks
- VLSI Systems Design
- Silicon Photonics
- Secure Hardware and Embedded Devices
- Power and Distribution
- Quantum Devices and Technology
- Space Systems Engineering
- Engineering Design
- Electromechanical Energy Conversion
- Medical Electrical and Electronic Technologies
- GPS and its Applications
- Electronics for Spacecraft
- Power Systems Technology
- Guidance, Navigation & Control
- Radar Techniques & Applications
- Aerospace Electronics Design
- Flight Mechanics & Aerospace Systems Engineering
We have a track record of helping student achieve excellent academic result regardless of if they are GCSE (O-Level), A-Level, OND, HND, Bachelors, Masters, MBA or Ph.D. students.
We offer good competitive prices for our report writing services in comparison to other major websites out there. You can get a rough estimate of what your writing order will cost by clicking on the pricing calculator . We are also deadline driven, our team of study abroad consultants, academic researchers & writers, professional CV writing experts and tutors ensure that your work is delivered to you on time.
Our proofreading and editing services ensures that your work is structured the right way and rid of grammatical errors. We also provide comments and point you to relevant resources that would be helpful in improving the quality of your work.
We also help you craft concise, fit to use Curriculum Vitae (CV) for internship application, masters or PHD application as well as job application.
Our study abroad consultants can help you with your overseas university application to major european countries like Finland, Sweden, Estonia, Iceland, Denmark, United Kingdom, France & Germany. We can also help with applications to universities in Canada, Australia and the United States. Our process covers everything you need such as application form filling, CV writing, personal statement, motivational letter, visa application & reference letter review.
We offer free resources as well as paid resources which include past exam paper solutions, thesis proposals, dissertation proposals, past essays, past assignments solutions, past coursework solutions, full final year project, full dissertations, full thesis covering computer science, information technology, business management, mathematics, physics, biology, microbiology, geology, geoscience, geography, statistics, chemical science, education, medical science, biomedical science, biochemistry, health & social care, economics, sociology, psychology, philosophy, mechanical engineering, acoustical engineering, mechatronics engineering, civil engineering, aerospace engineering, electrical/electronics engineering, chemical/petroleum engineering, history, political science, english literature and law.
After several years of experience with offices in three countries; United Kingdom, Nigeria and Sri Lanka you can bet on our experience to deliver excellent piece of work.
Get Started
Request quote.
Submit the word you see below:
Work Samples
See for yourself.
Take your success to new heights with AcademicianHelp.

Dissertation - An Investigat…

Dissertation - An investigat…

Dissertation - Spam Detectio…

Business Intelligence Tools:…

An Investigation into the i...

Student Accommodation System

Skeleton Argument ...
Frequently asked questions, have a question.
First look at these three.
Click below to get answers to your questions.
Wellawatte, Colombo 06, Sri Lanka
+94786798715, [email protected], find out how much your order will cost., price calculator, call +94786798715 for more information.
We are an innov
Deadline (Days)
Price: 40 gbp.
- Staff Login
- Student Login
- Hotline : +94 763216802
- Reg. No : CPC/KY/DS/5/2/6938
assignment.lk
Assignment writing services.
Assignment.lk offers a professional writing service in Sri Lanka through a dedicated writing unit who has vast experience in writing PhD, MBA, SLIM & HND Assignments to vanish all assignment worries & assignment writing anxieties of Sri Lankan students!
On time delivery
We deliver your assignment works on time & it’s 100% guaranteed.
Confidential
Assignment.lk will not reveal the details of our valued customers to any third parties and it’s 100% guaranteed.
Plagiarism free
All our Ph.D., MBA, CIM & HND assignment works guaranteed 100% plagiarism free
Satisfaction
Our top priority has given to our customer’s satisfaction & each assignment comes with professional proofreading & unlimited revisions.

ABOUT assignment.lk
Since 2008, we have developed as a global provider of custom written assignments for the students to eliminate all their assignment writing anxieties while assisting them towards a brilliant future.
We pride about ourselves for having a dedicated & the best qualified in-house team....
Reg No: CPC/KY/DS/5/2/6938
Copyright © 2008 - 2018 - assignment.lk is a trading name of Liovision Group which is the oldest and the largest registered academic writing group in Sri Lanka. Registration No: CPC/KY/DS/5/2/6938.

Professional Assignment Help for Sri Lankan Students

Ph.D., MBA, SLIM & HND Assignment Writers/Help in Sri Lanka

Our MBA academic writers on your assignment help

Privacy concerns on our assignment writing service

What do we expect to deliver for Sri Lankan students?

Our products
- PhD dissertation
- MBA / MSC Assignments
- HND / HNC Assignments
- CourseWork / Term Paper
- Proofreading/Editing
- Memorable dissertation

Our Unique Features
- All papers are custom-made
- 150+ Academic Writers
- Discounts & Special offers
- 100% Privacy Guarantee
- 24x7 Service
- Plagiarism Free(Below 9%)

- Professional Level

our Strength
- Course Category 25+
- Writers: 150+
- Establish :07/04/2008
- Sales : 12,000+
Copyright © 2016 - All Rights Reserved - assignment.lk
Website by Target

BEST ASSIGNMENT WRITING SERVICE
Highly qualified, experienced academic experts committed writing up your assignments guaranteeing you on time delivery and high quality work., why bestassignments.lk.
We believe in both working smart and working hard, most importantly we believe in balanced life. This is why BestAssignments.lk steps in to help students and employees to achieve their bigger dreams while enjoying a balanced life.
“Your job is to learn, our job is to write”

Meet Deadlines Always
- On time delivery
- No more repeats or paying late submission fees.

Plagiarism free
- We got the best writers and the best software.
- We write smart, we deliver fast and we guarantee best quality
- Now you also can get your Plagiarism report attached.

100% Confidential
We respect our customers and their profession therefore we will not reveal your information to any third parties under any circumstances.

Best Quality Guaranteed
Our top priority is the quality of our work and customer’s satisfaction. Our team is full of qualified professionals, experienced academic writers from various industries. Therefore we shall not compromise the quality of our work under any circumstances.
Attachments
You will get a confirmation email with the quotation with-in 24 hours your writer will start working as soon as you make your advance payment. free revision will be subject only up to 03 days after delivery, for you to check your paper and request for minor revisions under the same framework submitted. you can either download on your profile at bestassignments.lk also we will email you the completed work on or before the due date..

PHD/ DBA/ Msc/ MBA Dissertations
MBA/Msc/ HND/ SLIM/CIM Assignments
Case studies/ Research papers, PPT
Business Management
Business Psychology
Tourism & Hospitality
Human Resources
Project Management
Strategic Management
Information Technology
Our Qualified Team
Our qualified team of writers are members of the alumni of these prestigious Universities, which gives you the assurance and confidence of the standard quality of our writing.

How to Avoid Plagiarism and AI Detection on Turnitin
Write Your University Assignment like a Pro Avoid plagiarism and

Assignment types we offer
We Offer variety of Writing services! At Bestassignments.lk, we take

FAQ of Bestassignments.lk – Leading Assignment Outsourcing Company in Sri Lanka
FAQ of Bestassignments.lk Welcome to the FAQ section of Bestassignments.lk!

Subject areas covered by Bestassignments.lk
Accounting Financial Accounting Financial Analysis Management accounting Auditing Accounting Information

- NSF at a glance
- Organizational Structure
- Board of Management
- Director General
- Additional Director
- Employee Guide
- NSF Booklet
- Annual Reports
- Manuals & Procedures
- Strategic Plan 2024 - 2028
- Organizational Transformation
- Audit Committee
- Staff Directory
- Research Division
- Technology Development and Innovation Division
- Science & Technology Policy Research Division
- Science Communication and Outreach
- International Affairs Division
- Journal Publication Division
- Library & Resource Center
- Supporting Divisions
- Competitive Research Grants (CRG)
- Technology Grants
- International Collaborative Research Programme (ICRP)
- International Partnerships for Science and Technology Programme (IPSAT)
- National Thematic Research Programme (NTRP)
- Gap-Filling Research Grants Scheme (GAPF)
- Spare Part Grants for Research Equipment (SPG)
- Research Equipment Grants (EQ)
- Support Scheme for Scientific Meetings & Events (SSSME)
- Support Scheme for Publication Fees (SSPF)
- Science Education and Popularization Programme (SEPP)
- Science and Technology Publications Grants Scheme (STPGS)
- Research Scholaships
- Postdoctoral Research Fellowships (PDRF)
- International Travel Grants
- Overseas Special Training Programme (OSTP)
- Overseas Science Education programme (OSEP)
- Support Scheme for Supervision of Research Degrees (SUSRED)
- National Awards for Science & Technology Achievements (NASTA)
- NSF Research Awards
- NSF Technology Awards
- School Science Societies (SSS)
- Science Research Projects Competition (SRPC)
- School Science Competitions (SSC)
- Overseas Science Education Programme (OSEP)
- For Community
- University Science Societies (USS)
- Science Education (OSEP)
- Media Releases
- Journal of the National Science Foundation of Sri Lanka (JNSF)
- Sri Lanka Journal of Social Science (SLJSS)
- R & D Statistics
- Newsletter “Vidya”
- Reports, Booklets & Monographs
- Policy Briefs
- Conference Proceedings
Strengthening National Research, Development and Innovation Eco-System

The National Science Foundation (NSF) of Sri Lanka plays a pivotal role in supporting and strengthening the National Research, Development, and Innovation Ecosystem to promote wealth creation and ensure the wellbeing of the citizens of Sri Lanka. NSF, as a key government organization, has designed its programmes and initiatives to contribute to this endeavor at three different levels as shown below.
- Individual Level
- Institutional Level
- National Level
- Science Research Project Competition (SRPC)
- School Science Competitions
- Kids Naturalists
- Research Scholarships (SCH)
- Technology Development Grants (Tech D)
- Startup Grants on novel technologies (Startup)
- Gap Filling Grants (GapF)
- Sri Lanka Journal Online (SLJOL)
- Digital Science Library
- International Travel Grants (ITG)
- Participation at local Conferences, Seminars and Workshops- CRG miscellaneous vote
- Journal of the National Science Foundation (JNSF)
- Sri Lanka Journal of Social Sciences (SLJSS)
- Science Education and Popularization Programmes (SEPP)
- Publication Grant Scheme for S & T Publications (PGS)
- Global Digital platform (GDP)
- Science and Technology Management Information System (STMIS)
- National Instrument Database (NID)
- Research and Technology Grant database (RTGra)
- Support Scheme for Supervision of Research Degrees Awards (SUSRED)
- Technology and Innovation Support Centre (TISC)
- Training workshop
- Public-Private/Public-Partnership Research Grants (PPP)
- Research Equipment Spare part grants (SPR)
- Support schemes for scientific meetings and events (SSSME)
- International Collaborative Research Programme (ICRP): MOU with National Natural Science Foundation (NSFC) China, Pakistan Science Foundation (PSF), and Brazil Government
- International Partnership for Science and Technology (IPSAT)
- Man and the Biosphere Programme (MAB)
- Science Engineering Technology and Innovation Policy Asia and the Pacific Network (STEPAN)
- Global Research Council (GRC)
- Global Research Alliance on Agricultural Green House Gases (GRA)
- International Centre for Genetic Engineering and Biotechnology (ICGEB)
- International Council for Science (ICS)
- The World Academy of Sciences (TWAS)
- United Nations Educational, Scientific and Cultural Organization (UNESCO)
- Federation of Asian Biotech Association (FABA)
- Science Council of Asia (SCA)
- International Union of Biochemistry and Molecular Biology (IUBMB)
- Asia Pacific Advanced Network (APAN)
- Association of Asian Social Science
- Research Councils (AASSREC)
- Sri Lanka Science and Technology Institute Network (SLSTINET)
- NSF e-repository
- S&T Statistical hand Book
- Research Programme on Health Science (RPHS)
- Special Project on Cinnamon (SPC)

WHO ARE WE?
We are a company based in sri lanka with the team of expert writers in academic writing from countries around the globe. we provide legitimate and 100% trusted writing services in sri lanka. we offer services including assignment writing, dissertation writing, essay writing, proposal writing, presentations, thesis writing, proof reading, web copy writing, editing, sop writing and all other content writing services in sri lanka for students around the world., what we do.

Assignments
We provide all levels of assignment writing service in Sri Lanka in all the subjects for all grades and Levels.

We have best academics and specialists to provide you highly professional and excellent grade Thesis writing service in Sri Lanka.

Proofreading
We offerhigh quality academic and professional proofreading service in Sri Lanka with the team of experts and exeperienced academics.

SOP Writing
Statement of Purpose Writing in Sri Lanka for all types of visas and countries by qualified and experienced immigration experts.

We provide professional winning CV writing and personal statements for focused jobs with high-end designing options for all professions.

Copy Writing
Copy Writing for web contents and pages with excellent success rate from the team of globally experienced and qualified writers.
Contact Us Today
0777650323 [email protected], there is no big shame than failing an assignment or delaying the graduation. speak to our friendly and discrete staff and get your assignments done in no time from the most legitimate and highly professional assignment writing service provider in sri lanka., explore the ocean of the subject areas we cover.
Management Assignments
Accounting & Finance
Accounting Assignments
General Subjects
General Subjects Assignments
IT & Computing
IT Assignments
Law Assignments
Engineering
Engineering Assignments
Science Assignments
Humanities Assignments
Why Choose Us?
100% genuine and unique writing, qualified and experienced scholars, plagiarism-free with turnitin reports, all subjects.. all levels.. all modules, timely delivery, 100% confidentiality guaranteed, free revisions and reworks, competitive prices and unbelievable bulk discounts, accurate formatting and referencing, professional handling and best support.
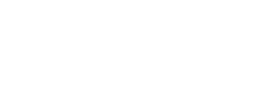
- FORMER CHAIRMEN
- FORMER COUNCIL
- PPP PROGRAMME
- TARGET ORIENTED
- RAPID RESPONSE
- SEARCH AWARDS
- MERIT AWARDS
- PROCUREMENT 2018
- PROCUREMENT 2019
- ALL EQUIPMENT
- CONTACT STAFF
- CONTACT NRC
- Search for: Search Button
- Investigator Driven Research Grants
Introduction
The NRC provides funds for Scientific Research Projects. Grants are open to any researcher of a Public R & D organization in Sri Lanka.
Public R& D organizations are the National Research Organizations, Universities and Affiliated Colleges and any governmental and semi-governmental organization where a research option exists in the mandate.
The Research Grants are advertised annually, generally at the beginning of the year and are evaluated by the Council. The evaluation criteria will include the scientific aspects, the relevance of the study to national development, its contribution to strengthening the capacity of science and technology in the country, and the possibility of research findings being published in international journals.
For the proposals selected, the Council will decide on an appropriate allocation of funds which will be channelled from the Treasury directly to the Principal Investigator, who will be solely responsible for implementing the project. Funds are considered for equipment, consumables, scientific literature.
The success of a grant is measured by international publications in referred journals, where the publications are judged by the most competent international scientists. This is to ensures that the research carried out is on par with international standards, and also to encourage our scientists to reach such high standards.
Grants Funded
Medical sciences / food & nutrition.
| Grant No | Title | |
| 16-001 | The Genetic origin (s) and distribution of the sickle cell gene and the clinical description of the sickle cell disease in Sri Lanka | |
| 16-023 | A population genetic study of 12 X-STR loci in Sri Lankan population and its applicability in forensic and kinship analysis purposes | |
| 16-024 | Dating violence among undergraduates in Western Province: Magnitude, types, associated factors and effectiveness of an intervention in reducing violence | |
| 16-044 | A novel ultrasound technique to detect early chronic kidney disease | |
| 16-052 | A brief intervention for prevention of non-fatal self- poisoning delivered primary care nurses -a randomised controlled trial | |
| 16-080 | Sero- prevalance of anti-varicella IgG and factors associated with immunity in pregnant mothers attending antenatal clinics of De Soyza Maternity Hospital, Sri Lanka | |
| 16-086 | Cost-effectiveness of three approaches to hysterectomy for benign uterine conditions: a multi centre randomized controlled trial | |
| 16-142 | Establishment of insectary facilities for the maintenance of potential leishmaniasis vectors and study on systematics, biology and bionomics of sandflies in Sri Lanka |
| Grant No | Title | |
| 17-008 | Risk assessment of foodborne pathogens in food commodities available in the Sri Lankan market and application of biocontrol measures to ensure food safety | |
| 17-020 | Mutations and polymorphisms of mitochondrial genes as risk factors for sporadic breast cancer in Sri Lankan patients of Sinhalese ethnicity | |
| 17-029 | Development of an antidiabetic agent from Coccinia grandis (L.) Voigt (Cucurbitaceae) for diabetes mellitus | |
| 17-042 | Insight for molecular Anthropology of early people in Sri Lanka: Ancient human mtDNA and Molecular sex analysis of archeological skeletal remains at Udupiyangalge and Alugalge caves | |
| 17-055 | Molecular characterization of carbapenemase producing enterobacteria (CPE) isolated from a tertiary care teaching hospital in Sri Lanka & validation of a rapid CPE detection protocol | |
| 17-086 | The steroid profile of follicular fluid in In Vitro Fertilisation (IVF) treatment cycles with a standard controlled ovarian stimulation GnRH antagonist regimen and with adjuvant of Letrozole among women with polycystic ovary syndrome and non-PCOS, and its relationship with oocyte number, quality, fertilisation rate and implantation rate. | |
| 17-098 | Detection of genotypes and serotypes of Leptospira isolated from severe leptospirosis patients |
| Grant No | Title | |
| 18-008 | Islandwide study on Scrub Typhus genotypes, their clinical features, Biochemical markers of severity and transmitting vector species | View More |
| 18-030 | Foetal haemoglobin induction as a treatment for β-thalassaemia | View More |
| 18-035 | Effectiveness of an intervention to introduce reading skills to school children with features of dyslexia in the Gampaha District in Sri Lanka; a randomized clinical trial | View More |
| 18-057 | Novel and Innovative Strategies to Control Anopheles stepheles stephensi and other malaria vectors for prevention of reintroducation of malaria in Sri Lanka | View More |
| 18-079 | Isolation and identification of environmental Burkholderia pseudomallei and comparative analysis of major virulent associated genes from clinical isolates of infected Sri Lankan Melioidosis patients | View More |
| 18-080 | Developing and validating a speech sound (articulation and phonology) assessment for Sri Lankan Tamil-speaking children aged 3 to 6 years | View More |
| Grant No | Title | |
| 19-006 | Examination of the state of food literacy education and food environment in Sri Lankan secondary schools | |
| 19-028 | Identification and characterization of etiological agents of brugian filariasis in Sri Lanka and their vectors | |
| 19-030 | Genetic analysis for predictive markers for hepatocellular carcinoma (HCC) in non-alcoholic steatohepatitis (NASH) related cirrhosis | |
| 19-050 | Comprehensive biochemical and molecular analysis of patients suspected with inherited hemolytic anemia in Sri Lanka and assessment of its contribution to anemia burden in the community | |
| 19-065 | Development of a colourimetric reverse transcription Loop-mediated isothermal amplification (RT-LAMP) assay as a cost-effective, novel surveillance tool for differential detection of dengue serotypes in Aedes mosquitoes | |
| 19-089 | Analysis of multidrug resistant Extra intestinal Pathogenic Escherichia coli clones in humans and animals in Sri Lanka and determine the potential of developing a vaccine to eliminate the clones | |
| 19-099 | A “One Health” approach: the epidemiology of methicillin-resistant Staphylococcus aureus isolated from humans, animals and animal products in southern Sri Lanka |
| Grant No | Title | |
| 20-066 | An attempt to in vitro differentiation of human round spermatids into mature spermatozoa (spermiation) | |
| 20-073 | Investigation and characterization of hantavirus infection in selected Districts and enhancement of hantavirus diagnostic facilities in Sri Lanka. | |
| 20-078 | Clinico-epidemiology, coagulation profile and the phylogenetic positioning of Saw-scaled viper in Northern Sri Lanka. | |
| 20-083 | Canine tick borne infections: reservoirs, tick vectors and zoonotic disease risk of rickettsial infections | |
| 20-118 | PCR-based molecular evaluation of intestinal parasitic infections among school children in Anuradhapura, Sri Lanka. | |
| 20-005 | Epidemiology and molecular diagnostics for acute undifferentiated febrile illness in Sri Lanka |
| Grant No | Title | |
| 22-003 | Association of maternal BMI and gestational weight gain with cord blood DNA methylation, adipokine levels, offspring anthropometry, early childhood cardio-metabolic parameters and the effect of lifestyle modification on growth during infancy | |
| 22-011 | A Comparison of the Degree of Platelet Inhibition in Sri Lankan Coronary Artery Disease Patients on Clopidogrel and Ticagrelor | |
| 22-027 | Transcriptome analysis of mycobacteria in serum exosomes of latent tuberculosis patients for candidate biomarker identification. | |
| 22-031 | Fourier transform infrared (FTIR) spectroscopy and, metabolomic screening with gene expression profiling of body fluids for early detection of Oral squamous cell carcinoma (OSCC). | |
| 22-044 | Detection and validation of molecular abnormalities in bone marrow aspiration samples obtained from patients with myelodysplastic syndrome using an “inhouse” developed bone marrow transport medium | |
| 22-075 | "The use of PGE1 in patients with non-revascularizable Chronic limb threatening Ischaemia- randomized study" |
Agriculture / Plantations / Livestock & Fisheries
| Grant No | Title | |
| 16-016 | QTL map based candidate gene discovery for salt tolerance in rice (Oriza sativa) | |
| 16-025 | Studies on thermotolerant acetic acid bacteria from Sri Lanka and production of fermented healthy non-alcoholic beverages | |
| 16-033 | Assesment of behavioural and reproductive responses of coconut mites to coconut varieties and relationship of volatile organic compounds, lipid profiles and phenolic compounds of coconut varieties with their susceptibility levels to coconut mite | |
| 16-038 | Identification of reliable method for laboratory diagnosis of tuberculosis using nasopharyngeal swabs and saliva of PPD positive cattle and buffalo | |
| 16-054 | Investigation on ecological and socio- economic impacts of bamboo (Bambusa bambos L. Voss ) in dry zone forests in Sri Lanka | |
| 16-071 | Characterization and purification of bacteriocin produced by lactic acid bacteria isolated from natural fermented food products | |
| 16-075 | Developing botanical nitrification inhibitors to reduce nitrogen fertilizer wastage in vegetable crop cultivation |
| Grant No | Title | |
| 17-010 | Analysis of pesticide residues and evaluation of some beneficial effects along with farmer perception of an eco-friendly crop management package for chilli and tomato in comparison to existing commercial cultivation practices conducted in Sri Lanka | |
| 17-011 | Development of baseline soil information system for soil C and other nutrients for paddy growing soils in Sri Lanka | |
| 17-017 | Rapid multiplication and Production of Agarwood Fragrant Constituents by Plant Cell and Tissue Culture of Gyrinopsis walla | |
| 17-038 | An automated system to quality control the fermentation stage in black tea manufacturing process | |
| 17-058 | Temporal variation of cyanobacterial community in fertilized and long-term unfertilized tropical rice fields |
| Grant No | Title | |
| 18-009 | Genetic diversity and cultivar development of Dendrobiums integrating classical and molecular biological tools | View More |
| 18-012 | Investigation of aetiology, disease development and management of rough bark disease of cinnamon (Cinnamomum zeylanicum Blume) | View More |
| 18-084 | Identification of drought tolerant coconut mother palms through phenotypic, physiological and gene expression studies | View More |
| 18-088 | Effect of priming of rubber (Hevea brasiliensis) plants with some natural or chemical compounds on growth and abiotic stress alleviation under sub-optimal climatic conditions in Ampara District of Sri Lanka | View More |
| 18-091 | In-silico mining for resistance gene analogs and identification of genetic resources for blast disease resistance in the local finger millet germplasm | View More |
| 18-094 | Extraction, purification and chemical characterization of inulin-type fructans from three Asparagus species (A. falcatus, A. racemosus, and A. officinalis) grown in Sri Lanka, and their utilization as potential prebiotic ingredients in dairy products. | View More |
| EWC 18-002 | Use of Artemisia vulgaris (L) as an eco-friendly and economically-viable component in integrated management of weeds, insect and mite pests and nuisance pests in tea fields of Sri Lanka | View More |
| EWC 18-003 | Microbial metabolites - a source for development of eco-friendly new weedicides | View More |
| EWC 18-004 | Development of eco-friendly integrated weed management system for rice farming | View More |
| EWC 18-005 | Investigations on eco-friendly cultural , physical and allelopathic weed management strategies for tea cultivation as alternatives for synthetic herbicides | View More |
| Grant No | Title | |
| 19-052 | Enhancing soil fertility in degraded rubber lands by combine use of agro management practices such as inorganic fertilizer, biofertilizer, cover cropping and mulching with organics | |
| 19-054 | Investigation of cultivar dependent dynamics of seed metal ion content and identification of prospective genetic candidates for nutritional quality improvement in Sri Lankan rice germplasm | |
| 19-061 | DNA Barcoding, Morphological Taxonomy and Phylogeny of Syzygium spp. of Family Myrtaceae in Sri Lanka: Implications for Conservation and Sustainable Exploitation | |
| 19-062 | Genetic diversity and relationship among agronomically locally adapted black pepper (Piper nigrum) accessions from selected localities in Sri Lanka and their endophytes, applied to biotic stress tolerance and growth promotion | |
| 19-072 | Determination of the variation of soil carbon dynamics and soil physico-chemical properties in tropical rainforests and tropical montane forests in Sri Lanka across an altitudinal gradient | |
| 19-076 | Development of irradiated multivalent chicken coccidial oocyst vaccine in Sri Lanka in order to minimize drug residues in poultry products | |
| 19-095 | Characterization of proteins from underutilized Sri Lankan seaweeds and application as protein alternatives in bakery foods |
| Grant No | Title | |
| 20-010 | Shift in species composition and diversity of bee pollinators and natural enemies while enhancing crop yield in a highly dynamic agro-natural landscape | |
| 20-022 | Study of some postharvest disorders of guava, mango and avocado and their management | |
| 20-079 | Evaluation of feed efficiency and meat quality parameters of slow growing (label rouge) pasture raised chicken | |
| 20-123 | Conservation and Utilization of Old Seedling Teas: A Viable Option for Adaptation to Climate Change | |
| 20-128 | Engineering Microbial Ecology in Agroecosystem via Bio-encapsulation of Microbial Communities to Improve Soil Health and Fertility | |
| 20-115 | Effects of environmental fluoride, hardness and heavy metal (Cd, Pb, As) exposures to the cow milk and their kidney function in CKDu endemic areas of Sri Lanka | |
| 20-079 | Evaluation of feed efficiency and meat quality parameters of slow growing (label rouge) pasture raised chicken | |
| 20-109 | Control of stored-product insects using biorational methods | |
| 20-012 | Identification and characterization of major pathogens in grape cultivation and improving the grape production by managing major diseases through ecofriendly control measure | |
| 20-098 | Investigation of crop water usage and soil hydrological dynamics of oil palm (Elaeis guineensis Jacq.) and rubber (Hevea brasiliensis Muell. Arg.) plantations in the low country wet of Sri Lanka |
| Grant No | Title | |
| 22-062 | Assessment of species diversity, anti-phytopathogenic activities of crude extracts and in vitro growth performances of marine macroalgae in Sri Lanka | |
| 22-104 | Identification and characterization of phytotoxic metabolites of actinomycetes; candidates for the development of an eco-friendly tool for sustainable weed management | |
| 22-131 | Design and Implementation of Microenvironment Conditions for Tea and Ornamental Foliage Plants using Precision Agriculture Systems Powered by Solar Photovoltaics | |
| 22-036 | Assess the suitable conditions for sustainable and environmentally friendly aquaculture of the sea cucumber Holothuria scabra (sandfish) in northern Sri Lanka. |
Engineering Technology / IT / Physical Sciences
| Grant No | Title | |
| 22-041 | Slope surface stabilization by using polymer modified microbial induced carbonate precipitation method – Ecofriendly and sustainable alternative approach for the conventional cement grouting | |
| 22-047 | Colloidal dispersions of cellulose nanostructures from sustainable raw materials and their applications in packaging industry | |
| 22-053 | Cinnamon essential oil nanocapsules incorporated starch based food packaging with antimicrobial properties. | |
| 22-060 | Development of novel value-added forms of processed cinnamon through automation | |
| 22-070 | Development of a computational model to simulate fate and transport of accidental oil spills for Sri Lankan territorial waters and maritime zone |
| Grant No | Title | |
| 17-006 | Value addition to Sri Lankan natural rubber in the field of Power and Energy | |
| 17-018 | Design and Development of a Soft Orthotic Device for Lower Limb and Spinal Assistance | |
| 17-019 | Launching a Greenhouse Gas Emissions Technology Evaluation Center (GRETEC) | |
| 17-047 | Optimization of Shear Retrofitting of RC beams via Non-linear Numerical Analysis | |
| 17-060 | Adaptation of Mechanistic Pavement Design Guide for Road Designed based on Empirical Design Methods. | |
| 17-064 | Improving effectiveness of Massive Open Online Courses (MOOCs) to meet the 21st century challenges | |
| 17-065 | Adaptive Protection of Microgrids Using Graph theory and Optimization algorithms | |
| 17-066 | Ecological rehabilitation of canals in Colombo: a design to harmonize flood control and physical heterogeneity | |
| 17-069 | Intelligent wheelchair robot with human like interactive features for domestic environments |
| Grant No | Title | |
| 18-005 | Copper zinc tin sulfide (CZTS) Photovoltaic – Thermoelectric hybrid system for the fabrication of efficient solar energy conversion devices | View More |
| 18-007 | Fabrication and analysis of super capacitors with low cost composite hybrid electrodes to meet the future energy challenge | View More |
| 18-028 | Design, analysis, and optimization of next generation fiber optic national backbone networks | View More |
| 18-043 | Impact of Increasing Renewable Energy Developments on the Reliability of Power Generating Systems | View More |
| 18-044 | Development of a Soft Robot Gripper with Inbuilt Sensors for Deformable Object Grasping and Tactile Feedback | View More |
| 18-077 | Modeling and description of compact astrophysical objects using Einstein’s field equations | View More |
| Grant No | Title | |
| 19-019 | Development of a model to simulate the sustainability of infrastructure using life cycle approach | |
| 19-023 | Synthesization of novel structural materials, mainly by CVD method, for the fabrication of high performance Li-ion hybrid supercapacitors | |
| 19-032 | Development of new Thermo-Electric (TE) materials for automobile heat recovery applications | |
| 19-040 | Development of a network of subsoil sensors and drones for crop surveilance | |
| 19-051 | Development of an environmentally friendly high efficient low cost Cu2O homojunction solar cell | |
| 19-060 | Conversion of natural and synthetic carbon based polymers to the conductive carbon nanomaterials by photonic, plasma and thermal treatments, and use them in possible electronic applications |
| Grant No | Title | |
| 20-108 | Development of a cooling system to reduce the temperature generation in conventional spice grinding machines through experimental investigation of the temperature distribution inside the grinding chamber of conventional spice grinding machines | |
| 20-124 | Determination of Optimum Characteristics of Feeder Service for a Public Transit Route | |
| 20-080 | Simulation of self-deployable structures made of ultra-thin shells | |
| 20-031 | Optimizing Wearable Triboelectric Nanogenerators for the Internet of Things (IOT) | |
| 20-107 | Investigation of the potential of microalgae cultivation in hybrid systems for carotenoids production under Sri Lankan climatic conditions | |
| 20-055 | Development of surface enhanced Raman spectroscopy (SERS) methods for in-situ detection of hazardous pesticides combined with portable technology |
Environment, Chemical Sciences/ Others
| Grant No | Title | |
| 16-029 | Impact of linear developments on ecology of wildlife with special reference to roads, railways and power lines in Sri Lanka | |
| 16-059 | Species diversity and the potential vector status of Ornithophilic mosquitoes in Sri Lanka | |
| 16-072 | Optimizing Dendrimer Architecture for Drug Entrapment | |
| 16-128 | Ecotourism in Coastal Wetlands: Meeting the Dual Mandates of Recreation and Conservation | |
| 16-129 | Investigation of the potential of employing indigenous microalgae for third generation biofuel production | |
| 16-144 | Phytoremediation of used lubricating oil contaminated soils by Impatiens balsamina L. and Crotalaria retusa |
| Grant No | Title | |
| 17-007 | Using Nano/micro-capsules for Self-healing Epoxy Composites | |
| 17-025 | Baseline concentrations, solubility and spatial variability of potentially toxic trace elements in soils in Up- and Mid-country Wet zone in Sri Lanka | |
| 17-027 | Taxonomic revisions of jumping spider subfamilies Ballinae and Spartaeinae of Sri Lanka based on morphology and DNA barcodes | |
| 17-028 | Igneous rocks in the Mannar Basin as potential evidence from Sri Lanka for the juxtaposition of the Reunion Hotspot and the impacts of the igneous rocks on the hydrocarbon exploration in the Mannar Basin. | |
| 17-033 | Combined therapeutic drug leads for antidiabetic and anti-hyperlipidaemic treatments from the selected combined medicinal plants. | |
| 17-037 | Investigation of Weathering and Erosional Processes in the Catchment of the Ma Oya Tributary of the Mahaweli River | |
| 17-054 | Bioactive metabolites of endophytic fungi from the medicinal plants Coccinia grandis, Costus speciosus and Gymnema sylevestre used in indigenous medicine for treatment of diabetes mellitus and possible commercial applications | View More |
| 17-072 | Evaluation of structural, rheological and mechanical properties of ternary composites of filled Thermoplastics (TP) and Skim Natural Rubber (SNR) blends: a novel route for value addition to skim natural rubber | View More |
| 17-074 | Molecular phylogeny of marine macro algae (sea weeds) present in Sri Lankan coasts and isolation of anti-cancer compounds to target oral cancers from marine macro algae | View More |
| 17-094 | Avian feathers as bioindicators of exposure to toxic trace elements and links between trophic position, genetic diversity and reproductive success | View More |
| 17-095 | Seed storage behaviour of fifty keysone rainforest species from Sri Lanka: Towards Conservation of Biodiversity | View More |
| Grant No | Title | |
| 18-013 | Transdermal drug delivery via smart textiles: Development of new formulations for the controlled release of natural compounds to prevent cancer | View More |
| 18-032 | Production of Mosquito Repellents using Lesser-Known, Under-Utilized Volatile Oil Producing Plant Species | View More |
| 18-050 | Cardioprotective effect of three medicinal plants against doxorubicin induced cardiotoxicity in Wistar rats and in neonatal ventricular cardiomyocytes | View More |
| 18-063 | Absorption of selected pesticide residues during cooking by curry leaves available in Sri Lanka and its impact on the carotenoid compositional variation in curry leaves | View More |
| 18-066 | Understanding exposure levels of volatile organic compounds and fine particulate matter while commuting in Kandy city | View More |
| 18-083 | Development of a phototrophic-heterotrophic biofilm/mat for the detoxification and removal of Chromium in waste water. | View More |
| Grant No | Title | |
| 19-005 | Supplement effect of Cherukurinja (Gymnema lactiferum) on glycemic control and on selected biochemical and physiological parameters among patients with Type II Diabetes Mellitus | |
| 19-007 | Development of Nutritious and healthy food corners for the children / adolescences | |
| 19-024 | Synthetic Biology approaches for the synthesis of strictosidine derived anticancer compounds | |
| 19-033 | Evaluation of potential health enhancing properties of edible flowers available in Sri Lanka | |
| 19-046 | Efficacy and welfare of Aversive Geofencing Devices for managing the movements of Asian elephants | |
| 19-058 | A needs assessment study of young and mid-career academics in Sri Lankan Universities aiming at evidence-based decision making | |
| 19-064 | Fabrication of Intelligent Textile Garment for Diabetes Patients with Features of Blood Glucose Sensing, Monitoring, Data storage and Drug Delivery Systems combined with a mobile app | View More |
| 19-075 | Bioethanol production from marine algae | |
| 19-081 | Analyzing the phylogenetic relationships of Sri Lankan Agamid Lizards to facilitate their conservation | |
| 19-090 | Synthesis of modified Zeolite for catalytic converting and removal of NOx, SOx and CO from the vehicle exhaust | |
| 19-092 | Petrogenesis, geochemistry and potential of economic mineralization of granitic pegmatite in Sri Lanka | View More |
| Grant No | Title | |
| 20-014 | A stable composite based on titanium dioxide and clay as an effective photocatalyst for wastewater treatment | |
| 20-117 | Microplastics Bound Transport and Differential Bioavailability of I Pharmaceuticals, Personal Care Products (PPCPs) and Toxic Trace Elements in Water | |
| 20-086 | Determination of Descriptor Values for Selected Volatile Constituents in Cinnamon, in order to Determine their Distribution Levels in Environmental Compartments | |
| 20-085 | Household Food Waste Behaviors and Implications for Food Security and Environmental Sustainability in Sri Lanka. | |
| 20-074 | Characterization of a composite flour from Kithul (Caryota urens) and arrowroot (Marantha arundinacea) flour with different modifications to widening its applications in food industry. | |
| 20-007 | Investigation of the potential use of bryophytes as climate change indicators | |
| 20-039 | Tunable biodegradable polymers and polymeric nanocomposites from locally available renewable sources | |
| 20-051 | Characterization of bioactive pigments of mangrove-associated bacteria and screening for their potential biotechnological applications | |
| 20-110 | Transition metal chalcogenide embedded TiO2 nanocomposites for Hydrogen energy production and environmental remediation under extended solar irradiation | View More |
| 20-089 | Fine-Tuning Electronic / Semiconductor Properties of an Iso-reticular Metal Organic Framework Series to be Applied in Dye-Sensitized Solar Cells | |
| 20-111 | Selected Transition metals and Nitrogen co-doped Titanium dioxide electrode for Dye Sensitized Solar Cells | |
| 20-104 | Development of pH- and esterase-responsive β-cyclodextrin-adamantane inclusion-based biodegradable novel supramolecular network towards the fabrication of hydrogel for the controlled drug delivery | |
| 20-038 | Assessment of Endocrine Disrupting Potential of Industrial Effluents and Surface Water of Kelani River using Bioanalytical Tools | |
| 20-047 | Investigation of the detection of bacteria in water and food samples using bioconjugated fluorescent nanoparticles |
| Grant No | Title | |
| 22-095 | Developing ecological tools for monitoring river health using bio-indicators: A case study from Walawe River basin | |
| 22-101 | Cryptogamic epiphytes as indicators of successional changes in tropical lowland rainforests in Sri Lanka | |
| 22-114 | Mechanochemical synthesis of urea cocrystals as a sustained release nitrogen source | |
| 22-127 | Preparation of electrically conductive magnetic toner powders from Sri Lankan graphite and iron ores |
.png)
ECONOMIC RES EARCH FOR THE BOARD ROOM
Time is our most precious resource. We believe in work that enables people to live better by using their time better.
For our team, this means enabling them to engage in fulfilling work at times that are best suited for them, in a flexible work environment.
For our clients, this means getting them the information that matters most to them in less time,through time efficient research and information services.
Our Services
.png)
We currently offer macroeconomic advisory mainly in the form of presentations and reports, sectoral insights and information curations services.
Our online reports service, Frontier Athena, allows clients to easily access our work from anywhere, at any time, through a user-friendly platform.

The Frontier Way
At Frontier, we support choice and believe in building a culture of trust among all our stakeholders. We are strongly independent, encourage entrepreneurship, facilitate a learning environment, value open and honest communication, support progressive diversity in culture, and are driven to inspire purpose.
Frontier Team
Founded by economist and entrepreneur, Amal Sanderatne, our team comprises of diverse young individuals with a knack for the industry and a thirst for knowledge carrying forward a legacy of curiosity, independence and respect for time of all our stakeholders.

We are looking for self motivated lateral thinkers who can work independently on research projects that offer our clients with a different approach to assessing opportunities and risks. We are interested in people with a curious mind who like to question the norm.


- What Clients Often Ask

Looking for a research agency
Leading market research companies in sri lanka.
Sri Lanka’s most experience market research company, with an extremely dedicated market research team of qualitative and quantitative researchers, data analysts, and skilled data collection peoples. We conduct any type of qualitative and quantitative Market Research project in Sri Lanka.

Need a market research on your product
One of the best research firms in sri lanka.
You have found TK research firm, a research firm in Sri Lanka with a digit firmly on the beat of ever-changing attitudes, behaviors and social trends across Sri Lanka. The benefit of working with a research firm in Sri Lanka is you will eventually feel the rich insights, shocking answers, strong direction and a clear vision.

Result given research firms
Hire the best research agencies in sri lanka.
Our research agency people are outstanding, mostly because we love what we do. We have a solid track record in carrying insights, knowledge and skill in many categories although our analytical, performance and communication skills are some of the best in the research agencies in Sri Lanka.

Creative market research agency
Best market research company in sri lanka.
Expert at calculated thinking and analysis, we plan research to supplement accessible data sources and figure a comprehensive picture. Innovative, flexible and agile, our market research company in Sri Lanka personalized solutions that influences best-in-class methodologies, analysis tools and thinking.
Looking for market research companies in Sri Lanka
TK research is one of the best market research company in Sri Lanka. We are a full facility quantitative and qualitative market research fieldwork company dedicated in providing high-quality data collection and market research services. We are among the top market research companies in Sri Lanka for fetching problematic to reach audiences and excellence data collection, have in-depth knowledge and experience of applying appropriate procedures across a wide range of different businesses, geographies, and cultures.
Minimize risk
A market research in Sri Lanka will minimize the risk complicated in the business. It will support in setting up business with a possible of making huge profits.
Recognize clients
Know what client’s interest is and the products they avoid. When prepared with such data you will know the flawless products that can meet the present requirements of the market.
Exclusive strategies
Without a research firm in Sri Lanka, you cannot access grave realities that will permit you to brand unique strategies, most companies fail in this.
Value of decisions
By undertaking a market research in Sri Lanka, you find extra evidences concerning the market and the business. This expands the excellence of your choices.
Strategic planning
Strategic planning in a research agency is managing activity that is used to set priorities, focus energy and resources, strengthen operations towards common goals.
Improves communication
Market research increases current communication in corporate. The research will have you exposed to the requirement of those potential customers & ideas.

Our organization offers clients both qualitative and quantitative research methodologies while the primary area of our expertise can be listed as follows:
- Advertising and Brand Equity Research
- Brand Health Tracking
- Customer Satisfaction Research
- Retail Census and Retail Audits
- Retail & Shopper Insights
Need a market research proposal? Drop us an email to [email protected]
Customer research, monitoring & evaluation, marketing inspection.
Measure your brand presentation and get data on product awareness, usage, observation, trustworthiness and measure marketing success & customer performances. TK Research has the knowledge of buyer involvement management in businesses like retail, food, call centers, insurance, banks, airlines, hotels, oil, government and others.
Monitoring and evaluation are an important role in any project or business. We help in determining the effectiveness of campaigns in achieving their outcome objectives. The effect of campaigns could be from both the process and the outcome. The services we offer in this are questionnaire design and creation, training of field agencies, questionnaire scripting and data capturing.
Our marketing inspection package offers you with a total picture of what goes on at the goods. We can evaluate your products’ presentation at the trade end by reviewing accessibility, pricing, graphic brand obedience or elevations across your network. We also conduct brand presence and visibility via retail audit & candid evaluation to our clients.
Our Clients
TK Research & Solutions is a Colombo Based Market Research Agency, we are one stop solution for all your market research needs. We help our clients discover their true potential audiences across the world with our research experts.

© 2019 TK Research & Solutions (Pvt) Ltd. All Rights Reserved.
Sri Lanka Journal of Social Sciences


Sri Lanka - Science topic

- Recruit researchers
- Join for free
- Login Email Tip: Most researchers use their institutional email address as their ResearchGate login Password Forgot password? Keep me logged in Log in or Continue with Google Welcome back! Please log in. Email · Hint Tip: Most researchers use their institutional email address as their ResearchGate login Password Forgot password? Keep me logged in Log in or Continue with Google No account? Sign up
Special announcement
Study & research in sri lanka.
Are you interested in studying, researching or teaching in Sri Lanka? Have you thought about completing an internship or learning a foreign language abroad? Here you can find all the information.

Getting to Know the Country
Information on Sri Lanka
Here you will find information on scholarship programmes for study, teaching and research stays, university projects and scientific collaborations in Sri Lanka and more country-specific information. The information is only available in German.

Information for Academics in Germany
Study, Research & Teach Abroad
From planning to financing, here you will find all the necessary information on study-related stays abroad and scholarships for students, graduates and lecturers.

International Experiences
Studieren Weltweit
International study, research or work experience is increasingly in demand in the work place. The campaign "studieren weltweit – ERLEBE ES!" is designed to help young people understand of the benefits of a stay abroad.

DAAD Country Status
Higher and general education system and overview of DAAD activities
The DAAD country status offers a brief introduction to the education and academic system in Sri Lanka complemented by an overview of the DAAD activities on location. The following information is currently available in German only.
Advertisements by German Universities

M.Sc. in Cross Cultural Nursing Practice
You have a bachelor's degree in nursing and would like to gain further qualifications without losing touch with your patients? If you also have basic German language skills, our Master in Cross Cultur...

Apply to the TUM Global Postdoc Fellowship at Technical University of ...
The TUM Global Postdoc Fellowship is a funding opportunity for external postdoctoral scientists who are currently residing abroad and would like to start their research at TUM.
Get future-ready: Master’s in Water Management or Sustainable Textiles
You hold a Bachelor in Engineering? You are looking for an additional qualification with social, environmental and economic relevance? Get future-ready with our hands-on Master’s programs in Sustainab...

Truly international – Study at ESB Business School!
Do you want to study in the heart of Germany, Europe’s strongest and most dynamic economy? Come to ESB Business School at Reutlingen University!
DAAD Sri Lanka
DAAD Information Centre Colombo
Address: 15th Floor, 127 W A D Ramanayake Mawatha, Colombo 00200, Sri Lanka
PART I: Understanding Poverty in Sri Lanka

- Civil Society
- Education NGOs and CSOs
- Education Suppliers
- Government Agencies
- Independent Schools
- Other Organisations
- Research Institutes
- Universities
- Universities and Colleges
Research Institutes in Sri Lanka
There are numerous research institutes, higher education institutions and independent think tanks carrying out research into a wide range of fields and disciplines in Sri Lanka. Notable among these are the Institute of Policy Studies, who promote policy-orientated economic research and aim to strengthen policy-analysis capacity in Sri Lanka; the Coconut Research Institute of Sri Lanka which was founded in 1928, making it the first ever research institute devoted to the study of the coconut industry; and the Medical Research Institute of Sri Lanka who support research across the biomedical field to help achieve national health goals set by the Ministry of Health and to develop better health practices and services for the benefit of the Sri Lankan population. A website portal srilankaresearch.org provides a comprehensive database of scholarly journals and articles and information about Sri Lanka.
| Research Institutes organisations in Sri Lanka | |
|---|---|
- All member countries
- Our network:
- Commonwealth Education Online
- Commonwealth Governance Online
- Commonwealth Health Online
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- BMC Med Ethics

Understanding of research: a Sri Lankan perspective
Athula sumathipala.
1 Institute for Research & Development, Colombo, Sri Lanka
2 Institute of Psychiatry, Kings College London, UK
Sisira Siribaddana
Suwin hewage, manura lekamwattage, manjula athukorale, chesmal siriwardhana, kumudu munasinghe, kethakie sumathipala.
3 Department of Primary Care and Public Health Sciences, Kings College London, UK
Joanna Murray
Martin prince.
Lack of proper understanding on the part of researchers about public understanding of research and informed consent will increase the potential for malpractice. As a part of a larger study on ethics and informed consent in Sri Lanka, this study aimed to ascertain the level of understanding of 'research' by exploring the views of the public and professionals.
Convenience sampling and snow ball technique were used for recruitment with an emphasis on balanced age and gender representation, diverse educational, socio-cultural and professional backgrounds, and previous research experience, either as researchers or participants. Content analysis of the data was carried out.
66 persons (37 males, 29 females) participated. Although fundamentally a qualitative study, themes were also quantitatively analysed for informative results. Most participants thought that the word 'research' meant searching, looking, inquiring while some others thought it meant gathering information, gaining knowledge and learning.
A third of participants did not offer an alternative word for research. Others suggested the words survey, exploration, search, experiment, discovery, invention and study as being synonymous. Doctors, health professionals, health institutions, scientists, professionals, businessmen, pharmaceutical companies, students, teachers were identified as people who conduct research.
Participants indicated that crucial information on deciding to participate in research included objectives of the research, project importance and relevance, potential benefits to individuals and society, credibility & legitimacy of researchers, what is expected of participant, reason for selection, expected outcome, confidentiality and ability to withdraw at any time. A majority (89%) expressed their willingness to participate in future research.
Conclusions
The results show that with or without prior experience in research, participants in this study had a reasonable understanding of research. The findings show that a decision about taking part in research is dependent on knowledge, education and also on social networks.
The results demonstrate that the majority were supportive of health research and believe that research is beneficial to the welfare of society.
The international research community has debated and promoted the discussion on the issue of informed consent in human subject research [ 1 - 3 ]. However, a considerable gap in research literacy still exists between research participants and investigators [ 4 ]. This gap along with the authoritative position held by academics may affect the quality of informed consent as much as the desire to participate in research [ 3 ]. A lack of proper understanding on the part of researchers about what the public understand by research and consent processes will only widen this gap, increasing the potential for malpractice in conducting research and intentional or unintentional exploitation of vulnerable subjects, especially in the developing world [ 3 , 5 , 6 ].
Public understanding of research may vary according to levels of education and literacy, the existence of a research culture and the extent of debate about science and research in the public domain, while the value placed on individual informed consent practices may have cultural variations [ 2 , 6 , 7 ].
Although the understanding and attitudes of patients from Western countries towards research have been investigated [ 8 - 10 ], the perspectives of individuals from developing countries have received little attention [ 11 - 13 ]. An Egyptian study of individuals' attitudes towards medical research reported that although the participants recognized the value and expressed a great deal of trust in medical research, they nonetheless mentioned concerns about the level of risks associated with several types of medical research [ 11 , 14 ]. This study further concluded that participants experienced difficulty in understanding several research concepts: randomization, double-blind, and clinical equipoise. Trust in the physicians conducting research was important in making the decision to participate in clinical research [ 14 ]. A recent qualitative study conducted in Malawi concludes that people make rational decisions to participate in research, especially in settings with inadequate health services [ 15 ]. This study questions 'therapeutic misconception' in certain low resource settings. A number of studies have been conducted in African countries investigating the attitudes and understanding of research participation, mainly in malaria treatment and vaccine trials [ 16 ].
Several guidelines currently exist for guiding health research in both developed and developing country settings [ 17 , 18 ]. But these guidelines do not address the critical issue of public understanding of research, especially in the developing country context where low literacy, religious beliefs and lack of resources dictate the public perception towards health research. The current study was designed to address the lack of empirical evidence on understanding of medical research and informed consent in Sri Lanka. The study focused on individuals' willingness to participate in research in particular and on information they require in order to make a decision to participate.
Ethical approval
Ethical approval for the project was obtained from ethics review committee (ERC) of the Faculty of Medicine, Sri Jayewardenepura University, Sri Lanka and ERC of the Institute of Psychiatry, King's College London.
This was part of a larger study on informed consent in Sri Lanka [ 19 , 20 ]. The aim of this component of the study was to ascertain the level of understanding of 'research' with a particular emphasis on health research and the concept of voluntary informed consent by exploring the views of the general public and a selected group of professionals in Sri Lanka.
Protocol development process
Along with other components of the project, the initial protocol was subjected to revision based on comments received from reviewers for the funding body. There was also a consultation meeting held in UK to finalise the protocol. The proposal was also presented to an invited audience in Sri Lanka who were either involved in ethics review process or who had a special interest in ethics, some of whom had received training during an intensive course in bioethics funded by the Wellcome Trust in 2003 [ 19 , 20 ].
Following a two-day workshop on qualitative research methods, focus group meetings on the protocol were held to develop consensus. Three rounds of meetings were conducted where strategies for recruiting participants for the study were discussed in depth. Focus group participants felt that it was important to include people who had participated in research as well as people with no research participation experience. Strategies discussed to recruit participants with previous research experience include;
1. Obtain permission from ethics committees to have access to people who participated in previous research.
2. Try to recruit them through researchers who have carried out research projects recently.
3. Door knocking, snowballing technique and convenience sampling
While advantages and disadvantages in all these methods were identified, there were specific ethical concerns arising from using the first and second approaches.
The group discussions led to a final decision to use convenience sampling [ 21 ], recruiting through recommendation from the initial participants and using snowballing technique. Purposeful sampling allowed participants with different professional or educational backgrounds to be recruited ensuring diversity of characteristics.
Sample recruitment
Recruitment was carried out with an emphasis on balanced age and gender representation, diverse educational, socio-cultural and professional backgrounds and on those with previous research experience, either as researchers or participants.
Participants were initially given a verbal description of the study aims and what would be required of them and then invited to participate. An information leaflet and consent form was also provided.
Data collection
The interview schedule consisted of open-ended questions designed to elicit a wide range of views from the participants (appendix). The original questions were composed in English and translated to Sinhalese to facilitate the data collection. At the beginning of each interview, the interviewer informed the participant that this study was focused on healthcare research. Topics included: 'understanding of research, who does research, whether it is good or bad to do research, who benefits, experience in and willingness to participate in research, what sort of information would they want to know before deciding'.
Three research assistants (SH, ML, MA) conducted the interviews. As in other qualitative work carried out by our team in Sri Lanka, the interviews were not audio recorded as this was felt to be culturally too sensitive and could adversely affect the study participation [ 22 ]. Therefore, participants' responses were written verbatim by the interviewers.
A predefined check-list of information important in making a decision to participate in research was included and participants were asked to respond as 'Yes', 'No' or 'Not sure'.
The interviews were conducted with medical students, doctors, teachers, researchers and patients who were selected at Out Patient Departments (OPD) of GP and hospital clinics. Some had previously participated in or conducted research.
Data analysis
The answers to the open ended questionnaire were recorded in written form in Sinhala and subsequently entered in to a SPSS database by two researchers (ML, MA). Then these were manually coded and entered into separate databases for each question (SH, CS). As the interviews were conducted in Sinhalese, the researchers (SH, CS) jointly translated the answers to English before database entry was conducted.
Content analysis of the data was carried out by reading the transcripts line-by-line analysing the contents [ 23 ]. Therefore, interview data under pre determined questions and headings were perused for recurring themes and line by line analysis to identify similar themes. Responses containing similar themes were grouped together and categorised. In order to verify the analysis it was repeated once again by KM and KS. SPSS was also used to analyse the quantitative data presented here.
Participant characteristics
A total of 66 persons (37 males; 56%, 29 female; 44%) participated. The mean age of participants was 41 (range 15-72). The age of nine participants was missing.
The sample included 30 (45%) who had participated in research projects previously and 36 who had not. Participants were patients in the government sector and GP setting, researchers (medical and non-medical), research assistants, medical students and teachers including eight teacher-researchers from National Institute of Education (Table (Table1 1 ).
Study participant representation.
| Participants | Number |
|---|---|
| Previous research participants | 7 |
| Researchers | 8 |
| Research assistants | 4 |
| OPD patients in a hospital | 13 |
| OPD patients in a GP clinic | 5 |
| Teachers | 14 |
| Doctors who have done research | 4 |
| Doctors that have not done research | 4 |
| Medical students | 7 |
The patients from government hospitals and GP setting were considered to be lay-persons. Their educational or professional backgrounds were not recorded explicitly as it was considered non-relevant with concern to the particular study and setting. Therefore, they were simply categorised as lay patients. Researchers (medical and non-medical) were categorised according to their profession, derived from what they indicated as their profession. Research assistants were also taken as a whole, without differentiation into categories such as health or other fields. All the people categorised as students were in fact medical students from various medical faculties in the country.
Initial preliminary analyses of data
As there were two main categories of participants in the study; professionals and non-professionals as well as those who had participated in and conducted research, we compared the responses to following three questions to identify differences in understanding or perceptions between the groups.
1. What do you understand by the word "Research"?
2. Are there words similar in meaning to the word "Research"?
3. To your knowledge, what sort of people conduct research?
As there were no observable differences between the groups on these key questions, we analysed the data for the sample as a whole.
Although this is fundamentally a qualitative study we have presented the frequencies for each theme as combined qualitative and quantitative methods are now becoming more popular and informative [ 24 ]. These themes were derived and defined from participant responses according to similarities in meanings. The responses were coded according to themes which emerged and subsequently quantified in order to identify frequencies. The similarities were identified originally from the Sinhala language responses, and verified for context and concept after translation in to English.
Because the questions were short and structured, the answers were also short and it was possible to accurately record verbatim without limiting the pace of the interview. For each question most patients provided single worded replies while only a few elaborated their answers. Many participants provided several short answers for some questions, giving different meaning words which encompassed the general idea of the answer. In the analysis, these answers were quantified as separate, ignoring the fact that this may lead to the percentages exceeding 100% in numerical sense. Also these separate answers were given due to the complexities in the Sinhala language, in which this questionnaire was administered. Participants used different words to describe and answer a single concept, but these words have distinct contextual differences, leading to the separate coding done in the study.
Research Concept
Out of the total 66 participants, 21 (31.8%) did not provide an answer to this question. The responses from the rest are shown in Table Table2 2 .
Concept of research.
| Searching/look for/inquiries (48.5%) discovery and finding (33.3%) Obtaining data/gathering information/getting to know/gaining knowledge and learning (22.7%) Searching about problems/looking in to problems (13.6%) Testing of blood, urine, stools and other types of laboratory tests ordered by doctors(4.5%) | 'Making a judgment about something' 'Experimenting' 'A process that looks in to see if something is correct or not, in a way that is encouraging to the public' 'Coming to a decision by obtaining data using a certain methodology to make something clear' 'An in-depth search' 'Obtaining a description' 'A study to identify a disease' 'Looking in to something to see if it is good or bad' 'Looking in to something, to comprehend something that is not understood, to improve an existing thing' 'Further exploration of something unknown' 'Using statistical knowledge to collect observations, to summarise, to analyse, to present, to come to conclusions in a scientific background and to forward them to those who require them for future progress' 'Developing a hypothesis and searching if it is correct or not' |
Total number of participants -- 66
Number of participants responded for this question -- 45
A third of participants (22; 33.3%) did not offer an alternative word for research. The responses of the other participants are shown in Table Table3 3 .
Words similar in meaning to the word 'research'.
| Theme (meaning in Sinhala language) | Number |
|---|---|
| Survey/Scientific Survey (SAMEEKSHANAYA) | 15 (23.%) |
| Exploration/Scientific Exploration (GAVESHANAYA) | 8 (12%) |
| Search/Scientific Search/Methodical Search (SEVEEMA/SOYA BELEEMA/SODISI KIREEMA) | 7 (11%) |
| Experiment (ATHHADA BELEEMA) | 6 (9%) |
| Test/Examination (PAREEKSHANAYA/PAREEKSHA KIREEMA/PIRIKSUMA) | 4 (6%) |
| Discovery/Invention (SOYA GENEEMA) | 3 (5%) |
| Observation (NIREEKSHANAYA) | 3 (5%) |
| Research (in English) | 3 (5%) |
| Study (ADYAYANAYA) | 2 (3%) |
| Inquiry (VIMASEEMA/VIMARSHANAYA) | 2 (3.%) |
| Manufacturing (NISHPADNAYA) | 1 (2%) |
| Project (VIYAPRUTHIYA) | 1 (2%) |
| Education (ADYAPANAYA) | 1 (2%) |
| Data collection (DHATHTHA EK RAS KEPEEMA) | 1 (2%) |
| Making a judgement (VINISHCHAYA KIREEMA) | 1 (2%) |
Number of participants responded for this question - 44
People who conduct research
Table Table4 4 shows the types of people who conduct research as indicated by participants.
What sort of people conducts 'research'?
| Doctors, allied medical professionals, health care workers & health institutions | 54(82%) |
|---|---|
| Scientists professionals & learned people | 27 (41%) |
| Businessmen, pharmaceutical & other companies | 10(15%) |
| Anyone | 10(15%) |
| Students & teachers | 8 (12%) |
| Government institutions | 8 (12%) |
| Others | 6 (9%) |
| Nongovernmental organisations (NGO) | 5 (8%) |
The purpose of health research
Twenty five (37.9%) said health research is carried out in order to improve health services to the public, society and to find solutions to health problems in order to make a healthy population. The full set of themes and responses are shown in Table Table5 5 .
Purpose of health research.
| Concept | Themes | Supporting Quotes |
|---|---|---|
| Improve health services to the public, society and to find solutions to health problems (37.9%) Search for/discover/introduce/improve and assess the quality of drugs, treatment and cures (25.8%) Search for, broaden and consolidate knowledge, curiosity and for the advancement of science (19.7%) Achieve individual betterment and to meet educational requirements (7.6%), Commercial gain (6.1%) | 'To keep people informed' 'To identify new diseases, To look in to the knowledge of the public about diseases' 'For the development of the medical profession of Sri Lanka' 'For exams, 'To make new discoveries those are beneficial to the public as drugs and treatments' 'To consolidate knowledge that has been already discovered' 'To get to know about the health status of the population of the country' 'To relieve their suspicions and curiosities, to make a new discovery' 'To scientifically identify health problems, To broaden your knowledge in the field, For individual betterment' 'For individual educational requirements, Institutional requirements, Interest in the problem' |
Benefits and risks of research
Although all participants expressed the view that conducting research was beneficial, the majority (45; 68.2%), believed that untoward effects may arise from research. Table Table6 6 shows the full results.
Benefits and risks of research.
| Concept | Themes | Supporting Quotes |
|---|---|---|
| Benefits Ability to find new knowledge about diseases, new treatment methods for diseases Research helps improve existing knowledge on disease and treatments Research helps to increase productivity of the health sector Risks Adverse effects from participating in research causing harm or death such as drug trials (35.5%) Methodological errors in research resulting in false conclusions (17.8%) | Benefits 'To prove something with scientific evidence as in mosquito eradication' 'To find data on harmfulness of new drugs, to obtain new knowledge' 'To find a cause of a disease' 'To get the correct information regarding something as an illness' 'Search for treatments for diseases as cancer and rabies, Vaccines for prevention Increase productivity of the health sector' 'To assess the weakness of an old treatment' 'To solve problems and provide the right answer' Risks 'Adverse effects from participating in research causing harm or death as in drug trials' 'The harm to placebo group of patients in a drug trial' 'Being cheated due to the ignorance of the public' 'In research done by private institutions, due to signing of agreements there could be problems in withdrawing' 'Research that is not ethical', 'Presenting false research reports' 'Blood samples being used for other things', 'participants are not properly cared for' 'Plundering of genetic resources, selling our resources' 'Abusing people in the third world by developed nations' 'Research on arms development, research that are done with the aim of financial gain and those done in areas that has no benefit for society' |
Who benefits from research?
Most participants (51; 77%) nominated very broad categories of public beneficiaries ( everyone, we, society, public, country, world, humanity ). According to 21 (32%) respondents, researchers, research institutions and scientists stood to benefit from research. Other nominations included patients (12; 18%), businessmen, drug manufacturers and companies (9; 14%), health professionals (9; 13%) and policy makers (2; 3%).
How are research participants selected?
Two themes emerged from half (33) of the study participants' views on this topic:
1. Depending on the requirements of the research question, suitable/relevant individuals/patients with certain characteristics/features/conditions/diseases, are selected according to inclusion criteria
2. According to the sampling method of the research, a random sample or if possible all relevant individuals/patients will be selected
A further 6(9%) participants held the view that participants were selected from individuals giving consent or volunteering by themselves or by choice of participant .
Among the 30 (45%) participants who had previously taken part in research, the following descriptions were given of the type of study in which they had been involved: undergoing investigations, market surveys, health and community surveys .
Some of the responses are reported below verbatim for clarity
'Those with grater skill in research, specialists, researchers'
'According to the connections of the researcher'
'Those with greater knowledge'
'Those with the dedication'
'Ask for those willing to participate after calling people to gathering in committees'
'According to patient's choice'
'Individual thought to be suitable by the researchers, that is willing to make a sacrifice, able to conduct one self in society'
'Level of education, social status, job, according to the problems, ability to answer questions'
Willingness to take part in research
The overwhelming majority (59; 89%) expressed their willingness to participate in future research while five (8%) said they would not and two (3%) were undecided.
While 17 (26%) participants said they would not consult anyone before deciding whether to take part in research, the majority (48; 73%) indicated that they would discuss with someone before giving consent to take part in research. Thirty six (75%) of this group said they would consult their family and friends , 16 (33%) would consult a knowledgeable person on the matter, and 14 (29%) would consult a researcher or research assistant . One (2%) participant thought consulting superiors would prove to be the most appropriate.
Types of research willing or unwilling to join
Table Table7 7 shows types of research that the participants were willing or unwilling to join.
Types of research willing or unwilling to join.
| Concept | Themes | Supporting Quotes |
|---|---|---|
| Research that involves donating tissue samples from body including blood (35.8%) Health research (15%), questionnaire research (11%) Research that benefits society 11%) Do not wish to segregate research or not particular about the type of research (18.9%) | 'Those that answer the problems faced in life' 'Research that is of benefit to the country and public Education research' 'Research on rehabilitation of disabled children' | |
| Involving testing of a new drug or a treatment (36%) Invasive/interventional research with instrumentation/research where there is introduction of something in to the body or taken internally (26%) Done only for the benefit of the researcher/of no benefit to society or detrimental to the country (13%) | 'If have to go to some other place' 'Participating in medical tests' 'Things that go by the name research but that are not research' 'Research about extremely personal issues' 'Research of an unfamiliar field' | |
Information needed for decision making
Two strategies were adopted to examine this aspect. Initially participants' views were sought through open ended questions and their responses were noted verbatim. Secondly, participants were given a pre-defined checklist of information pertaining to the decision to take part in research and asked to note whether each of these was important to them in making the decision to participate in research.
Table Table8 8 lists participants' responses to the open ended question. Table Table9 9 shows their responses to the pre-defined checklist.
Participants' responses to the open ended questions on important information they wish to have to decide to participate in research.
| Objectives of the Research/Reason/Importance/Relevance | 27 (43%) |
|---|---|
| What is the research/Type/Nature/Field | 23 (37%) |
| Potential benefits/risks to society | 19 (30%) |
| Potential benefits/risks to participant | 19 (30%) |
| Credibility & legitimacy of Researchers/Institutions | 14 (22%) |
| What is expected of participant/participation related info/Why selected | 11 (18%) |
| Expected outcome/Protocol rationale/how scientific | 10 (16%) |
| How results would be/should be used | 9 (14%) |
| Methodology | 8 (12%) |
| Confidentiality | 3 (5%) |
| Can withdraw anytime | 2 (3%) |
| Ethical issues/intentions good or bad/information source | 2 (3%) |
Participants' responses to the pre-designed checklist on important information they wish to have to decide to participate in research.
| Yes (%) | No (%) | Not sure (%) | |
|---|---|---|---|
| 1. Description of the project | |||
| 1) verbally | 62(94%) | 3(5%) | 1(2%) |
| 2) in writing | 59(89%) | 6(9%) | 1(2%) |
| 2. Who are the researchers? | 56(85%) | 8(12%) | 2(3%) |
| 3. Who is funding? | 37(56%) | 28(42%) | 1(2%) |
| 4. Why have you been selected? | 52(79%) | 13(20%) | 1(2%) |
| 5. It is compulsory to take part? | 54(81.8%) | 9(14%) | 3(5%) |
| 6. A statement assuring that declining to take part will not affect medical care | 49(74%) | 15(23%) | 2(3%) |
| 7. A statement stating that even if they agree to take part it is possible to leave the research at any time | 56(85%) | 9(14%) | 1(2%) |
| 8. What will they have to do as research participants? | 64(97%) | 1(2%) | 1(2%) |
| 9. Informing that they are free not to answer any question or not do thing if they as so wish? | 56(85%) | 8(12%) | 2(3%) |
| 10. Are there any risks involved? If so what are they? | 60(91%) | 5(8%) | 1(2%) |
| 11. Will the information given be confidential? | 58(88%) | 7(11%) | 1(2%) |
| 12. Contact details of main researchers? | 55(83%) | 10(15%) | 1(2%) |
| 13. What are the possible benefits 1)To me?(missing data-1) | 6(85%) | 8(12%) | 1(2%) |
| 2) Wider benefits if any? | 65(99%) | 0(0%) | 1(2%) |
Table Table8 8 shows that, unprompted, participants nominated important points of information on research, which appeared as pre-defined items in Table Table9. 9 . Most participants agreed readily when prompted that the information was important.
An overwhelming 56 (85%) noted that they require a time gap between receiving the information leaflet to taking a decision and notifying the researcher of their decision. Only 9 (13.6%) respondents said that they would not require a time gap.
The majority (61; 92%) were aware that they were participating in a research project right now.
The results show that with or without prior participation in research, participants in this study had a reasonable understanding of research, including the following core information: what is research, why research is conducted, why members of the public are selected, whether the outcome of participation is beneficial or may bring harm and whether the decision to participate is affected by knowledge about research and researchers. The 'reasonable' understanding mentioned above was deemed so after considering the fact that most participants indicated an understanding about the core issues concerning participation in research.
As indicated from some studies conducted in Africa, public will participate in research according to the circumstances regardless of literacy in the absence of other care provision alternatives [ 15 ]. Also, our study results indicate that almost 30% of participants were illiterate about the meaning of research. It is in this context that the public knowledge and awareness about core reasons for participation in research presented in this study is important.
In spite of the general understanding of the participants on core ideas about research, a small number of participants believed that research meant laboratory tests ordered by doctors and that the words test and research were similar in meaning. As shown in findings of this study, participants seem to be reluctant to take part in drug research or intervention studies. This is an important finding in view of more and more new drug related clinical trials taking place in developing country settings. But, in answer to a different question in the study, majority of participants expressed willingness to take part in future research, which may mean that although drug trials and interventions are perceived to be harmful in some sense, people are keen to take part in other areas of research perceived to be less harmful. The reasons for people perceiving drug research and interventions to be harmful are areas that merit further exploration.
The findings show that a decision about taking part in research is not only dependent on the knowledge and education of the participant but also on the views of their immediate social network of family and friends. This reflects on the strong family structure inherent in Sri Lankan society which is also common to other countries and cultures in the South Asian region [ 25 ]. Within this backdrop, it raises an important point for researchers to address when designing studies and obtaining informed consent in the future.
Majority of health and other research is being conducted by various government agencies which include universities, research institutions and others in Sri Lanka. But, in this study it appears that participants had only a vague idea about government being an agency conducting research. Although the majority had indicated health professionals and scientists to be the sort of people conducting research, they had not observed a link between these professionals and the government, which employs the majority of researchers. This raises questions about public opinion and lack of awareness about government involvement in research in the Sri Lankan context.
This paper stands to add a perspective from a developing Asian country to the existing literature and debate about the issue of public understanding of research. As Sri Lanka has higher health indicators and a better developed health system and infrastructure than most developing countries in Africa and Asia coupled with a high literacy rate [ 26 ], it is important to bring out what its people think about health research. The attitudes and beliefs expressed by them may help to shape future and ongoing research in other developing countries.
The results demonstrate that the majority were supportive of health research and all participants confirmed that research is beneficial to the welfare of the society. Contrary to academic assumption that the public is averse to taking part in research [ 4 ], our sample expressed willingness to take part, even in research that requires taking body tissue samples. This is an encouraging sign. Given this good will, it is essential that undue exploitation of public trust and support for research should be prevented by adhering to sound ethical principles.
Limitations
Participants were drawn from diverse educational, socio-cultural and professional backgrounds, with and without previous research experience. Therefore, differences between subgroups could not be specifically investigated. However, the aim was to capture a wide range of views and understanding on research and consent. Although the findings cannot be generalised to the whole population, the majority of participants appear to be educated and knowledgeable about basic health research and held positive attitudes. They will continue to be supportive of sound ethical research agendas. This work has also opened up the scope for more research in these areas expanding some of the positive as well negative perceptions revealed in the study.
Competing interests
The authors declare that they have no competing interests.
Authors' contributions
AS proposed the initial conceptual framework for the research and was responsible for overall conduct of the project. AS, SS, SH, MP and JM were involved in the protocol design, writing and editing the manuscript. SS, SH, ML, MA, CS, KM, KS contributed to the modification of the protocol, collection and analysis of data including the statistical analysis. KM and KS were involved in the reanalysis of data. AS prepared, the first draft and AS, CS, SS wrote the second draft. All authors were involved in subsequent editing and agreed on the final version. CS and AS further edited the paper as required by reviewers.
The interview schedule for general public who have not participated in research previously
In this study we are mainly interested in healthcare research. So can you tell me
1. What does the word "research" mean to you?
2. Is there any other word for research?
3. In your opinion what sort of people will do research?
4. Why do you think they do healthcare research? What is the purpose?
5. Is it a good thing to do research? Can you give an example?
6. Are there any bad things about research? Can you give an example
7. Who do you think benefits from research?
8. How do people get selected or invited for research?
9. Have you ever participated in research? If yes, can you tell me about it?
10. If you are asked to participate in a research in the future will you participate?
11. Would you like to discuss it with someone else before you agree?If yes, who are they//who would that be?
12. What are the types of research that you would
• Like to participate in
• Not Like to participate in
13. What information would you like to have about the research that would help you to decide to or not to participate in research?
14. Which of the following information would you think is/are important for the decision?
CHECKLIST-A →
• Description of the project reflecting what it is about
• Who are the researchers?
• Who provided the funds?
• Why have you been selected?
• Is it compulsory to take part (is it entirely voluntary)?
• A statement assuring that in the case of declining to take part, it will have no affect on the medical care that they receive or any other affect on them
• A statement stating that even if they agree to take part it is possible to leave the research at any point
• What will they have to do as research participants?
• Informing that they are free not to answer any questions or not to do things if they as so wish
• Are there any risks involved? If so what are they?
• Will the information given be confidential?
• Contact details of main researchers
• What are the possible benefits?
& wider benefits if any
• Any other
15. Do you need to have a gap between giving the information leaflet and in deciding whether to participate?
16. Do you realize that you are engaged at the moment is also a research?
Pre-publication history
The pre-publication history for this paper can be accessed here:
http://www.biomedcentral.com/1472-6939/11/7/prepub
Acknowledgements
We would like to thank the BMC Medical Ethics reviewers; Michael Parker and Christine Grady for their valuable contribution in improving this manuscript. We would also like to thank Ms Suranga Sewwandi for her assistance with the manuscript preparation. This work was funded by a Wellcome Trust Biomedical ethics grant (074928).
- Doyal L, Tobias JS, Warnock M, Power L. Education and debate. BMJ. 1998; 316 :1000–1005. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Butta ZA. Ethics in international health research: a perspective from the developing world. Bull World Health Organ. 2002; 80 :114–120. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Benatar SR. Reflections and recommendations on research ethics in developing countries. Social Science & Medicine. 2002; 54 :1131–1141. [ PubMed ] [ Google Scholar ]
- Edwards SJL, Lilford RJ, Hewison J. The ethics of randomised controlled trials from the perspectives of patients, the public and healthcare professionals. BMJ. 1998; 317 :1209–1212. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Shapiro HT, Meslin EM. Ethical issues in the design and conduct of clinical trials in developing countries. N Engl J Med. 2001; 345 :139–142. doi: 10.1056/NEJM200107123450212. [ PubMed ] [ CrossRef ] [ Google Scholar ]
- Costello A, Zumla A. Moving to research partnership in developing countries. BMJ. 2000; 321 :827–9. doi: 10.1136/bmj.321.7264.827. [ PMC free article ] [ PubMed ] [ CrossRef ] [ Google Scholar ]
- Bhutta ZA. Beyond informed consent. Bull World Health Organ. 2004; 82 :771–777. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Madsen SM, Mirza MR, Holm S, Hilsted KL, Kampmann K, Riis P. Attitudes towards clinical research amongst participants and nonparticipants. Journal of Internal Medicine. 2002; 251 :156–168. doi: 10.1046/j.1365-2796.2002.00949.x. [ PubMed ] [ CrossRef ] [ Google Scholar ]
- Akkad A, Jackson C, Kenyon S, Dixon-Woods M, Taub N, Habiba M. Research: Patients' perceptions of written consent: questionnaire study. BMJ. 2006; 333 :528. doi: 10.1136/bmj.38922.516204.55. [ PMC free article ] [ PubMed ] [ CrossRef ] [ Google Scholar ]
- Miller JD. Public understanding of, and attitudes toward, scientific research: what we know and what we need to know. Public Understand Sci. 2004; 13 :273–294. doi: 10.1177/0963662504044908. [ CrossRef ] [ Google Scholar ]
- Khalil SS, Silverman HJ, Raafat M, El-Kamary S, El-Setouhy M. Attitudes, understanding, and concerns regarding medical research amongst Egyptians: A qualitative pilot study. BMC Medical Ethics. 2007; 8 :9. doi: 10.1186/1472-6939-8-9. [ PMC free article ] [ PubMed ] [ CrossRef ] [ Google Scholar ]
- Verastegui EL. Consenting of the vulnerable: the informed consent procedure in advanced cancer patients in Mexico. BMC Medical Ethics. 2006; 7 :13. doi: 10.1186/1472-6939-7-13. [ PMC free article ] [ PubMed ] [ CrossRef ] [ Google Scholar ]
- Caniza MA, Clara W, Maron G, Navarro-Marin JE, Rivera R, Howard SC, Camp J, Barfield RC. Establishment of ethical oversight of human research in El Salvador: lessons learned. Lancet Oncology. 2006; 7 :1027–1033. doi: 10.1016/S1470-2045(06)70977-9. [ PubMed ] [ CrossRef ] [ Google Scholar ]
- Sackett DL. Participants in research. BMJ. 2005; 330 :1164. doi: 10.1136/bmj.330.7501.1164. [ PMC free article ] [ PubMed ] [ CrossRef ] [ Google Scholar ]
- Mfutso-Bengo J, Ndebele P, Jumbe V, Mkunthi M, Masiye F, Molyneux S, Molyneux M. Why do individuals agree to enrol in clinical trials? A qualitative study of health research participation in Blantyre, Malawi. Malawi Medical Journal. 2008; 20 (2):37. [ PMC free article ] [ PubMed ] [ Google Scholar ]
- Barry M, Molyneux M. Ethical dilemmas in malaria drug and vaccine trials: a bioethical perspective. J Med Ethics. 1992; 18 :189–1920. doi: 10.1136/jme.18.4.189. [ PMC free article ] [ PubMed ] [ CrossRef ] [ Google Scholar ]
- Declaration of Helsinki. Bulletin of the WHO. 2001. pp. 373–374. [ PMC free article ] [ PubMed ]
- Council for International organizations of Medical Sciences (CIOMS 2002) International guidelines for ethical review of epidemiological studies. Geneva
- Sumathipala A, Siribaddana S, Hewege S, Lekamwattage M, Athukorale M, Siriwardhana C, Murray J, Prince M. Informed consent in Sri Lanka: a survey among ethics committee members. BMC Medical Ethics. 2008; 9 :10. doi: 10.1186/1472-6939-9-10. [ PMC free article ] [ PubMed ] [ CrossRef ] [ Google Scholar ]
- Sumathipala A, Siribaddana S, Hewege S, Lekamwattage M, Athukorale M, Siriwardhana C, Murray J, Prince M. Ethics Review Committee approval and informed consent: an analysis of biomedical publications originating from Sri Lanka. BMC Medical Ethics. 2008; 9 :3. doi: 10.1186/1472-6939-9-3. [ PMC free article ] [ PubMed ] [ CrossRef ] [ Google Scholar ]
- Bryman A. Social Research Methods. Second. Oxford University Press. New York; 2004. [ Google Scholar ]
- Sumathipala A, Siribaddana S, Prince M, Mann AH. Understanding the cognitive representation of medically unexplained symptoms and its implication on treatment development research: A Sri Lanka study. BMC Psychiatry. 2008; 8 :54. doi: 10.1186/1471-244X-8-54. [ PMC free article ] [ PubMed ] [ CrossRef ] [ Google Scholar ]
- Strauss A. Qualitative Analysis for the Social Scientists. Cambridge: Cambridge University Press; 1987. [ Google Scholar ]
- Onwuegbuzie AJ, Leech NL. The Importance of Combining Quantitative and Qualitative Research Methodologies. International Journal of Social Research Methodology. 2005; 8 :375–387. doi: 10.1080/13645570500402447. [ CrossRef ] [ Google Scholar ]
- Freeman MA. Demographic Correlates of Individualism and Collectivism: A Study of Social Values in Sri Lanka. Journal of Cross-Cultural Psychology. 1997; 28 :321. doi: 10.1177/0022022197283007. [ CrossRef ] [ Google Scholar ]
- World Health Organization. The world health report 2007: a safer future: global public health security in the 21st century. Geneva. 2007.
Publications
- Research Reports
- Research Briefs
- Policy briefs
- Debt Update
- Background Note

The 13% primary expenditure rule proposed in a new public finance bill is at odds with established economic theory. It will undermine “good” public spending that enhances growth, efficiency, and social welfare. It will also make Sri Lanka a global outlier, by setting a GDP based limit on primary expenditure, which is the lowest in the world.

This note proposes three steps Sri Lanka could take to construct and manage high quality Investment Zones, drawing from regional and global best practices. First, is enacting a separate, overarching legislation to govern Zones. Second, is enhancing the quality of Zones by mandating minimum quality standards and establishing minimum criteria for selecting investors to develop and manage Zones. Third, is preventing conflicts of interest by separating the roles and responsibilities of regulators, developers, and operators and establishing a level playing field by ensuring regulatory independence. Underlying these proposals is the recognition that Sri Lanka needs to have a more robust regulatory framework than what is provided in the Economic Transformation Bill (ETB) gazetted on May 14, 2024. The need for such a framework is higher in Sri Lanka, given the scarcity of land and intense competition in the Asian region for foreign investments. The recommendations address three critical problems that have made Sri Lanka fall behind many of its regional peers. s. First, Sri Lanka has under-invested in both the quantity and quality of Zones. Second, it has exclusively depended on the public sector to build and manage Zones. Third, the country lacks an appropriate regulatory framework to attract private…

This report delves into the intricate landscape of Freedom of Religion or Belief (FoRB) in Sri Lanka, particularly focusing on the challenges surrounding the establishment and maintenance of places of worship. It sheds light on discriminatory practices, including registration requirements imposed by Ministry of Buddha Sasana circulars, which have disproportionately affected minority religious groups. By examining both international standards and domestic legal frameworks, the report aims to provide insights and recommendations to safeguard the right to FoRB in Sri Lanka and ensure equitable treatment for all religious communities.

This working paper outlines the technical and incentive dynamics for a proposed new sovereign debt instrument designed for countries with high country risk premiums, where this risk is, ceteris paribus, correlated with the quality of present and future governance. We call this instrument a Governance-Linked Sovereign Bond (GLSB). The paper introduces the design of a GLSB and the formulaic method for deploying such an instrument in situations where country risk premiums might be correlated with governance-related actions. A specific illustrative model is used to demonstrate the practical applications of this debt instrument.

Ethno-religious violence against minority groups in Sri Lanka is a long-entrenched phenomenon that has persisted, irrespective of changes in the political landscape of the country. This study examines critical trends in religiously motivated violence against Christians between November 2022 and October 2023, based on data collated by the National Christian Evangelical Alliance of Sri Lanka (NCEASL). The study unpacks three empirical insights into factors that lead to violence against Christians. These insights are data-driven explanations of who the primary perpetrators are, their main targets, and the modality through which they incite violence against Christians. The study also provides insight into harmful speech content against prominent religions in Sri Lanka found on online platforms. View Past Reports: Religious violence against Christians: Disruptions and Distractions Patterns and risks of Religious violence against Christians (October 2020 – October 2021) Prejudice and Patronage: An Analysis of Incidents of Violence against Christians, Muslims, Hindus in Sri Lanka (2021) Inaction and Impunity: Incidents of Religious Violence Targeting Christians, Muslims and Hindus (2015 – 2019)

A ‘Blueprint for a Rational Government in Sri Lanka‘, created by Verité Research and Manthri.lk, seeks to implement the recommendations from the White Paper on “A Rational Method for Cabinet Formation in Sri Lanka“, published in 2020. It lists down the duties and functions, institutions and acts to be implemented under the 15 ministries proposed in the annexures of the White Paper, following revisions that were supported by extensive expert consultation. This document is the blueprint by which governments can solve 3 key issues relating to irrational cabinet formation: 1. Misalignment of subjects Unrelated subjects being grouped together under one ministry. 2. Fragmentation of subjects Related subjects being split across different ministries. 3. Not having a fixed structure for ministries and their institutions Ministry purviews often change alongside ministerial appointments and shuffles, resulting in institutions shifting from ministry to ministry. The document takes on the form of an extraordinary gazette, and serves as a starting point for a more effectively and efficiently structured form of government.

The State of the Budget 2024 report compiled by Verité Research assesses the financial, economic and fiscal assumptions, the computation of estimates, and reporting standards applied in the 2024 Budget Speech. The state of the Budget is set out in four main sections. Section one introduces the report, sets out its objectives, and provides some background on Sri Lanka’s budget formulation process. Section two draws attention to the various deficiencies in the budget. Section three analyses the revenue estimates used in Sri Lanka’s 2024 Budget. Section four focuses on expenditure allocations and highlights concerns regarding the 2024 budget.

To address the governance risk to debt sustainability and provide incentives for the Government of Sri Lanka to implement governance reforms, this proposal sets out the structure of a novel sovereign debt instrument that can be used for countries with significant country risk in terms of future default, where the risk is likely to be correlated with the trajectory of governance. It is termed a “Governance-Linked Sovereign Bond” (GLSB). This short proposal is derived from a working paper by Verité Research that sets out the technical basis for the GLSB described here.

The research brief titled “Backwards in Blacklisting: Gaps in Sri Lanka’s Procurement Framework Enable Corruption” by Verité Research, published in November 2023, critically evaluates Sri Lanka’s public procurement system. It highlights two significant gaps: the legal gap, where procurement guidelines don’t allow for blacklisting contractors/suppliers involved in fraud and corruption, and the compliance gap, shown by the failure to maintain a blacklist for defaulting contractors. The brief compares Sri Lanka’s approach unfavourably with other South Asian countries, noting these countries’ more effective implementation of blacklisting and their maintenance of updated online databases of blacklisted firms. The study emphasizes the need for Sri Lanka to implement robust blacklisting provisions and maintain a comprehensive online list of blacklisted companies to deter corruption and ensure efficient use of public funds.

Sri Lanka has specific personal laws applicable to distinct ethnic and religious groups, such as Kandyan law, Muslim law and Tesawlamai law. Critics, both domestically and internationally, have raised concerns about discriminatory provisions in Sri Lanka’s personal laws that contradict constitutional and human rights standards. This working paper aims to assess the disparities between Sri Lanka’s personal laws and international standards, particularly focusing on gender discrimination and impacts on women and children’s rights. Recommendations for reforms aligning with international standards will be proposed, advocating for the evolution of personal laws while retaining Sri Lanka’s pluri-legal aspects.

British Council unveils research on transnational education in Sri Lanka
The report makes recommendations to bridge the gap in higher education quality and drive economic growth.
The British Council released a pivotal report that offers valuable insights into the current state and future potential of transnational education (TNE) in Sri Lanka, underscoring the opportunities and challenges faced by students and educational institutions.
The report was launched at the BMICH and was attended by the British High Commissioner to Sri Lanka Andrew Patrick, education ministry officials, education policy makers, officials from the University Grants Commission, state and non-state university officials.
The Minister of Education, Susil Premjayantha said: “Despite Sri Lanka’s high literacy rate and impressive strides in basic education, higher education capacity remains a significant challenge, with only 44,000 of the 171,532 qualified students gaining admission to state universities in 2022. This shortfall has driven a growing demand for private higher education and transnational education which has proliferated in the last few years.
“We hope that this report will shed light on how TNE can bridge the gap in Sri Lanka’s higher education landscape.”
The Country Director of British Council Sri Lanka, Orlando Edwards said: “The report is testament to our ongoing commitment in South Asia where we collaborate with governments and stakeholders to enhance access and quality of international education, while fostering cross-border partnerships and collaboration. Sri Lanka is rapidly becoming a hub for transnational education. In 2022-2023, it emerged as the second-largest country for UK TNE, accounting for 10% of all UK TNE enrolments globally with a 50% surge in UK TNE—totalling almost 54,000. This research report highlights the immense potential of TNE in bridging the gap in higher education access and driving economic growth for the country.”
Cable Solutions debuts trading on CSE
Union bank appoints dilshan rodrigo as chief executive officer, you may like.
Your email address will not be published. Required fields are marked *
Save my name, email, and website in this browser for the next time I comment.
SEC amends entry requirements for Capital Market professionals
In a move aimed at enhancing professional standards and increasing accessibility in the capital market industry, the Securities and Exchange Commission (SEC) has issued a Directive that provides new entry requirements and exemptions for its certification programs.
This Directive which came into effect from 1st August 2024 contains new entry requirements designed to better serve aspiring and current investment advisors by aligning educational and professional requirements with industry best practices and emerging market trends.
The SEC develops and administers professional education and Continuous Professional Development (CPD) programs as a part of Sri Lanka’s capital market licensing framework. The licensing processes is crucial to uphold high standards of professionalism and trust in the financial advisory sector, thereby protecting investors’ interests and enhancing the stability of financial markets.
The SEC administers the Certificate in Capital Markets (CCM) program, which is the only pathway to obtaining the Registered Investment Advisor (RIA) Qualification and is designed to provide comprehensive education and training for professionals in Sri Lanka’s capital market. Relaxation of the entry requirements for CCM is expected to make it easier for a wider range of candidates to participate in this crucial program. Previously, candidates seeking to register for the CCM were required to hold either 3 passes for Advanced Level (A/L), a completed degree or a completed professional qualification in any discipline. The new entry criteria now recognize a broader range of academic and professional qualifications allowing more individuals to pursue the certification program.
Additionally, to accommodate various professional backgrounds and prior learning experiences, the SEC has broadened the exemption policy for CCM. Previously, the SEC only granted exemptions for candidates who had passed Level 2 of Chartered Financial Analyst. However presently, candidates who are passed finalists of Chartered Institute of Management Accountants (CIMA), Association of Chartered Certified Accountants (ACCA), Institute of Chartered Accountants of Sri Lanka (CA) and candidates who have completed a Bachelor’s or a Master’s Degree in a finance related discipline can apply for exemptions as well.
Moreover, the eased minimum entry requirements and updated exemption policy apply to single asset class certification programs as well.
The first batch of the CCM program, featuring the revised entry requirements and exemptions, is set to begin on August 31, 2024. Comprehensive details are available on the SEC website www.sec.gov.lk. This launch represents a significant step forward in offering accessible, high-quality certification opportunities for capital markets professionals.
These revisions are designed to elevate the standards of the industry while making it more inclusive and supportive of ongoing professional growth.
The shares of Cable Solutions Limited (CODE: CSLK-N-0000) commenced trading on the Colombo Stock Exchange (CSE) on 14th August 2024. The shares have been listed on the Diri Savi Board of the CSE. The occasion was marked with a special Bell Ringing Ceremony.
The company’s Initial Public Offering (IPO) for over 80 million ordinary voting shares for sale at Rs. 7.50 per share, was notably oversubscribed on the opening day itself.
The event was attended by Suren Madanayake, Chairman, Cable Solutions Limited (CSL); Pawan Tejwani, Managing Director, CSL, Mahesh Amarasiri, Director, CSL; Daya Wahalatantri, Director, CSL; Ms. Ranila Wijesundara, Head of Operations, Tempest PE Partners; Ms. Sajana Gunewardhana, Assistant Manager, Tempest PE Partners; Dumith Fernando, Chairman, Asia Securities; Udesh Rajeendra, Vice President Investment Banking, Asia Securities Limited (ASL) ; Ms. Pavani Hindurangalage, Analyst, ASL; including guests from CSL, ASL and Tempest PE Partners. The CSE was represented at the event by its CEO, Rajeeva Bandaranaike; CRO, Renuke Wijayawardhane and the CSE Senior Management.
Delivering the opening remarks, Rajeeva Bandaranaike congratulated Cable Solutions Limited on its progressive initiative to go public. “With an oversubscribed IPO on its opening day, Cable Solutions now becomes a PLC today. This milestone will elevate your corporate status and enhance relationships with your customers, suppliers, bankers, and investors. Listing brings greater visibility and brand recognition for the company and over time creates wealth for your shareholders. The compliance and regulatory framework you now enter will further strengthen your company’s standing, leading to significant long-term benefits.”
Pawan Tejwani, delivering the keynote address, stated, “Cable Solutions is truly a synergistic product of collective vision. Our success hinges on preserving our core values while stimulating progress. This blend has created a dynamic organization that has achieved significant growth, including a successful IPO.” He concluded, “I believe export growth is inseparably connected with investor confidence, and with strong investor support, I am optimistic about our continued growth.”
Union Bank announced the appointment of Dilshan Rodrigo as its new Director/Chief Executive Officer, effective 16 August 2024. With an impressive career spanning over two decades in the banking sector, Rodrigo’s appointment signifies a transformative moment for the bank. Under his leadership, Union Bank aims to navigate the evolving landscape of Sri Lanka’s banking industry and become a beacon of innovation and customer-centric strategies in an era of digitalization.
Rodrigo stated that “Union Bank is committed to being at the forefront of banking innovation and service excellence. Our focus will be on harnessing our capital strength to drive growth and expand our footprint, particularly in the retail and SME sectors. We will capitalize on our well-located branches across Sri Lanka to target key areas for development and transform our digital capabilities to better serve our customers. Union Bank will also foster sustainable entrepreneurship through the Union Bank School of Social Entrepreneurship (UBSSE). The Bank’s strategic priorities will be aligned to the vision of CG Corp Global group, Union Bank’s main shareholder, led by Nepalese billionaire Dr. Binod Chaudhary. He further added that the recent stabilization of Sri Lanka’s economy offers a favourable environment for Union Bank to achieve its growth targets and emphasized the importance of leveraging past experiences to strengthen the production economy, drive value-added exports, and attract foreign direct investment “
Welcoming Rodrigo as the new Director/Chief Executive Officer of Union Bank, Chairman Nirvana Chaudhary expressed his confidence in the appointment, stating, “Dilshan’s extensive experience and dedication to digital transformation perfectly align with our vision to elevate Union Bank into Sri Lanka’s top five banks within the next 3-5 years. His leadership will be pivotal in driving shareholder value and accomplishing our strategic goals.”
EC Chief warns candidates: Violation of election laws could cost them even their civic rights
Ranil gets ‘gas cylinder’, a male-dominated contest, ‘dates have the highest sugar content to fight coronavirus’, sunday island 27 december – headlines, #sundayisland sunday island- 31 january- headlines, sunday island – 28th march, sunday island headlines – 21 march, sunday island – 21st february – headlines.
ADB steps up to support accountant entrepreneur in her own venture
Kaspersky cybersecurity summit in SL reveals emerging threats and AI-powered challenges
The Geopolitics of Democracy
Ekagei kaema (polyandry) – a way of life in the Kandyan highlands
HNB Assurance Finalist at Mob-Ex and The Drum Awards
TRC gives licence to Elon Musk’s Starlink to offer Satellite Broadband Services across the country
Harin, Manusha say happy to leave after helping make Lanka stable
Disney unveils Avatar 3’s official title and new films
Log in using your username and password
- Search More Search for this keyword Advanced search
- Latest content
- Supplements
- BMJ Journals
You are here
- Volume 8, Issue Suppl 6
- Sri Lanka’s COVID-19 response and maintaining health services: implications for future pandemics
- Article Text
- Article info
- Citation Tools
- Rapid Responses
- Article metrics
- http://orcid.org/0000-0002-5013-2816 Ravindra Prasan Rannan-Eliya ,
- Azrah Ghaffoor ,
- http://orcid.org/0000-0003-2572-8666 Sarasi Amarasinghe ,
- http://orcid.org/0000-0003-3344-740X Manage Dhanusha Nirmani ,
- http://orcid.org/0000-0002-2241-3194 Nilmini Wijemunige ,
- Sanjay Perera ,
- http://orcid.org/0000-0002-8137-3786 Sarath Samarage ,
- KCS Dalpatadu ,
- Niroshani Wisidagama ,
- http://orcid.org/0000-0002-4618-4947 Sachini Fonseka ,
- Nalin Kumara ,
- Ahthiga Selvaratnam ,
- Thimani Dananjana
- Institute for Health Policy , Colombo , Sri Lanka
- Correspondence to Dr Ravindra Prasan Rannan-Eliya; ravi{at}ihp.lk
This study examines how Sri Lanka, a lower-middle income country, managed its COVID-19 response and maintained health services. It draws on an extensive document review, key informant interviews and a national survey of public experience and opinion to assess what Sri Lanka did, its effectiveness and why.
Owing to a strong health system and luck, Sri Lanka stopped the first wave of COVID-19 infections, and it adopted a ‘Zero-COVID’ approach with the explicit goal of stopping outbreaks. This was initially effective. Outbreaks reduced healthcare use, but with minimal impact on health outcomes. But from end-2020, Sri Lanka switched its approach to tolerating transmission and mitigation. It took proactive actions to maintain healthcare access, and it pursued a COVID-19 vaccination effort that was successful in covering its adult population rapidly and with minimal disparities. Despite this, widespread transmission during 2021–2022 disrupted health services through the pressure on health facilities of patients with COVID-19 and infection of healthcare workers, and because COVID-19 anxiety discouraged patients from seeking healthcare. This led to substantial mortality and more than 30 000 excess deaths by 2022.
We find that Sri Lanka abandoned its initially successful approach, because it failed to understand that its chosen strategy required symptomatic PCR testing in primary care. Failure to invest in testing was compounded by groupthink and a medical culture averse to testing.
Sri Lanka’s experience confirms that strong public health capacities, robust healthcare systems and intersectoral action are critical for pandemic response. It shows that civilian–military collaboration can be beneficial but contested, and that lack of fiscal space will undermine any response. It also demonstrates that pandemic preparedness cannot guarantee a successful pandemic response. Policy and research must pay more attention to improving decision-making processes when faced with pandemics involving novel pathogens, rapid spread, and substantial scientific uncertainty.
- health policy
- health services research
- health systems
- public health
Data availability statement
Data may be obtained from a third party and are not publicly available. The key informant interview transcripts and recordings cannot be shared as informants were provided an absolute guarantee of confidentiality. Data from the IHP Private Hospitals Census Survey used in this study were collected with a guarantee of confidentiality, and so are not publicly available. The Sri Lanka Health and Ageing Study (SLHAS) Wave 1 and 2 data used in this study are not publicly available. They were provided by the SLHAS Consortium which has adopted an Open Data policy which will provide access to SLHAS Wave 1 data from 2024 and Wave 2 data on a later date, on application to the Consortium by interested researchers. Until the relevant access protocols are published, interested researchers may contact the corresponding author for further information. All other data used in this study are in public domain or can be requested directly from the relevant agencies.
This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, appropriate credit is given, any changes made indicated, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/ .
https://doi.org/10.1136/bmjgh-2023-013286
Statistics from Altmetric.com
Request permissions.
If you wish to reuse any or all of this article please use the link below which will take you to the Copyright Clearance Center’s RightsLink service. You will be able to get a quick price and instant permission to reuse the content in many different ways.
WHAT IS ALREADY KNOWN ON THE TOPIC
The COVID-19 pandemic severely disrupted healthcare systems and health outcomes in low and middle income countries (LMICs), as cases overwhelmed health systems and control measures prevented patients accessing healthcare.
WHAT THIS STUDY ADDS
This study adds evidence on how one LMIC, Sri Lanka, leveraged a strong health system to substantially mitigate the impact of COVID-19 on its health services and healthcare access and at least initially control transmission, while tracing the complex dynamics between epidemic control, health system impact and health outcomes.
Using a range of evidence and key informant interviews, it explains how Sri Lanka successfully implemented a Zero-COVID strategy but failed to sustain it owing to a failure to understand the critical role of symptomatic testing in that approach.
HOW THIS STUDY MIGHT AFFECT RESEARCH, PRACTICE OR POLICY
This study adds evidence on how strong public health capacities, robust healthcare delivery systems and intersectoral action are critical inputs for pandemic response, but also how civilian–military interaction, even if beneficial, can be contested, and how lack of fiscal space can undermine the overall response.
Sri Lanka’s experience shows clearly that pandemic preparedness and even luck cannot guarantee a successful pandemic response, and that policy and research need to pay more attention to improving decision-making processes when faced with pandemics involving novel pathogens, rapid spread, and substantial scientific uncertainty.
Introduction
Sri Lanka is a lower-middle income country (LMIC) in South Asia, with 22 million people living in a 66 000 square kilometre island, with a life expectancy at birth of 76 years in 2019 ( online supplemental table 1 ). Sri Lanka is advanced in its demographic and epidemiological transitions. Prior to the COVID-19 pandemic, it had eliminated several infectious diseases, including polio, malaria and measles, and its disease burden was dominated by non-communicable diseases (NCDs) with a high prevalence of diabetes. 1
Supplemental material
Sri Lanka’s health achievements, among the best for a country at its income level, are enabled by high levels of healthcare access. 2 Use of medical services, hospital capacity and immunisation coverage levels are comparable to high-income countries. Owing to low levels of government health spending (~2% of gross domestic product (GDP)), this is achieved through a mixed health system of parallel and independent public and private sectors. 2 3 All Sri Lankans have universal access to free public healthcare, which is financed from general revenue taxation, but can opt out to seek private care, with richer patients more likely to do so than poorer ones. The private sector provides half of outpatient care, and about 5% of inpatient admissions, with the government providing almost all preventive services including immunisation.
Sri Lanka detected its first COVID-19 case at the border in late-January 2020, before a gap of 6 weeks and the next wave of imported cases. Sri Lanka responded by building on its health system strengths. It experienced successes and failures. This study examines its experience, identifies key factors, and derives lessons for Sri Lanka and other countries.
We first outline the data sources and methods we used to examine the COVID-19 response and maintenance of health services. We describe the national strategy and then specific activities. These include coordination, epidemic control, vaccination, public communication and information sharing, management of health services and economic support. We then evaluate some core actions, before discussing our overall findings and conclusions.
Data sources
Our study used diverse data sources. We reviewed online news articles, government documents and circulars and reports shared by stakeholders and key informants. We reviewed situation reports, guidelines and data from websites maintained by the Ministry of Health (MOH), MOH Epidemiology Unit and MOH Health Promotion Bureau, and social media postings by government departments.
We conducted key informant interviews (KIIs) with 22 individuals involved in the COVID-19 response during March–August 2022, to obtain additional information and perspectives. Key informants (KIs) included government officials, politicians, health professionals, business and union representatives, military leaders and other experts. We guaranteed KIs confidentiality unless they specifically waived this, and we are not disclosing the composition of KIIs by type and sector to prevent identification of individuals. The interview guidelines were customised for each KI and compiled from a question bank covering a range of study topics. We obtained a positive response from all KIs approached, including politicians, health professionals, business, unions, the military and former MOH senior officials, except for the MOH which did not give permission to interview serving senior officials.
We used several data sets. These included data sets maintained by the Institute for Health Policy (IHP) and previously described, 4 which tracked metrics of the COVID-19 pandemic and response both globally and in Sri Lanka, collating data from public data sources. To assess the impact of COVID-19 on public well-being, healthcare use and opinion, we used survey data collected by the Sri Lanka Health and Ageing Study (SLHAS) during 2018–2022. The SLHAS is an MOH-approved, national longitudinal cohort study. Its Wave 1 survey recruited, interviewed and examined a nationally-representative sample of the adult population in 2018/2019 just before the pandemic started, 1 and Wave 2, conducted by computer-assisted telephone interview during 2021/2022, reinterviewed Wave 1 participants and an additional sample of adults reached by random digit dialling. 5
We modified a routine survey of private hospitals run by the IHP to ask additional questions on COVID-19 service provision. We also obtained data by request from government agencies and the military, and via Right to Information (RTI) requests submitted to the MOH.
Our study pursued several lines of inquiry, informed by the research design of the overall multicountry study. 6 We used an epidemiological framework and relevant literature from countries that pursued similar strategies to assess the data on cases, deaths, testing and vaccination, and other Sri Lankan studies, to characterise the epidemiological dynamics of the pandemic in Sri Lanka. We assessed the government response by characterising its explicit and implicit strategies, and how these changed over time. We paid specific attention to the strategies used and their effectiveness: (1) to control transmission; and (2) to mitigate impacts on health services, the economy and public well-being. To assess impact on services we used SLHAS survey data to quantify unmet need, and we examined inequalities in access to COVID-19 testing and vaccination, using concentration indices, multivariate regression and survival analysis. All analyses were performed using statistical software Stata V.17.0 (StataCorp, College Station, Texas, USA).
We also considered what motivated policymakers to adopt critical strategies, how strategy was communicated to the public and public opinion as tracked by the SLHAS.
Patient and public involvement
KIIs included private business and unions but did not involve the public or patients. We used the SLHAS surveys to examine and elicit public opinion and experience in the population and chronic disease patients. We held a dissemination meeting in Colombo in April 2023, where key stakeholders, including representatives of civil society participated and provided feedback. Gates Ventures has published selected study results online. 7
Timeline and phasing
Figure 1 illustrates the epidemic curve for reported COVID-19 cases in Sri Lanka. The government’s strategies changed over time in response to changes in transmission and morbidity, and perceptions about its ability to control transmission and consequences for the economy. The pandemic’s impact on health services also evolved. To frame our analyses and to facilitate understanding of the complex dynamics of the pandemic, we divided the pandemic timeline in Sri Lanka into successive 6 month phases, considering changes in epidemic transmission and response strategies in each period (see online supplemental text 1 for detailed characterisation and explanation).
- Download figure
- Open in new tab
- Download powerpoint
Daily COVID-19 cases, January 2020 to March 2022.
Phase 1 (January 2020 to June 2020) covers the first outbreaks, all of which were ended. Phase 2 (July 2020 to December 2020) corresponds to the start of sustained local transmission, which remained undetected for months before manifesting in the Brandix outbreak, which was a large outbreak in October 2020 that was associated with a garment manufacturing factory owned by the Brandix company. Phase 3 (January 2021 to June 2021) saw government’s strategy switch from stopping all outbreaks to vaccination and opening borders, with less emphasis on preventing transmission in the face of the Alpha variant. In Phase 4 (July 2021 to December 2021), the country was hit by the Delta variant, resulting in thousands of deaths ( online supplemental figure 1 ), significant pressure on health services and abandonment of most control measures, although the government reluctantly imposed a 2-month national lockdown. Phase 4 also saw most of the adult population being vaccinated with two COVID-19 vaccine doses. In Phase 5, which continues through 2022, successive Omicron waves hit the country, and the country’s attention shifted to the consequences of a collapse in the economy. COVID-19 testing largely stopped during Phase 5, and case numbers no longer provided meaningful information about transmission levels.
Although official cases (which required a positive PCR test) were only 587 245 (3% of the population) through end-2021, it can be inferred from epidemiological analysis, seroprevalence studies, low PCR testing rates ( online supplemental figures 2–3 ) and global experience that most Sri Lankans had been infected at least once by that point, and that actual deaths (14 979 reported) were more than 20 000.
The control strategy
Sri Lanka was better prepared for the COVID-19 pandemic than most countries. Enabling factors included having minimal exposure to the initial outflow of the virus from China ( online supplemental figure 4 ); being an island with one international airport; having a public health workforce with substantial experience in contact tracing and infectious disease control; a military that was able to rapidly establish border quarantine facilities; and a public with high levels of trust in the health system ( online supplemental text 2 ).
Through Phase 2, Sri Lanka aimed to minimise the entry of the SARS-CoV-2 virus through border controls, and to detect and rapidly end outbreaks to prevent any sustained local transmission to minimise health, social and economic impacts. The government’s official strategy of stopping all outbreaks 8 resembled that of a few, mostly East Asian and Pacific, countries that attempted to prevent sustained community transmission. Key interventions were similar to those of New Zealand, the country which most clearly articulated what has been dubbed the ‘Zero-COVID’ approach 9 10 : (1) border controls to minimise entry of the virus; and (2) PCR testing in the community, tracing of contacts of detected cases and isolation to detect and stop local transmission chains and to provide an exit from lockdowns. This was supplemented by extensive public health and social measures (PHSMs) to slow transmission.
Sri Lanka’s approach, explicitly fashioned after the ‘Hammer and the Dance’ approach proposed in an online article by an American analyst, 11 arose from its initial advantages and success in stopping outbreaks. It was supported by many local health experts and internal research on international responses by the military, and advocated for by the doctors’ trade union, the Government Medical Officers Association (GMOA). However, KIIs could not identify who initially proposed this approach.
During Phase 2, epidemiological inference and genomic analyses 12 indicate that cryptic sustained local transmission started sometime around June/July 2020, becoming visible in October 2020. As case numbers increased, most political leaders and health officials became fatalistic about the inevitability of spread, and came under increasing pressure from business interests, particularly in tourism, to tolerate transmission. Control efforts unravelled, with relaxation of border security and testing, contact tracing and isolation efforts. This implicitly abandoned the official strategy, but the government never officially announced this or explained coherently its new strategy. Though Phases 3 and 4 in the face of high levels of transmission, focus shifted to mitigating impacts on health services and the economy. From then the public health response focused on vaccination, with the USA and the UK being role models for President Rajapaksa.
Strategic actions
Coordination.
In March 2020, the government established two coordination mechanisms. The Presidential Task Force for COVID-19 provided a coordination forum of government agencies, health agencies and other stakeholders to discuss strategy and policy. The National Operations Centre for Prevention of COVID-19 Outbreak (NOCPCO), headed by the Army Commander, coordinated preventive, control, quarantine, and other pandemic-related operations.
The government generally excluded non-governmental entities and independent technical experts, other than business groups and health sector stakeholders, from these mechanisms. The largest Sri Lankan community service organisation, Sarvodaya, independently coordinated and led a collective of civil society organisations (CSOs) to provide social support to the community.
Epidemic control measures
Border security.
Through end-2020 (Phases 1–2), Sri Lanka implemented a strict border security regimen to prevent entry of the virus. This included suspension of visas for foreigners, mandatory 14-day quarantine for all arrivals with PCR testing, and suspension of routine commercial flights from mid-March 2020 to January 2021. 13 14 KIIs revealed that political leaders entrusted the running of quarantine facilities to the military, as health authorities lacked capacity to rapidly set these up and later to run them. Government quarantine was free, but from 2021 authorities allowed the private sector to operate paid quarantine facilities with better accommodation. During 2020–2021, the military operated 233 quarantine facilities for returning Sri Lankans, and the private sector established 119 paid facilities. This system processed 249 797 international arrivals of which 80% stayed in government facilities.
In Phase 3, from end-2020, the government allowed entry of tourists with restrictions. From April–June 2021, border controls and restrictions for all arrivals were incrementally relaxed, although tourist numbers did not recover rapidly owing to depressed global tourist travel ( online supplemental figure 5 ).
The border security regime was effective in minimising entry of the virus until the end of Phase 2, when this remained the strategic priority. The inclusion of PCR screening served to reduce the risk of hidden infection leaks, which would have been 1% with simple 14-day quarantine. 15 Despite several hundred thousand arrivals (mostly returning Sri Lankans), there were few outbreaks (<10) due to imported infections, a performance comparable with Zero-COVID countries such as China, Vietnam, Bhutan, Australia and New Zealand. However, a culture of defensiveness and lack of openness to independent scrutiny led to unwillingness to admit to or to audit potential quarantine leaks, limiting improvements.
Testing, tracing, and isolation
From Phase 1, MOH instigated an intensive test, trace and isolate (TTI) effort, coordinated by the MOH Epidemiology Unit, and implemented by the cadre of 2800 public health inspectors (PHIs) attached to local preventive health units. The State Intelligence Services (SIS) provided support, particularly in leveraging use of mobile device data and other big data for contact tracing. Through 2020, identified cases and contacts were placed in institutional isolation or quarantine in government hospitals. During Phases 1–2, TTI was effective, as evidenced by the identification of an average of 20+ contacts for each new case, and termination of all but one community transmission chain. Enabling factors included the prior experience of public health staff with contact tracing, interagency collaboration, reliance on PCR tests and the policy of tracing all upstream and downstream, first and second level contacts, an approach pushed by key stakeholders, such as the GMOA. The choice of PCR testing over rapid antigen tests (RATs) was crucial, as it allowed the detection of old infections, which was needed for contact tracing in the Zero-COVID-type approach. 16
From Phase 3, with abandonment of the control strategy and shortages of PCR kits for PHIs, the TTI effort weakened. From June 2021 asymptomatic or mild cases were isolated at home, with community supervision by healthcare workers. In Phase 4, contact tracing and isolation efforts essentially stopped.
Testing capacity
Sri Lanka established domestic testing capacity for SARS-CoV-2 virus early, benefiting from technical collaboration with Hong Kong experts, and pre-existing PCR capacity at local universities and the TB control programme. Health authorities expanded capacity by organising a national network of testing laboratories, including hospital, university, private sector and military laboratories, supported by centralised procurement and distribution of supplies.
Expansion in capacity slowed after the first wave of cases were controlled. By end-2020 testing capacity and rates fell far below those of other middle-income countries, and closer to that of poorer low-income countries ( figure 2 ). This was a policy choice and not the consequence of resource constraints. Senior health officials, whom the President, other political leaders and the military deferred to on this issue, did not think it necessary to increase capacity, despite vocal criticism by the GMOA, Public Health Inspectors Union (PHIU) and other local experts. Officials were also often reassured that testing was adequate by WHO staff and other experts. KIIs advised that political leaders would have found funds if asked, and the World Bank provided funds in May 2020 which were available to purchase urgent testing equipment and supplies ( online supplemental text 3 ) but were not fully spent through 2022. Local Rotary clubs raised funds to purchase large, automated testing machines, and private sector informants disclosed they were willing to fund these if the MOH had wanted.
PCR testing in Sri Lanka in global comparison, January 2020 to April 2021 (monthly tests per 1000 people). Notes: Authors’ analysis of Institute for Health Policy Global COVID-19 Testing database. Zero-COVID countries include Australia, New Zealand, Hong Kong SAR (China) and Singapore. High-income countries exclude the four Zero-COVID territories.
When case numbers increased rapidly at the end of Phase 2, the testing system was overwhelmed leading to pressure to relax the criteria for testing. Its capacity was limited by too few test machines, failure to adopt innovations such as saliva testing and large-scale test pooling, and failure to automate processes leading to huge pressures on staff.
Through Phase 2, case detection relied on PCR tests. Testing was publicly financed and free. In Phase 3, as financing became inadequate, the MOH let private laboratories undertake PCR testing for private patients. This led to concerns about private hospitals price gouging or saving costs by test pooling, which led to a ban on private sector test pooling, and in August 2021 a price cap of US$33 per test. 17 RATs were introduced in December 2020 to supplement PCR testing. As cases surged through 2021, MOH shifted to relying more on RATs and less on PCR tests. 18 However, the retail sale of RATs to consumers was not permitted.
Social distancing, lockdowns, mobility restrictions and masks
The government employed social distancing measures to reduce transmission. These included lockdowns, closures of schools and universities, limitations on gatherings and public messaging on maintaining interpersonal distances in public spaces. In Phase 1, there was a national lockdown for 1 month, but subsequent lockdowns were generally more localised. Google and Facebook mobility data indicate generally high public compliance in response to these ( online supplemental figure 6 ), comparable to other countries. In Phase 4, when the Delta variant caused the biggest wave, the government resisted intense public clamour to impose a lockdown, and when it did, it provided exemptions to numerous sectors. Nevertheless, the public strongly supported the national lockdown, preferring it to have been imposed earlier and more stringently, and supporting stronger measures ( online supplemental figures 7–8 ).
Educational institutions remained shut between lockdowns. Schools were closed for 17 months, one of the longest periods in the world ( online supplemental figure 9 ). Masks were mandated in public from October 2020, by which time supplies were established. 19 The mask mandate was lifted in June 2022, 20 and Facebook survey data indicate good compliance ( online supplemental figure 10 ).
Vaccination
Sri Lanka implemented an aggressive vaccination effort in 2021 to vaccinate all adults. This was facilitated by a robust national immunisation programme that routinely achieved near universal coverage of childhood vaccines, political support for procuring adequate vaccine supplies, minimal vaccine hesitancy, logistics support by the military and high levels of trust in the health services and military ( online supplemental text 4 ).
Through early-2021, the State Ministry of Primary Health Care Epidemics and COVID Disease Control pushed for ambitious coverage targets covering all adults, and self-purchasing vaccines instead of relying on COVAX. There was public criticism of delays in placing orders, but public sector procurement rules did not permit advance purchasing of vaccines not approved by the WHO and the local National Medicines Regulatory Authority (NMRA). The Cabinet approved purchasing vaccines using Treasury funds in February 2021, and the government later secured World Bank and Asian Development Bank (ADB) loans for additional vaccines. While awaiting delivery of purchased and COVAX vaccines, the government also obtained donations of vaccines from China, which eventually dominated supply ( online supplemental text 5 ). After a delay in approvals by the NMRA, which required WHO approvals, large supplies of Sinopharm vaccines were administered from July 2021, with newly imported stocks typically given out within days, leading to rapid increases in coverage ( online supplemental text 5 ). Adult one dose coverage reached 50% by late-July 2021, and two dose coverage reached 95% by mid-March 2022 ( online supplemental figure 11 ).
Although health officials raised concerns about vaccine hesitancy in the youth and a negative impact of social media, SLHAS survey data indicate minimal hesitancy ( online supplemental text 5 ). Vaccine hesitancy was even less in the youth in practice, with delays driven only by brand preference for Pfizer, which led people to wait for availability. However, uptake of the third booster dose was lower, which may have contributed to much higher mortality in 2022 (figure 4).
Given the need for rapid deployment and competing demands on preventive health staff to handle TTI, the military played a critical role in assisting MOH clinics and they set up vaccination centres (some open 24 hours) and mobile units to reach people with restricted mobility. Military-operated vaccination centres, staffed by 5200 personnel, delivered 2.4 million vaccinations. The military also designed and managed an electronic COVID-19 vaccine register, as the MOH lacked capacity to establish and maintain one.
Public communication and information sharing
The crisis forced authorities to engage in unprecedented levels of public communication, involving multiple channels and multiple actors in government. Much of this developed reactively during the crisis, and significant gaps and weaknesses were apparent.
The authorities used daily media briefings to provide the public with updates, which were widely covered by television, radio, print and social media. Though initially led by the Director-General of Health Services (DGHS), the Army Commander and head of NOCPCO became the lead spokesperson in Phase 2, after the incumbent DGHS was transferred without immediate replacement. Unlike in many countries, elected politicians rarely led media briefings.
As the government implicitly abandoned its elimination strategy, health officials increasingly understated the risk of COVID-19. Official health spokespeople overestimated the ability of the authorities to control the virus and the benefits of vaccination, while understating uncertainties in knowledge. We could not determine if this was due to political pressure to underestimate risks, or a desire to comply with perceived political wishes, or a desire to minimise public anxiety, or whether this represented their own beliefs; the MOH did not approve a request to interview relevant officials as KIs. However, KIs disclosed that when some officials or ministers took a more pessimistic public position or called for more aggressive control, they were often sidelined or scolded privately.
Data collection and reporting in relation to the pandemic was handled chiefly by the MOH, principally its Epidemiology Unit, and NOCPCO ( online supplemental text 6 ). Although Sri Lanka has RTI legislation to make government data accessible to the public, the culture of data sharing and transparency is underdeveloped, and most government data were not shared. Often regular data releases were made only to media representatives, and not directly to the public limiting wider access. Public authorities never published detailed test statistics as some other countries did, although these data were available. This also hindered decision-makers, with some KIIs within the government complaining of data hoarding by key MOH units.
There were controversies about the transparency and accessibility of the data that were released to the public. 21 In one instance when the daily COVID-19 death toll passed 100, the President intervened to change how the MOH reported COVID-19 death statistics. Although there were some legitimate arguments to justify changes, the impression was that political leaders wanted to downplay the number of deaths ( online supplemental text 6 ). Health authorities were also slow to counter misleading or stigmatising information from other stakeholders, including ministers and civil society. For example, many ministers extolled the untested treatment pushed by a charlatan, and some unions and politicians singled out Muslims as sources of infection.
This affected vaccination. Through 2021, authorities conveyed the message that two COVID-19 vaccine doses would protect people and achieve herd immunity, without conveying their limitations that were already known by the scientific community. This likely hindered later uptake of COVID-19 boosters.
Maintaining health services and health system resilience
During Phases 1–2 after the first national lockdown, COVID-19 had minimal impacts on health services when local transmission was minimal, 22 but significant disruption with negative impacts on health outcomes occurred in Phases 3–4 when the country was hit by the Alpha and Delta waves.
Management of patients with COVID
During Phases 1–2, MOH designated specific public hospitals for COVID-19 positive cases. As cases surged in Phase 3, health authorities established intermediate COVID care centres (ICCs) for asymptomatic and stable patients with COVID-19, 23 with the military contributing personnel. During Phases 3 and 4, the MOH authorised private hospitals to manage patients with COVID-19 and to run their own ICCs, but this was accessible mainly to affluent patients.
Generally, the public sector had sufficient intensive care unit (ICU) beds (expanded from an initial 560) but had to expand capacity substantially during Phase 4. The military contributed with rapid construction of additional facilities. The MOH leveraged an existing monitoring system to optimise ICU bed allocation for both COVID-19 and other patients. The national ambulance service also played a critical role in transporting patients.
Hospital and clinic service delivery
During Phases 1–2 and except for the first national lockdown, health authorities maintained normal operations in public clinics, facilitating access for healthcare workers and patients with curfew passes and staff transport. 24 Later, hospitals used RATs to screen new admissions to minimise in-hospital transmission.
After initial disruptions caused by mobility restrictions and closures due to fear of COVID-19, the MOH proactively restarted and maintained maternal and child health and immunisation services at Medical Officers of Health clinics. 25 The MOH instructed clinics to remain open and provided guidelines to mitigate infection risks, with provision to substitute infected public-health midwives. 26 During 2021–2022, it largely cleared immunisation backlogs from 2020 ( online supplemental table 1 ). 27 28 The public sector exclusively managed suspected/confirmed pregnant/postpartum mothers and newborns, with COVID-19 positive cases sent to a designated national centre for management. 29
Routine services were only substantially affected during the Alpha and Delta waves, when substantial local transmission occurred. During the Delta wave, pressure on beds and staff shortages due to COVID-19 infection were overwhelming, leading to suspension of non-emergency care. Despite this, Sri Lanka’s historical prioritisation of hospitals in public spending limited the impact, 2 as it had hospital bed capacity (4.2 beds per 1000 capita) several times more than the average in middle-income (2.3) and South Asian (0.6) countries and more comparable to that of high-income countries (5.2). 30
Preventive service delivery
Preventive health activities were disrupted as public health staff were mobilised to contain COVID-19 transmission and later to administer vaccinations, despite MOH instructions to maintain routine services and military assistance. 31 Fortunately, closed borders, reduced mobility, social distancing and masks reduced other infectious disease transmission. Dengue fell to one quarter of predicted levels during March 2020 to April 2021, 32 despite reduced control activities. It helped that dengue vector breeding sites are often located in workplaces like construction sites and schools. 33
During Phase 1, senior MOH managers acted proactively to maintain supply of medicines, particularly for patients with chronic conditions. They reached out to the private sector to understand the challenges private distributors faced and to identify supportive measures, an unprecedented move by a public sector that rarely worked with the private sector.
The MOH revised regulations to allow 2 months’ medication supply for MOH outpatients instead of 1 month. It introduced temporary postal delivery for registered patients. 34 Private sector patients with NCDs were allowed to obtain medicines at government hospitals if unable to reach their usual private hospital. 35 Private pharmacies were permitted to stay open during lockdowns, to deliver medicines directly to homes and to accept prescriptions sent by electronic means.
Public awareness of the new distribution mechanisms was high. SLHAS Wave 2 data indicate that 30% of adults needed a regular medication refill, of which 85% were aware of the MOH postal delivery mechanism, and 33% of them had benefited from it, with 90% reporting satisfaction. Additionally, 40% of adults needing refills knew that private pharmacies offered home delivery, although only 5% of them had used this option ( online supplemental figure 12 ). However, foreign exchange shortages and fiscal constraints began to impact overall medicines supply from 2021.
There were several initiatives to develop telehealth services to improve access, which expanded use of remote consultation from almost zero. Many MOH clinics provided consultations by telephone, including using algorithms to remotely screen possible COVID-19 cases. 36 The University of Kelaniya developed a system to facilitate primary care teleconsultations by phone and WhatsApp, which other public sector facilities adopted. 36 Private channelling companies, which act as booking agents for private specialists, and private providers allowed patients to remote consult specialists via video or audio. Internet bandwidth was increased at many public facilities, and telecom providers provided equipment, software and additional bandwidth to MOH facilities, often free.
Remote consultations surged during national lockdowns when mobility restrictions made access to private providers difficult. Private channelling industry sources reported that teleconsultations grew from zero to peak at 35% of consultations in March 2020, before averaging 5–10% of consultations during October 2020 to October 2021. SLHAS Wave 2 data indicate that remote consultations remained at 5–12% of outpatient encounters through 2022, suggesting a permanent increase in telehealth service usage.
Impacts on healthcare access and use
We assessed impacts on healthcare usage using provider data ( online supplemental text 7 ). In 2020 inpatient admissions declined by a fifth (public sector −18% and private sector −26%), while outpatient visits dropped by a third (public sector −32% and private hospitals −23%) compared with 2019. Usage partially recovered in 2021, with available data indicating a 17% reduction in private hospital admissions and an 18% drop in private hospital outpatient visits compared with 2019.
We assessed the impact on unmet healthcare needs with SLHAS data following the same approach that the European Union (EU) uses with its EU Statistics on Income and Living Conditions survey ( online supplemental text 7 ). Unmet needs for medical care, dental care and medicines in the previous 12 months increased substantially from 2019, rising from 4%, 4% and 5% of adults to 17%, 14% and 20%, respectively, in 2021/2022. The end of the August to October 2021 lockdown and waning of the Delta wave led to improvements ( figure 3 ). During August 2021 to January 2022, COVID-19 was a bigger barrier than cost factors. Primary reasons were (1) fears of catching COVID-19 or being diagnosed with COVID-19 (40%), and (2) mobility restrictions and transport barriers during lockdowns (26%), versus (3) cost barriers (37%). Poorer Sri Lankans were less likely to cite fear of COVID-19 as a barrier, reducing overall inequality in unmet need in 2021/2022 compared with 2019. Patients with chronic NCDs reported more unmet need for medicines, indicating that mitigations efforts were not completely successful.
Unmet need for medical care due to financial costs, travel barriers, waiting times, unavailability or COVID-19 (% of adults, past 4 weeks), September 2021 to May 2022. Notes: Percentage of adults (14 days moving average) reporting unmet need due to financial costs, travel barriers, waiting times, lack of service availability and fear of COVID-19. Authors’ analysis of Sri Lanka Health and Ageing Study Wave 2 data, weighting to match national population. Wave 2 interviews (N=4606) conducted September 2021 to May 2022.
Economic support and policies
Government financed its response mostly from its own resources, with foreign assistance most important for health interventions. Key international funders were the World Bank, ADB, China, India and Japan ( online supplemental text 3 ). 37 38
During Phases 1–2, household and business hardships mainly resulted from PHSMs, especially mobility restrictions, and reduced export earnings. These most affected informal and daily workers, and industries such as tourism. The government implemented initiatives to assist households ( online supplemental text 8 ) 8 39 : cash grants or food rations for low-income, elderly, COVID-19 or lockdown affected households; and extended deadlines for utility and credit card payments. CSOs also organised assistance but this was less likely than government assistance to reach the poorest households ( online supplemental text 8 ). Business support focused on tax concessions, with some assistance in accessing loan facilities. However, overall public economic support to businesses and households was small, less than 1% of GDP, 40 compared with 3–10% of GDP in most developing Asian countries. 41 Beneficiary households typically received just US$25–100, with no direct business support beyond tax concessions, unlike other countries ( online supplemental text 8 ).
The weak economic support measures were the inevitable consequence of the government’s constrained fiscal capacity. 42 43 Decades of low taxes and tax cutting policies had led to twin fiscal and current account deficits, financed in the 2010s through increased foreign commercial debt. This left the economy ill-prepared for the COVID-19 shock: no fiscal reserves, low foreign exchange reserves and dwindling access to foreign financing. Sri Lanka started the pandemic with government revenue at just 12% of GDP, a fiscal deficit of 9% of GDP, public debt at 89% of GDP and foreign debt at 39% of GDP ( online supplemental table 2 ). The new government in 2019 compounded this. It implemented substantial tax cuts and maintained an overvalued exchange rate. This reduced revenues to 9% of GDP and foreign reserves to just 3 months of imports and raised the fiscal deficit to 11% of GDP and public debt to 104% of GDP in 2020. Failure to reverse fiscal and monetary policies when COVID-19 hit left the government in a fiscal straitjacket with no room for significant spending.
COVID-19 worsened Sri Lanka’s problems. It reduced foreign exchange earnings from tourism, exports and migrant remittances, and reduced tax revenues ( online supplemental table 2 ). While the initial COVID-19 strategy in Phases 1–2 mitigated any damage, lack of fiscal space led policymakers to prioritise perceived immediate economic needs over control of the virus, which contributed to the unravelling of the COVID-19 strategy from 2021.
Underlying economic issues may have undermined the public health response in other ways. Low taxes had limited the government health budget to under 2% of GDP for decades. 2 3 42 44 This shaped a medical culture that was averse to spending on laboratory tests and less receptive to appreciating the importance of testing for controlling viral transmission.
Evaluation of key actions
Covid-19 control strategy.
Sri Lanka’s control strategy requires evaluation at two levels: (1) strategic, and (2) implementation.
Sri Lanka’s initial official COVID-19 control strategy aimed to prevent sustained local transmission. 8 This largely worked in 2020, but from 2021 Sri Lanka changed tack and experienced sustained local transmission. Given the unreliability of testing data, Sri Lanka’s success in controlling COVID-19 and protecting population health must be evaluated by examining its impact on overall mortality ( figure 4 ). The crude death rate fell from 6.7 deaths per 1000 persons (2019) to 6.0 in 2020, before increasing to substantially above the pre-COVID-19 baseline in 2021 (7.4) and 2022 (8.1). 45 The initial fall was in line with experience in successful Zero-COVID countries. But the subsequent increases, equivalent to over 30 000 excess deaths over the whole time period, resembles more the experience of the UK and USA ( online supplemental table 3 ).
Changes in crude death rates for Sri Lanka and selected countries that pursued Zero-COVID approach, 2015–2022. Source: Compiled by authors using data from Department of Census and Statistics, Sri Lanka; Australian Bureau of Statistics, Australia; National Bureau of Statistics, China; General Statistics Office, Vietnam; Statistics New Zealand, New Zealand; and World Bank World Development Indicators. Full details given in online supplemental table 3 .
Why did policymakers abandon the initially effective strategy, which played to Sri Lanka’s strengths? The immediate reason, confirmed by KIIs, is that the outbreak that became visible in late-2020 was too large to control with the interventions attempted. As political leaders lost faith in the health authorities’ ability to control the virus, they aligned with competing voices that argued that the economic costs of preventing transmission were excessive and that such efforts were doomed to failure. This raises the question of why the control strategy failed to stop the late-2020 outbreak before it reached such levels?
It is necessary to reference the insights of Australian and New Zealand epidemiologists that underpinned their more successful Zero-COVID strategies. 16 46 Ironically, these were informed by a preprint published in April 2020 by a Sri Lankan Australian researcher and colleagues. 47 They anticipated that even the best border security regime would fail frequently, and prevention of sustained local transmission depended on early detection of cryptic chains of transmission within the community. Modelling indicated that the most feasible option for achieving this involved intensive PCR testing at the primary care level of people with coughs, colds and respiratory symptoms, followed by downstream and upstream contact tracing. Both countries estimated independently that this required testing rates of approximately one test per 1000 capita daily to detect hidden outbreaks while they still numbered fewer than 20 infected persons, that is, small enough to be controlled. Sri Lanka’s strategy never met these requirements. While its border security and contact tracing performance matched these countries, Bhutan and Vietnam, testing rates never exceeded 0.2 tests per capita or 3500 tests per day before detection of the Brandix outbreak ( online supplemental figure 2 ). This was substantially lower than Bhutan and Vietnam, both poorer LMICs, and testing was less effective focusing on random testing and hospital patients. The Australian and New Zealand modelling imply that with such an inefficient and inadequate testing policy hidden transmission chains seeded by a single imported infection would persist for months and infect several hundred people before detection, which matches the Brandix outbreak. Genomic sequencing and back forecasting of the epidemic curve support this inference, both indicating a quarantine leak in mid-2020.
If epidemiology can explain the failure of the control strategy, it does not explain why Sri Lanka maintained such a low testing rate, given that it had access to both government and donor financing, and given frequent and often strident public calls by many local health experts and stakeholders to increase testing. KIIs with a range of health, military and other sources revealed that policymakers and the experts advising them were unaware of the Australian and New Zealand analyses and that the testing strategy was unlikely to achieve the desired goal. We found no evidence of any efforts to quantify an adequate testing rate, despite stakeholder concerns. KIIs and media reporting indicate that a general sense of complacency prevailed, reinforced by reassurances by staff of international agencies and trusted foreign and local experts that testing was adequate through 2020.
While the overall strategy was based on a technical paradigm, although flawed, with significant influence from technical experts, detailed implementation of strategy was often disrupted by a wide range of stakeholders and political interests. This was facilitated by longstanding governance weaknesses which permitted formally technocratic processes to be subject to undue political and social influences. Two specific examples illustrate this.
One was the vaccination rollout, initially detailed by technical committees working to international guidelines. However, during implementation, stakeholders and even officials often subverted the agreed-upon phasing to favour specific groups. Although this interference did not have a major impact on the overall phasing of coverage, they generated public criticism and eroded trust in the vaccination process. A second example was the prolonged dispute over the forced cremation of COVID-19 deaths, which caused considerable anguish to the Muslim community and damaged Sri Lanka’s relations with several foreign countries. 48 This was not justified by the scientific evidence, but the MOH’s efforts to change the guidelines through review by expert committees encountered political pressures and inadequate objectivity by experts involved. 49 50
Coordination and the role of the military
The two government mechanisms to coordinate government agencies and stakeholders generally ensured cohesive implementation. MOH collaboration with the private medical sector functioned well most of the time and was unprecedented given a history of limited public–private collaboration. However, there were several weaknesses.
Civil society criticised the coordination mechanisms and the COVID-19 response for being excessively military dominated, or specifically dominated by the Army Commander. KI interviews and our assessment of the evidence revealed a complex situation. We found a significant degree of both policymaker and senior military deference to the technical advice of health staff. We found no evidence that the military made any substantive public health technical decisions, including critical errors in the design of the control strategy–in each case MOH personnel proposed the actions. However, some KIs reported that particularly during Phase 3 mid-level MOH personnel sometimes bypassed inappropriately the top-level MOH officials to brief and lobby military decision-makers, subverting decisions previously agreed by MOH at taskforce meetings. In these cases, both health and military personnel shared culpability for poor governance, and we speculate that weak MOH leadership failed to reassert lines of authority.
Nevertheless, the Army Commander had a prominent role, being the lead public face of the government and having the most influence within the taskforce, at the expense of MOH officials (from late 2020) and elected ministers. Several factors may have contributed to this: constitutional centralisation of executive authority in the President; a culture of deference of ministers to the President; and the inclination of President Gotabaya Rajapaksa, who had a military background, to delegate to military officers. While KIs noted negative consequences, such as unwillingness of many doctors in the taskforce to voice dissenting views, it is difficult to disentangle how much of this was ultimately driven by the role of the Army Commander and how much by the hierarchical, centralised decision-making that is the norm in Sri Lanka. At the same time, the removal of the senior-most MOH official by the President in mid-2020, left a lacuna which the Army Commander filled in the absence of a strong MOH leadership.
In several areas we assessed, for example, border quarantine, design and operation of the COVID-19 vaccination database, emergency construction of public facilities, military involvement was evidently necessary. This was because relevant public agencies or private contractors either lacked capacity to take on the function or could not be swiftly procured through government procurement procedures. Use of the military and intelligence services to handle mobile device data for contact tracing could not have been entrusted to other agencies owing to data protection and confidentiality concerns. In other areas, like vaccination support and military assistance to the police in enforcing mobility restrictions, the military provided reserve capacity which allowed civilian agencies to concentrate on other essential tasks. In the case of vaccination, even this support might have been inadequate, as the vaccination drive led to reductions in testing activities because public health staff were redirected to vaccination duties.
Another weakness in the coordination mechanism was groupthink. At critical points, there was inadequate questioning of assumptions, consideration of alternative perspectives and appreciation of the inherent uncertainties in the COVID-19 evidence base. Observation during KIIs suggests that the self-confidence of senior military officers, which may have been beneficial for implementation, was associated with inadequate sensitivity to risks and uncertainties (a known characteristic of the military mindset 51 ), which in turn may have influenced the taskforce deliberations. This was most apparent in the failure to increase testing in 2020, which was associated with failure to consider alternative views or to assess fully the risks.
Although the taskforce brought together many stakeholders, there was no representation by independent technical experts, nor adequate involvement of experts with expertise in subjects such as public communication, public opinion, and social behaviour.
Control interventions
Sri Lankans generally accepted imposition of lockdowns, mobility restrictions and mask mandates without significant social protest. Compliance was generally good, although this frayed with long lockdowns and as the pandemic persisted. The effectiveness of these PHSMs remains uncertain, and later lockdowns were less stringent. International research, including some done in Sri Lanka, has mostly found weak or no evidence for the effectiveness of lockdowns, 4 but it is unclear how familiar local experts were with this research. In Sri Lanka, lockdowns in densely populated, poor, urban areas often did not stop transmission, because of the difficulties for residents to isolate for long periods.
The public generally thought that testing access was adequate ( online supplemental text 4 ), but the decision to allow the private sector to offer testing was preceded by frequent calls by members of the public and by private sector providers to allow the private sector to offer testing. In analysis of SLHAS data ( online supplemental text 9 ), we found that use of all and private testing was pro-rich (all testing: concentration index, CI=0.04, p<0.0001; private testing: CI=0.03, p<0.0001), and that of public testing was not significantly unequal though there was a modest pro-rich gradient (CI=0.01, p=0.24). Concentration index analysis also found that testing was pro-rich when it was of close contacts (p<0.02) or symptomatic (p<0.09), and only pro-poor for random testing (p<0.001). We also found that women and Muslims were significantly less likely to be tested.
As COVID-19 vaccine coverage was high across the population, we used SLHAS data to analyse disparities in time to be fully vaccinated ( online supplemental text 9 ). We found that time to full coverage was largely equal with no disparities by sex, education, socioeconomic status quintile, sector of residence, being a healthcare worker or Facebook or WhatsApp use, once differences in when population groups became eligible was accounted for. However, we found that Muslims took longer to be fully vaccinated (p=0.01).
Public communication and public confidence
In routine public communication, elected politicians typically played a secondary role to health officials, with the Army Commander taking a lead role in his capacity as head of the taskforce. The consequences of this for actual pandemic control are complicated and difficult to evaluate. It is important to acknowledge that the role of the Army Commander raises normative issues outside our empirical analysis.
The military, health officials and health stakeholders enjoyed more credibility and public trust than political leaders, as evidenced in their higher favourability ratings ( online supplemental text 4 ). This may have facilitated public communication and reduced public anxiety. It was reflected in the public having more confidence than in other countries in the ability of the government’s pandemic team to manage the pandemic, and in the overall response ( online supplemental text 4 ).
Simultaneously, public distrust in government reports about the spread of COVID-19 was higher than most countries ( online supplemental text 4 ). This likely reflected the greater political influence on public messaging, as opposed to underlying strategy, and efforts to downplay negative news and uncertainties. Although political leaders and officials may have believed that avoiding bad news was sound strategy, it was detrimental. Public figures who vocally called for more aggressive action to control virus transmission, such as the state minister for COVID-19, the GMOA and the PHI union, generally enjoyed higher favourability ratings than the President, health minister and other political leaders who did not ( online supplemental text 4 ).
Overly optimistic messaging about the benefits of vaccination negatively impacted uptake of booster vaccination. Stigmatising and racist communication by politicians and stakeholders may have contributed to lower uptake of testing and vaccination by the Muslim community, although the effects were not large ( online supplemental text 9 ). In contrast, in SLHAS Wave 2 interviews conducted October 2021 to December 2022 (N=1430), the percentage of individuals reporting unmet need for medical treatment in previous 12 months was no higher among Muslim (9.6%, 95% CI 4.9 to 18.1) than in Sinhala respondents (9.7%, 95% CI 8.0 to 11.6).
The key challenge for countries at the start of the COVID-19 pandemic was how to minimise impacts on health, health systems and wider society, until such time that vaccination might provide an exit route. Sri Lanka’s performance was mixed. It did well during 2020 but performed badly in the following 2 years. Although healthcare use fell in 2020, it had minimal adverse health impacts and overall mortality fell. But in 2021–2022, disruptions to healthcare use and service provision led to increases in mortality, with a substantial reversal of prepandemic health gains ( figure 4 ). And although COVID-19 was not a fundamental reason, these failures in 2021–2022 contributed to the profound political and economic crisis that hit Sri Lanka in 2022, which led to the collapse of the government and economic bankruptcy, with continuing deleterious consequences for health and its health system.
This reversal was due to Sri Lanka’s initially successful strategy unravelling when it confronted the late-2020 outbreak that was too large for it to control. Most countries were unable to stop outbreaks from the initial pandemic wave, but Sri Lanka was one of a few countries that could and did. For most countries prevention of transmission was moot from early in the pandemic, but Sri Lanka retained this option through 2020. Its response must be evaluated from that perspective.
Several factors facilitated Sri Lanka’s positive performances, many of which it shared with successful Zero-COVID countries. This was not captured by assessments such as the Global Health Security Index, 52 confirming previously reported findings about its lack of correlation with COVID-19 pandemic performance. 4 Some factors were linked to core health system strengths. These included: strong public health capacities (infectious disease control, vaccination); a robust health system with large hospital bed capacity and universal coverage; genuine desire of health officials to protect access; and strong public trust in the health authorities, healthcare workers and vaccination. Fortuitous factors were being an island, reduced exposure to the initial Wuhan wave and reserve military capacity that could be mobilised to support public efforts.
These factors and an early border closure allowed Sri Lanka to end its first outbreaks, and for it to adopt a Zero-COVID approach in terms of goals. But its implementation failed within months. The Zero-COVID approach was a three-legged stool consisting of: (1) secure borders, (2) contact tracing and isolation and (3) intensive symptomatic PCR testing in the community. Sri Lanka implemented the first two, but not the third. This arose for several reasons. First, the experts responsible for the strategy were not aware of (and did not investigate) the epidemiological thinking behind the Australian and New Zealand approaches and did not attempt to assess technically what an adequate testing regime might be. Second, the decision-making process and linked technical experts suffered from groupthink, a culture of defensiveness and lack of openness to alternative ideas, which made them unreceptive to concerns, often public, expressed by other local experts. Third, longstanding resource constraints had bred a medical culture that was averse to spending on ‘unnecessary’ laboratory testing, and a health policy establishment that was accustomed to working within budgets and unaccustomed to making the case for additional money to political decision-makers. Fourth, in a situation where uncertain knowledge encouraged the use of heuristic shortcuts, the Anglophile medical and political culture in Sri Lanka led decision-makers to pay more attention to American and British thinking on the COVID-19 response, while ignoring the contrary thinking in Australia and New Zealand and elsewhere in East Asia, particularly China, which other regional countries benefited from. 53 This groupthink and lack of interest in East Asia parallels similar problems that the UK COVID-19 Inquiry has revealed, 54 and the cost-averse medical culture has similarities to that in Malaysia and Japan.
We can only speculate on why Sri Lanka did not overcome these problems. We suggest two reasons. One is that Sri Lanka’s historical health achievements were driven by continuous, incremental managerial improvements based on technocratic assessment of global evidence and trial and error within a stable framework. 55 This decision-making works well with long-term challenges, such as maternal mortality or hospital efficiency, but the OODA (observe, orient, decide, act) loop is too slow for an acute emergency such as COVID-19, where scientific knowledge is subject to large uncertainties and change. Sri Lanka’s chronically under-funded health system lacked spare capacity to process the incoming information and to think out-of-the-box. The second is that the political (and military) leadership relied too much on official health authorities and the WHO for advice and was too incurious to investigate alternative perspectives. One solution might have been provision for a ‘red team’ facility that generated independent critiques of strategy.
When considering COVID-19’s effects on health services, these were complex. We distinguished several pathways of impact. Two direct pathways were: (1) infection of healthcare staff, and (2) pressure on healthcare resources from sick COVID-19 cases. These only had substantial impacts in Sri Lanka during peaks in infection, such as the 2021 Delta wave, and these were partially mitigated by Sri Lanka’s substantial hospital capacity. Two indirect pathways involved ‘COVID anxiety’, which led patients to stay at home, and healthcare providers to adopt excessively precautionary behaviours. Both impacted access in Phase 1 in Sri Lanka (in addition to the effects of mobility restrictions), but although healthcare providers adapted, public ‘COVID anxiety’ continued to suppress healthcare use, only dissipating in 2022. In future pandemics, policymakers may need to do more to reassure the public, and to institute better protocols to prevent cross-infection in healthcare settings.
It is clear from the data on unmet need and healthcare use that all these effects significantly impacted service delivery and access throughout 2020–2022. However, increased mortality was only seen in 2021–2022. This suggests that the direct impacts are the most critical, consistent with control of transmission being beneficial in protecting health and health systems. Sri Lanka’s experience as a failed Zero-COVID country is instructive, since it enjoyed big mortality benefits from controlling transmission near zero but suffered large and continuing mortality losses when it gave up on stopping transmission.
Despite the strategic errors, Sri Lanka did well in implementation and mitigating impacts on health coverage. These include border security, contact tracing and isolation, medicines access, clearing childhood immunisation back-logs, managing ICU and hospital bed supply during waves, implementing COVID-19 safe protocols in healthcare, COVID-19 vaccination and intersectoral coordination and public–private collaboration. These positives were facilitated by pre-existing strengths of the health system, a cohesive national taskforce, trusting implementation to competent health sector and military managers and political willingness to draw on the military as the state’s human resource reserve.
We recognise that the military’s role is controversial in Sri Lanka. 56 57 However, KIIs and other evidence we reviewed indicate the need for a nuanced view. First, we note that considered discussion of the military’s role in Sri Lanka is challenging. Four decades of internal conflict that ended in 2009, during which survival of the state and civilian-led democracy often depended on the military, left a complex legacy of a large military establishment with significant organising capacities, a civil society with polarised views about the military and frequent suspicions about military motivations and a public with high levels of trust in the military. Many of the military involvements in the COVID-19 response, for example, in border security, vaccination, contact tracing, emergency construction, were contested by segments of civil society as excessive and undesirable militarisation, but paralleled the use of the military in established Western democracies. 58–60 Globally, military involvement was a double-edged sword which could strengthen the COVID-19 response but threaten citizenship rights and community trust so crucial for effective epidemic response. 61 In Sri Lanka’s case, we found that the military role was often necessary and overall a net plus in strengthening COVID-19 control. We could not assess its net impact on rights since this requires disentangling this from the inevitable restriction of liberties associated with many PHSMs, but the evidence revealed no negative net impact on community trust, with the public retaining high levels of confidence in the military ( online supplemental text 4 ). This leaves normative questions as to the appropriate role of the military in society, 61 but our empirical study cannot answer these, beyond simply noting that the Sri Lankan public’s positive view of the military should not be irrelevant in a democracy.
Sri Lanka did badly in other areas. Uptake of COVID-19 vaccine boosters was low, and 8 million expired Pfizer doses were eventually destroyed. 62 There was over-optimism in official messaging and reluctance to discuss uncertainties, both by health officials and political leaders. There was lack of transparency and sharing of data, and opaque decision-making processes with frequent failure to explain the basis of policies, despite Sri Lanka’s constitution enshrining the public’s normative right to information. This eroded public trust in COVID-19 communications, impaired accountability, contributed to poor decision-making and undermined local analysis which might have informed a better response. There are no easy remedies, as this reflects deep-seated problems of bureaucratic and political culture, and a society where demonisation of political opponents is often the norm making social discourse about common problems difficult. Practical actions might be providing systematic training to senior health officials on public communication when faced with pandemic uncertainty and how to better handle stakeholders including political leaders, and having facilities to bring in expert advice on communications. The bigger problems of lack of transparency, unwillingness to share information and narrow space to discuss common problems will require sustained pressure by political leaders and civil society to use RTI legislation to normalise transparency and efforts to strengthen dialogue.
Sri Lanka’s fiscal and foreign exchange constraints emerge as a consistent negative backdrop in our analysis. The government lacked money to provide significant economic support to mitigate the impact of PHSMs and contraction in global demand. This and dwindling foreign reserves contributed at the political level to the strategy shift from preventing transmission to living with the virus. Inflexible procurement processes motivated by chronic fiscal deficits delayed vaccine procurement. A health sector that had operated for decades under stringent fiscal constraints 3 lacked spare technical capacity to understand the epidemiology of COVID-19 control, was disinclined to invest in testing as a control intervention and was less motivated to push booster vaccination which would have reduced excess mortality through 2022. Although Sri Lanka entered an International Monetary Fund (IMF) adjustment programme in 2022 to tackle its fiscal problems, this might not improve Sri Lanka’s capacity for pandemic response. The IMF targets, which include raising taxes to a still low 15% of GDP, are the minimum to achieve sustainable debt repayment. 63 More ambitious revenue goals are required to increase health spending. These will not be adopted without wider social consensus and demands from health stakeholders, who have been silent or even opposed to raising taxes. 64
Conclusions
Sri Lanka’s response to COVID-19 was marked by successes and failures, which provide lessons for itself and other countries.
A well-functioning health system can give countries a significant advantage in facing pandemics like COVID-19. This includes strong public health capacities in infectious disease control including surveillance, contact tracing and epidemiological analysis; robust immunisation capacity with high levels of public trust; competent system managers to manage and balance service delivery in response to urgent demands; and substantial hospital capacity more than most LMICs. To this must be added fiscal capacity, which means adequate taxes, fiscal reserves and space to borrow in an emergency, to finance health interventions and economic support, something which Sri Lanka clearly lacked. And if fiscal capacity exists, countries must pre-emptively legislate procurement processes fit for pandemic situations.
Sri Lanka was fortunate to be one of a small number of countries that was able to stop the first pandemic outbreaks. Its initial pursuit and later abandonment of its Zero-COVID strategy carries several lessons. The first is that when this is feasible, preventing transmission of a COVID-19-like pathogen is in the long run better for public health, health services and society than tolerating sustained transmission, until such time that an exit route is available. The second is that the Zero-COVID approach could only work with all three components: secure borders, contact tracing and isolation and adequate symptomatic PCR testing in the community. Sri Lanka is an object lesson in what happens when the third element was missing. It suggests that for countries to have implemented this approach in 2020, they had to have sufficient technical capacity to independently work out the epidemiological underpinnings, since international advice was often wrong. 53
Sri Lanka’s experience adds to growing evidence on how groupthink by public health experts and policymakers often failed in the face of a pandemic characterised by pathogenic novelty and scientific uncertainty. Responding to such challenges requires avoiding heuristic shortcuts, such as treating COVID-19 like influenza, or simply relying on the usual role models. Finding mechanisms to minimise this risk should be a priority, and Sri Lanka would need to invest more in its own technical capacities, both within and outside government, and in efforts to increase transparency in both political and technical spheres.
Ethics statements
Patient consent for publication.
Not applicable.
Ethics approval
This study involves human participants and was approved by Institute for Health Policy Institutional Review Board (IRB/2022-31). Participants gave informed consent to participate in the study before taking part.
Acknowledgments
The authors thank their colleagues in the Sri Lanka Health and Ageing Study (SLHAS) consortium for making available data from the SLHAS Wave 1 and 2. We express our sincere appreciation to Jennifer Nuzzo, Moytrayee Guha and Lucia Mullen for their support on the Exemplars study, Anjana Senadeera, Natali Andrea and Navodi Hakmanage for their support on data collection, and the many key informants who provided valuable insights. We also thank two anonymous reviewers who provided valuable comments that helped shape the final version.
- Rannan-Eliya RP ,
- Wijemunige N ,
- Perera P , et al
- Sikurajapathy L
- Amarasinghe SN ,
- Dalpatadu KCS ,
- Rannan-Eliya RP
- Gunawardana JRNA , et al
- Rannan-Eliya R ,
- Dissanayake V ,
- Tanugi-Carresse AC ,
- Mullen L , et al
- Perera S , et al
- Government of Sri Lanka
- Kvalsvig A ,
- Verrall AJ , et al
- Jeewandara C ,
- Jayathilaka D ,
- Ranasinghe D , et al
- Ministry of Health
- Zhang M , et al
- Davis S , et al
- ↵ Face mask rule in Sri Lanka lifted . Ada Derana June 9 , 2022 . Available : https://www.adaderana.lk/news.php?nid=82958 [Accessed 15 Jun 2023 ].
- Jayasinghe C
- Arambepola C ,
- Wickramasinghe ND ,
- Jayakody S , et al
- ↵ Overview of immunization coverage during COVID-19 period, Sri Lanka ; 2023 . Available : https://www.linkedimmunisation.org/wp-content/uploads/2022/12/BBB_CountryPPT_SriLanka-1.pdf [Accessed 21 Aug 2023 ].
- Surendran SN ,
- Nagulan R ,
- Sivabalakrishnan K , et al
- Liyanage P ,
- Rocklöv J ,
- Primary Health Care Performance Initiative
- Ministry of Finance
- ↵ ADB COVID-19 Policy Database . Asian Development Bank ; 2022 . Available : https://covid19policy.adb.org/ [Accessed 30 Dec 2022 ].
- Asian Development Bank
- International Monetary Fund
- Department of Census and Statistics
- Schwehm M ,
- Sri Lanka Medical Association
- College of Community Physicians Sri Lanka
- Knighton RJ
- Nuclear Threat Initiative
- The Independent Panel for Pandemic Preparedness and Response
- UK COVID-19 Inquiry
- Dalpatadu S ,
- Wickramasinghe R , et al
- Nandakumar T
- Kazibwe J ,
- Quirk E , et al
- Gibson-Fall F
- ↵ 7.5Mn Pfizer vaccines expired! Sri Lanka Mirror Available : https://srilankamirror.com/news/7-5mn-pfizer-vaccines-expired/ [Accessed 1 Sep 2023 ].
- ↵ Sri Lanka income tax hike: GMOA to launch ‘black protest week’ on Jan 23 . EconomyNext January 3 , 2023 . Available : https://economynext.com/sri-lanka-income-tax-hike-gmoa-to-launch-black-protest-week-on-jan-23-108087/ [Accessed 30 Aug 2023 ].
Supplementary materials
Supplementary data.
This web only file has been produced by the BMJ Publishing Group from an electronic file supplied by the author(s) and has not been edited for content.
- Data supplement 1
Handling editor Seye Abimbola
Twitter @ravirannaneliya
Contributors RPR-E, SP, SS and KCSD conceived and designed the study. RPR-E, AG, MDN, SA, NWij, SP, SS and SF carried out data collection. RPR-E, NWij, NWis, SA, NK, AS, SF and TD carried out data analysis. RPR-E, AG, SA and NWij interpreted the data. RPR-E wrote the first draft, and NWis and MDN provided input for critical revisions. All authors contributed to the final version of the manuscript and subsequent revisions. RPR-E is the guarantor.
Funding This study was funded by a grant from the Rockefeller Foundation (Award number 2021 HTH 003) to the Johns Hopkins University and a subagreement with the Institute for Health Policy (IHP). Sri Lanka Health and Ageing Study Wave 2 data collection was supported by the Neelan Tiruchelvam Trust (Grant number 319/August/2021); the UK National Institute for Health and Care Research (NIHR) via a grant to University College London (grant number 17/63/47); and a grant from the Asia Foundation financed by the European Commission (award number ICSP/2020/417-844) and by the general funds of the Asia Foundation. Funding for dissemination was also provided by Gates Ventures.
Competing interests None declared.
Patient and public involvement Patients and/or the public were involved in the design, or conduct, or reporting, or dissemination plans of this research. Refer to the Methods section for further details.
Provenance and peer review Not commissioned; externally peer reviewed.
Supplemental material This content has been supplied by the author(s). It has not been vetted by BMJ Publishing Group Limited (BMJ) and may not have been peer-reviewed. Any opinions or recommendations discussed are solely those of the author(s) and are not endorsed by BMJ. BMJ disclaims all liability and responsibility arising from any reliance placed on the content. Where the content includes any translated material, BMJ does not warrant the accuracy and reliability of the translations (including but not limited to local regulations, clinical guidelines, terminology, drug names and drug dosages), and is not responsible for any error and/or omissions arising from translation and adaptation or otherwise.
Read the full text or download the PDF:
Disclaimer: Early release articles are not considered as final versions. Any changes will be reflected in the online version in the month the article is officially released.
Volume 30, Number 9—September 2024
Autochthonous Leishmaniasis Caused by Leishmania tropica , Identified by Using Whole-Genome Sequencing, Sri Lanka
Suggested citation for this article
Cutaneous leishmaniasis is atypical in Sri Lanka because Leishmania donovani , which typically causes visceral disease, is the causative agent. The origins of recently described hybrids between L. donovani and other Leishmania spp. usually responsible for cutaneous leishmaniasis remain unknown. Other endemic dermotropic Leishmania spp. have not been reported in Sri Lanka. Genome analysis of 27 clinical isolates from Sri Lanka and 32 Od World Leishmania spp. strains found 8 patient isolates clustered with L. tropica and 19 with L. donovani . The L. tropica isolates from Sri Lanka shared markers with strain Lt K26 reported decades ago in India, indicating they were not products of recent interspecies hybridization. Because L. tropica was isolated from patients with leishmaniasis in Sri Lanka, our findings indicate L. donovani is not the only cause of cutaneous leishmaniasis in Sri Lanka and potentially explains a haplotype that led to interspecies dermotropic L. donovani hybrids.
Leishmaniasis is a heterogeneous group of diseases caused by protozoan parasites of the genus Leishmania , transmitted by the bite of phlebotomine sand flies ( 1 ). The 3 typical clinical presentations of leishmaniasis affecting humans are visceral leishmaniasis (VL), cutaneous leishmaniasis (CL), and mucocutaneous leishmaniasis (MCL) ( 1 ). Those who are most affected are persons in Asia, Africa, and Latin America who suffer from poverty ( 2 ).
Although Leishmania donovani causes VL in other countries in Asia and Africa, an atypical variant of the same species is almost exclusively associated with CL in Sri Lanka ( 3 ). Common symptoms of CL are papules, nodules, plaques, and ulcers. Leishmaniasis cases in Sri Lanka have increased over the past 2 decades, from 22 in 2001 to 3,389 in 2022 ( https://www.epid.gov.lk ). Over the past 2 decades, <10 cases of leishmaniasis have been VL in Sri Lanka; some cases have included severe chronic conditions preceding or occurring after the Leishmania infection ( 4 ). There are 2 primary hotspots in Sri Lanka, 1 in the southern province and 1 in the north-central province ( 5 ).
The genetic factors associated with disease phenotypes of leishmaniasis are well understood. The A2 multigene family in Leishmania might be associated with either dermotropic or viscerotropic phenotypes ( 6 ). A2 gene variants encode stress-induced transmembrane proteins that are key for the parasite tropism to internal organs observed in visceralizing species ( 6 ). Abnormal changes in the number of chromosome copies that characterize extensive aneuploidy, usually harmful in most complex organisms, are frequent and highly tolerated in Leishmania parasites because they have a role in gene expression modulation ( 7 , 8 ).
The leishmaniasis disease profile worldwide is typically associated with the causative species of Leishmania ( 9 ). However, descriptions of emerging isolates and atypical phenotypes have made this association less clear ( 6 , 10 ). Recent genetic studies have shown that the Leishmania natural population structure is more complex than previously thought, partially because of the plasticity of the parasite genome and the occurrence of sexual reproduction ( 11 ). Isolates from the same clade might carry relevant genetic features accounting for shifts in clinical phenotypes. For example, L. donovani isotype MON-37 (from the Montpellier typing system) is the known causative agent of CL in Sri Lanka, and MON-2 is the known causative agent of VL in India ( 3 , 12 ).
A more recent analysis of L. donovani clinical isolates from Sri Lanka reported interspecies genomic hybrids between L. donovani and 2 common cutaneous species, L. major from Africa and L. tropica from the Middle East ( 13 ). The evidence of hybridization and introgression history in the Leishmania population in Sri Lanka suggests genetic exchange might have played a role in the insurgence of dermotropic L. donovani . However, many epidemiologic aspects of this model are unclear. Most CL causing L. donovani isolates described to date do not display clear evidence of hybridization with dermotropic species, and the parental strains of possible hybrid parasites in Sri Lanka remain unknown. Currently, <20 high quality next-generation sequencing (NGS) datasets of Leishmania spp. isolated from patients in Sri Lanka are publicly available ( 13 ). Therefore, it is crucial to perform whole-genome sequencing (WGS) analysis on a wider range of clinical isolates to better understand the atypical pathogenesis of leishmaniasis in Sri Lanka.
We studied WGS results of 27 Leishmania clinical isolates from Sri Lanka and made multiple genetic comparisons by using 32 different Old World Leishmania strains, including 5 interspecies L. donovani hybrids previously reported in Sri Lanka. Among the genomes analyzed, we describe autochthonous L. tropica isolates in patients from Sri Lanka who, apart from 1 exception, did not have travel history outside the country.
This study has been approved by the Ethics Review Committee, Faculty of Medicine, University of Colombo, Sri Lanka (approval no. EC-16-080). Written, informed consent was obtained from the participants.
Leishmania Culture
We cultured Leishmania promastigotes from 27 lesion aspirates (26 CL and 1 MCL) in M199 culture medium supplemented with 10% heat-inactivated fetal bovine serum (Thermo Fisher Scientific, https://www.thermofisher.com ) and 100 IU/ml of penicillin and 100mg/ml of streptomycin (Thermo Fisher Scientific). We incubated the cultures at 25 ± 1°C until the logarithmic phase promastigote count reached 10 7 /mL and then harvested them.
Genomic DNA Isolation and Sequencing
We extracted DNA from the cultured Leishmania promastigotes by using a QIAamp DNA Mini Kit (QIAGEN, https://www.qiagen.com ) and prepared libraries by using the Nextera XT DNA library preparation kit (Illumina, https://www.illumina.com ) and the Nextera DNA Flex library preparation kit (Illumina), according to the manufacturer’s instructions. Paired-end sequencing was conducted by Applied Biological Materials (British Columbia, Canada) by using the NextSeq (2×75bp) and HiSeq 4000 (2×150bp) platforms (Illumina).
WGS Data Analysis
We analyzed WGS data of 27 clinical isolates from this study and 32 Leishmania genomes of Old World species available from the National Center for Biotcechnology Information Sequence Read Archive ( https://www.ncbi.nlm.nih.gov/sra ) or the European Nucleotide Archive ( https://ebi.ac.uk/ena ). We detected genome-wide single-nucleotide polymorphisms (SNPs) in each sample after mapping high-quality reads to the reference strain, L. tropica L590 or L. donovani CL–Sri Lanka (genome available on TriTrypDB, https://tritrypdb.org ). We extracted the consensus sequences of 7 different genetic markers to identify the clinical isolates at the species level. Phylogenetic analysis by NGS multilocus sequence typing (MLST) involved 59 genomes of nucleotide sequences with the indicated number of base pairs from the following genes: ribosomal RNA internal transcribed spacer (ITS; L. donovani CL–Sri Lanka CP029526:1015798–1016063), 265 bp; glucose-6-phosphate dehydrogenase ( G6PD ; LtrL590_34:26953–27953), 1,001 bp; glucose-6-phosphate isomerase ( GPI ; LtrL590_12:302579–303479), 901 bp; isocitrate dehydrogenase precursor ( ICD ; LTRL590_SCAF000112:124407–125407), 1,001 bp; phosphomannose isomerase ( PMI ; LtrL590_32:632360–633360), 1,001 bp; aspartate aminotransferase ( AST ; LtrL590_35:290874–291838), 965 bp; and inosine-guanine nucleoside hydrolase ( IGNH ; LtrL590_14:44174–44933), 760 bp ( 14 ). We extracted the ITS reference sequence from the L. donovani CL–Sri Lanka reference genome because the ITS sequence is not fully assembled in L. tropica L590. We conducted phylogenetic analysis with maximum-likelihood method and tamura-nei model by using NGS MLST sequences as input in MEGA X ( 15 ). We compiled the pileup of read alignments to each locus used for 3 representative L. tropica genomes ( Appendix 1 Figure 1). We checked the aneuploidy profiles by inferring the chromosome copy values from whole-genome analysis normalized read depth after we mapped to the L. tropica L590 reference genome v.57, found in TriTrypDB, and assuming that all samples are diploid.
To confirm the absence of species admixture in the new L. tropica from Sri Lanka, we studied the genomewide zygosity profiles and the population genetic structure by tracking SNP frequencies in all 59 WGS samples. After mapping, we used aligned reads to identify SNPs in heterozygosity (allele frequency 0.15–0.85) or in homozygosity (allele frequency >0.85) by using the PAINT software suite ( 16 ). We investigated the gene sequences of the A2 virulence factor ( L. donovani CL–Sri Lanka CP029521:270000–320000) to identify any association with the phenotype of CL. We generated pseudo-sequences from 1,368,585 high-quality whole-genome linked SNPs that had information in > 50% of the samples to build phylogenetic network trees in SplitsTree v.6.0.2.3 ( https://software-ab.cs.uni-tuebingen.de/download/splitstree6/welcome.html ) ( 17 ). We calculated hamming distances and used the neighbor-net method to generate a splits network. A total of 1,000 bootstrap split replicates were used for internode confirmation of the phylogenetic tree of the L. tropica genomes, with a minimum 50% cutoff.
Data Availability
Data supporting the conclusions of this article are within the article and Appendix files, including Sequence Read Archive accession numbers for all the genomic data used in this work ( Appendix 2 Tables 1–3). We deposited raw sequencing data in the National Center for Biotechnology Information BioProject archive (accession no. PRJNA904745).
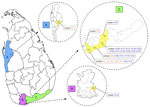
Figure 1 . Geographic locations of patients with cutaneous or mucocutaneous leishmaniasis in Sri Lanka. The mucocutaneous leishmaniasis patient was from the Puttalam district (A), Anamaduwa subdistrict. The cutaneous leishmaniasis patients were from...
We recovered Leishmania clinical isolates from 27 patients in 3 administrative districts in Sri Lanka: Hambantota (n = 25), Matara (n = 1), and Puttalam (n = 1) ( Figure 1 ). The CL patients were from the southern region and the MCL patient was from the north-western region of the country. Clinical manifestations of the CL lesions consisted of 8 papules, 3 plaques, and 15 ulcers. Eight of the ulcers were ulcerated nodules ( Appendix 2 Table 4).
Species Variability Among Clinical Isolates

Figure 2 . Phylogenetic analysis of Leishmania spp. clinical patient isolates from Sri Lanka and reference Leishmania spp. strains using sequences of the ribosomal RNA internal transcribed spacer (ITS). Sri...
NGS and MLST revealed that 19 genomes sequenced in this study belonged to the L. donovani complex and 8 to L. tropica . This finding was observed in every single locus investigated by MLST ( Figure 2 ; Appendix 1 Figures 2, 3). Of note, the ICD gene sequence of the single MCL isolate, HS1, is more similar to L. tropica strains from the Middle East (including LtKubba from Syria, and LtLT1 and LtLT2 from Lebanon) than to isolates from Sri Lanka ( Figure 2 ) ( 8 , 18 ).
Chromosome Copy Profiles

Figure 3 . Highly conserved aneuploidy profiles within the cutaneous Leishmania tropica clade from Sri Lanka. A) Heat map visualization of Leishmania abnormal chromosome numbers in 27 patient isolates from...
Genome-wide read depth analysis revealed highly conserved chromosome copy profiles among the 7 Sri Lanka L. tropica CL isolates (H9, H15, H19, H21, H24, H27, and H34), and a divergent pattern in the single MCL isolate, HS1 ( Figure 3 , panels A, B). Polysomy of chromosome 31 (>3 copies) was seen in all samples. This polysomy was commonly observed in previous studies on Leishmania spp ( 19 , 20 ).
Trisomy (2.4–3.5 copies) of chromosomes 2, 21, and 31 and near-trisomy (2.2–2.4 copies) of chromosomes 5, 8, 10, and 13 were detected in L. tropica isolates from Sri Lanka except for HS1, which displayed trisomic chromosomes 6, 9, 11, 14, 19, 20, 30, 32, and 33 ( Figure 3 , panel B). In comparison, L. donovani clinical isolates from Sri Lanka displayed a more heterogenous distribution of chromosome copy values with varied karyotypes ( Figure 3 , panels A, B). Of the 3 previously reported L. donovani–L. tropica hybrids, SRR67 and SRR66 showed multiple near-trisomy matches with the L. tropica isolates from Sri Lanka on chromosomes 5, 8, 10, and 13. Of note, near-monosomy of chromosome 2 (1.2–1.4 copies) was detected in SRR64, SRR65, and SRR69 ( Figure 3 , panel B).
Genome-Wide Zygosity Profiles and Phylogenetic Network Analysis

- Figure 4 . Frequency of genomewide heterozygous and homozygous SNPs in all genomes analyzed and presented as percent stacked bars after mapping sequencing reads from Leishmania spp. isolates from Sri Lanka. A)...
The total number of SNPs per sample ranged from 117,729 (in LtMA37 WGS) to 2,059,343 (in SRR65 WGS) within the sample cohort after mapping reads to the L. tropica L590 reference genome ( Figure 4 panel A). The 3 previously reported L. donovani–L. tropica hybrids showed low homozygosity (<0.12; SRR66–69). In contrast, most of the SNPs in the L. donovani isolates from Sri Lanka (H105–165) and in the intraspecies L. donovani hybrid LdHPCL66, identified in the Himachal Pradesh province of India, were homozygous (>0.98) ( Figure 4 , panel A) ( 10 ). Highly skewed heterozygosity was detected in most of the L. tropica genomes because they are genetically more similar to the L. tropica L590 reference genome than to L. donovani . For comparison, we also mapped reads to the L. donovani CL–Sri Lanka reference genome ( Figure 4 , panel B). As we expected for L. donovani – L. tropica progeny, both the genome-wide SNP frequencies and absolute numbers in the previously reported hybrids SRR66–69 were largely unaffected by the reference genome used for mapping ( Figure 4 ). All L. donovani laboratory strains showed high ratios of homozygous SNPs.
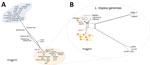
Figure 5 . Phylogenetic network of all Leishmania isolates from Sri Lanka and Old World strains analyzed and visualized as a splits tree built using genomewide single-nucleotide polymorphisms in SplitsTree 6 (...
We generated a network splits tree by using whole-genome SNPs for all the 59 Leishmania genomes, highlighting the separation between the L. donovani and L.tropica isolates from Sri Lanka, with the hybrids found in the middle point of the tree ( Figure 5 , panel A). A more detailed analysis by using only the data from the L. tropica genomes revealed 2 different subclusters of L. tropica in Sri Lanka. Although HS1 co-clusters with strains found in Syria (LtKubba) ( 8 ) and Lebanon (LtLT1 and LtLT2) ( 18 ) ( Appendix 1 Figure 4, panels A, B), the other L. tropica from Sri Lanka form a discrete subgroup more genetically similar to the LtK26 strain from India ( Figure 5 , panel B). This finding corroborated the phylogenetic profile observed by the MLST analysis by using the ICD gene sequence ( Appendix 1 Figure 3, panel C). Identification of L. tropica phylogenetic groups confirms worldwide L. tropica populations described by a previous comparative genomics study ( 18 ). We further expand on those findings by suggesting an additional population, consisting of LtK26 strain from India ( 8 ) and the H9–34 L. tropica from Sri Lanka.
Genomewide Genetic Variations and Shared Ancestries
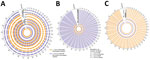
Figure 6 . Leishmania tropica and L. donovani strains from the Indian subcontinent that share genetic markers with interspecies hybrids found in Sri Lanka. A) Circos plot ( 22 )...

Figure 7 . Representative nucleotide-level visualization of the inheritance of parental allelic markers on chromosomes 1 (upper panel) and 36 (lower panel) in L. donovani – L. tropica hybrid SRR66, ...
From the list of SNPs identified by using the PAINT software suite ( 16 ), we selected the 1,354,425 homozygous alleles that were different between L. tropica K26 and L. donovani SL2706 as representatives of the 2 clades found in Sri Lanka. We tracked their inheritance in hybrids SRR66, SRR67, and SRR69 and in the 27 Sri Lanka isolates. L. donovani–L. tropica markers were remarkably heterozygous across the whole genome of the SRR66–69 hybrids, suggesting they have undergone recent hybridization with biparental contribution from L. donovani and L. tropica in all 36 chromosomes ( Figure 6 panel A). The number of SNPs shared with the L. tropica lineage from Sri Lanka was lower in the L. donovani – L. major hybrids (SRR64–65) ( Appendix 1 Figure 5); only 31.5% of the heterozygous SNPs were explained by the tested L. donovani–L. tropica admixture compared with 70% in the L. donovani–L. tropica hybrids (SRR66–69). Visual inspection at the single-nucleotide level confirmed the extensive heterozygosity of L. donovani–L. tropica markers in the SRR66–69 hybrids for most of the sites analyzed, which was not as evident in the SRR64–65 hybrids ( Figure 7 ; Appendix 1 Figure 6). The L. donovani (H105-H165) isolates from Sri Lanka showed low heterozygosity of selected parental markers and high similarity, and the L. tropica (HS1, H9-H34) isolates from Sri Lanka showed low heterozygosity of selected parental markers and high similarity to L. tropica from India lineages, evidence that these isolates have not experienced recent admixture of species ( Figure 6 , panels B, C).
A2 Gene Variations

- Figure 8 . Coverage plots of whole-genome sequencing reads mapped to the reference strain L. donovani cutaneous leishmaniasis from Sri Lanka. A) The absence of reads on the A2 gene locus in...
L. donovani and the hybrids from Sri Lanka contain the full A2 gene sequences of all 4 annotated copies in the L. donovani CL–Sri Lanka reference genome on chromosome 22. Read depths in L. tropica isolates from Sri Lanka were virtually zero in those positions ( Figure 8 , panel A), except for HS1, which contained very low partial coverage of the A2 gene, indicating a truncated gene sequence. Of note, isolates H106, H109, and H119 causing plaque lesions in patients were the only isolates from Sri Lanka to carry A2 sequences that are highly similar to the L. donovani CL–Sri Lanka reference, which also induced a plaque lesion phenotype ( Figure 8 , panel B).
This study identified an endemic L. tropica causing leishmaniasis in Sri Lanka. The 7 patients with CL caused by L. tropica had never traveled overseas, and 1 had not traveled outside their district of residence for 5 years. The CL patients had been living in their area of residence either since birth or for 20–60 years. Thus, it is likely that these are autochthonous cases of CL caused by L. tropica .
This study identified MCL caused by the L. tropica isolate HS1 in Sri Lanka. The patient’s upper lip, nose, and the perinasal regions were affected similar to previously reported cases of MCL caused by L. tropica ( 25 , 26 ). This MCL patient had traveled to Dubai and Iraq 8 years before the diagnosis and had no history of cutaneous leishmaniasis. The time elapsed since the first appearance of symptoms to diagnosis was ≈8 months ( Appendix 2 Table 4). Those facts suggest that either the patient began experiencing symptoms 7 years after a possible exposure during overseas travel or they acquired the infection in Sri Lanka.
The 7 cutaneous L. tropica isolates from Sri Lanka (H9–H34) were collected in southern Sri Lanka and belong to a genetically conserved subgroup that only co-clustered with L. tropica LtK26 from India. In contrast, the MCL-associated HS1 strain was isolated from a different geographic area and displayed a divergent chromosome copy profile more similar to L. tropica strains from Syria (LtKubba) and Lebanon (LtLT1 and LtLT2) than to the other L. tropica isolates from Sri Lanka ( Figure 3 ; Figure 5 , panel B), and a divergent genomewide SNP profile. Thus, it is possible that the infection was acquired in the Gulf region, and the mucosal manifestations might have become apparent years after the primary exposure.
Chromosome aneuploidy was evident among the study samples and the pattern differed between the L. tropica and L. donovani isolates. Noninteger chromosome copy values observed in this study are commonly found in Leishmania because of mosaic aneuploidy occurring in cultured parasite populations ( 19 ). Recent studies have shown that clonal growth in both sand flies and in vitro culture can by itself lead to major changes in chromosome copy values and karyotype diversity even after just 1 passage through the insect vector ( 20 , 27 ). In fact, concerning chromosome copy values, the L. donovani – L. tropica hybrids were among the most homogeneous genomes in our analysis.
From the data on patients’ residence and travel within Sri Lanka ( Appendix 2 Table 4), it is evident that both L. tropica and L. donovani may not be restricted to a single administrative area at the micro level. Considering that L. tropica is predominantly causing anthroponotic leishmaniasis and that the patients with CL have travel to other districts, further studies in additional locations and with other potential vectors would benefit the current understanding of leishmaniasis spread and genetic variability in Sri Lanka. In addition, zoonotic transmission of L. tropica through reservoirs such as rock hyraxes has been reported in other countries, and studies are needed to assess potential animal reservoirs of these parasites in Sri Lanka ( 28 ). Currently, there are no data available to dismiss either scenario, and both may represent valid and relevant routes of infection in the country. In addition to L. tropica causing cutaneous disease, its potential to visceralize in humans is known ( 29 – 31 ). Even though CL is the current predominant phenotype of leishmaniasis in Sri Lanka, the presence of L. tropica and L. donovani , both with potential visceralizing properties, raises concerns.
Studies on A2 gene expression in old world Leishmania spp. suggest its useful in determining species-specific organ tropism ( 32 ). Even though the pathogenicity of leishmaniasis is not fully understood, the understanding of CL lesions is they progress from an initial papule to a nodule or a plaque which can ultimately ulcerate. Several virulence factors were studied in the sequenced samples to understand the variability in Leishmania pathogenesis leading to different phenotypes. Because primarily cutaneous parasite species have a truncated A2 pseudogene, A2 is a gene family that occurs in L. donovani but not in L. tropica ( 6 ), a result seen in our study samples as well. A2 is necessary in the pathology of leishmaniasis and is known to aid in visceralization of the infection and survival within the host ( 33 – 35 ). Our analysis of the A2 gene in different phenotypes of L. donovani revealed marked differences in the plaque phenotype when compared with papules, nodules, and ulcers. A study conducted in Pakistan found that the clinical appearance of CL is not solely dependent on L. tropica genetic variations ( 36 ). This possibility could not be investigated in our study because most of the L. tropica –induced CL cases were ulcerated.
We have found there are > 5 different populations of Leishmania in Sri Lanka: SL1, SL2A, SL2B, SL3 ( 13 ), and L. tropica from Sri Lanka (SL4). Our study has shown L. tropica has caused both CL and MCL in Sri Lanka. Those findings suggest further studies on differences in clinical phenotypes, potential vector species, and reservoirs of Leishmania species in Sri Lanka would be beneficial. Revisiting diagnostic and research approaches might be necessary in consideration of this species variability. Analysis by PCR and restriction fragment length polymorphism represent the inexpensive and easy laboratory methods available for distinguishing between the 2 species ( 37 ).
In conclusion, although this large Leishmania WGS dataset provides valuable insights, further whole-genome studies might lead to better understanding of the Leishmania species infecting people in Sri Lanka and might shed light on the extent of genetic heterogeneity of infective clades circulating in the country. This discovery is a turning point in understanding the pathology of leishmaniasis in Sri Lanka and may contribute to the development of more efficient diagnostics and treatments for CL and MCL caused by L. tropica .
Dr. Silva is a senior lecturer in parasitology at the University of Colombo, Sri Lanka. Her research interests include epidemiology, pathogenesis, and treatment and drug resistance of human parasites.
Acknowledgments
We thank the staff members of the study sites, the Department of Parasitology at the University of Colombo, and Hernan A. Lorenzi for support with programming code.
This study was financially supported by the University of Colombo (grant no. AP/3/2/2017/PG/31); the United States-Japan Cooperative Medical Sciences Program, National Institutes of Health, USA (award no. DAA3-19-65623); National Institute of Allergy and Infectious Diseases, National Institutes of Health (award no. U01AI136033); and in part by the Intramural Research Program, National Institute of Allergy and Infectious Diseases, National Institutes of Health.
Author contributions: study design and leadership, H.S., N.V.C., and N.D.K.; funding acquisition, H.S. and N.D.K.; study oversight and supervision, N.D.K., N.V.C., and D.L.S.; data and sample collection, H.S.; bioinformatics analysis, H.S., K.M., S.S., and T.R.F.; data processing and data visualization, T.R.F.; data interpretation and manuscript drafting, H.S. and T.R.F.; provision of bioinformatic scripts and pipelines, E.V.C.A.F. and M.E.G. All authors reviewed the manuscript.
- Desjeux P . Leishmaniasis: current situation and new perspectives. Comp Immunol Microbiol Infect Dis . 2004 ; 27 : 305 – 18 . DOI PubMed Google Scholar
- Alvar J , Yactayo S , Bern C . Leishmaniasis and poverty. Trends Parasitol . 2006 ; 22 : 552 – 7 . DOI PubMed Google Scholar
- Karunaweera ND , Pratlong F , Siriwardane HVYD , Ihalamulla RL , Dedet JP . Sri Lankan cutaneous leishmaniasis is caused by Leishmania donovani zymodeme MON-37. Trans R Soc Trop Med Hyg . 2003 ; 97 : 380 – 1 . DOI PubMed Google Scholar
- Siriwardana HVYD , Karunanayake P , Goonerathne L , Karunaweera ND . Emergence of visceral leishmaniasis in Sri Lanka: a newly established health threat. Pathog Glob Health . 2017 ; 111 : 317 – 26 . DOI PubMed Google Scholar
- Karunaweera ND , Senanayake S , Ginige S , Silva H , Manamperi N , Samaranayake N , et al. Spatiotemporal distribution of cutaneous leishmaniasis in Sri Lanka and future case burden estimates. PLoS Negl Trop Dis . 2021 ; 15 : e0009346 . DOI PubMed Google Scholar
- Zhang WW , Ramasamy G , McCall LI , Haydock A , Ranasinghe S , Abeygunasekara P , et al. Genetic analysis of Leishmania donovani tropism using a naturally attenuated cutaneous strain. PLoS Pathog . 2014 ; 10 : e1004244 . DOI PubMed Google Scholar
- Sterkers Y , Lachaud L , Crobu L , Bastien P , Pagès M . FISH analysis reveals aneuploidy and continual generation of chromosomal mosaicism in Leishmania major. Cell Microbiol . 2011 ; 13 : 274 – 83 . DOI PubMed Google Scholar
- Iantorno SA , Durrant C , Khan A , Sanders MJ , Beverley SM , Warren WC , et al. Gene expression in Leishmania is regulated predominantly by gene dosage. MBio . 2017 ; 8 : 1 – 20 . DOI PubMed Google Scholar
- Burza S , Croft SL , Boelaert M . Leishmaniasis. Lancet . 2018 ; 392 : 951 – 70 . DOI PubMed Google Scholar
- Lypaczewski P , Thakur L , Jain A , Kumari S , Paulini K , Matlashewski G , et al. An intraspecies Leishmania donovani hybrid from the Indian subcontinent is associated with an atypical phenotype of cutaneous disease. iScience . 2022 ; 25 : 103802 . DOI PubMed Google Scholar
- Inbar E , Shaik J , Iantorno SA , Romano A , Nzelu CO , Owens K , et al. Whole genome sequencing of experimental hybrids supports meiosis-like sexual recombination in Leishmania. PLoS Genet . 2019 ; 15 : e1008042 . DOI PubMed Google Scholar
- Karunaweera ND . Leishmania donovani causing cutaneous leishmaniasis in Sri Lanka: a wolf in sheep’s clothing? Trends Parasitol . 2009 ; 25 : 458 – 63 . DOI PubMed Google Scholar
- Lypaczewski P , Matlashewski G . Leishmania donovani hybridisation and introgression in nature: a comparative genomic investigation. Lancet Microbe . 2021 ; 2 : e250 – 8 . DOI PubMed Google Scholar
- Zemanová E , Jirků M , Mauricio IL , Horák A , Miles MA , Lukeš J . The Leishmania donovani complex: genotypes of five metabolic enzymes (ICD, ME, MPI, G6PDH, and FH), new targets for multilocus sequence typing. Int J Parasitol . 2007 ; 37 : 149 – 60 . DOI PubMed Google Scholar
- Kumar S , Stecher G , Li M , Knyaz C , Tamura K . MEGA X: Molecular evolutionary genetics analysis across computing platforms. Mol Biol Evol . 2018 ; 35 : 1547 – 9 . DOI PubMed Google Scholar
- Shaik JS , Dobson DE , Sacks DL , Beverley SM . Leishmania sexual reproductive strategies as resolved through computational methods designed for aneuploid genomes. Genes (Basel) . 2021 ; 12 : 1 – 16 . DOI PubMed Google Scholar
- Huson DH , Bryant D . Application of phylogenetic networks in evolutionary studies. Mol Biol Evol . 2006 ; 23 : 254 – 67 . DOI PubMed Google Scholar
- Salloum T , Moussa R , Rahy R , Al Deek J , Khalifeh I , El Hajj R , et al. Expanded genome-wide comparisons give novel insights into population structure and genetic heterogeneity of Leishmania tropica complex. PLoS Negl Trop Dis . 2020 ; 14 : e0008684 . DOI PubMed Google Scholar
- Dumetz F , Imamura H , Sanders M , Seblova V , Myskova J , Pescher P , et al. Modulation of aneuploidy in Leishmania donovani during adaptation to different in vitro and in vivo environments and its impact on gene expression. MBio . 2017 ; 8 : 1 – 14 . DOI PubMed Google Scholar
- Ferreira TR , Inbar E , Shaik J , Jeffrey BM , Ghosh K , Dobson DE , et al. Self-Hybridization in Leishmania major. MBio . 2022 ; 13 : e0285822 . DOI PubMed Google Scholar
- Bussotti G , Gouzelou E , Côrtes Boité M , Kherachi I , Harrat Z , Eddaikra N , et al. Leishmania genome dynamics during environmental adaptation reveal strain-specific differences in gene copy number variation, karyotype instability, and telomeric amplification. MBio . 2018 ; 9 : 1 – 18 . DOI PubMed Google Scholar
- Krzywinski M , Schein J , Birol I , Connors J , Gascoyne R , Horsman D , et al. Circos: an information aesthetic for comparative genomics. Genome Res . 2009 ; 19 : 1639 – 45 . DOI PubMed Google Scholar
- Samarasinghe SR , Samaranayake N , Kariyawasam UL , Siriwardana YD , Imamura H , Karunaweera ND . Genomic insights into virulence mechanisms of Leishmania donovani : evidence from an atypical strain. BMC Genomics . 2018 ; 19 : 843 . DOI PubMed Google Scholar
- Robinson JT , Thorvaldsdóttir H , Winckler W , Guttman M , Lander ES , Getz G , et al. Integrative genomics viewer. Nat Biotechnol . 2011 ; 29 : 24 – 6 . DOI PubMed Google Scholar
- Shirian S , Oryan A , Hatam GR , Daneshbod Y . Three Leishmania/L. species— L. infantum, L. major, L. tropica —as causative agents of mucosal leishmaniasis in Iran. Pathog Glob Health . 2013 ; 107 : 267 – 72 . DOI PubMed Google Scholar
- Shirian S , Oryan A , Hatam GR , Daneshbod K , Daneshbod Y . Molecular diagnosis and species identification of mucosal leishmaniasis in Iran and correlation with cytological findings. Acta Cytol . 2012 ; 56 : 304 – 9 . DOI PubMed Google Scholar
- Bussotti G , Li B , Pescher P , Vojtkova B , Louradour I , Pruzinova K , et al. Leishmania allelic selection during experimental sand fly infection correlates with mutational signatures of oxidative DNA damage. Proc Natl Acad Sci U S A . 2023 ; 120 : e2220828120 . DOI PubMed Google Scholar
- Waitz Y , Paz S , Meir D , Malkinson D . Effects of land use type, spatial patterns and host presence on Leishmania tropica vectors activity. Parasit Vectors . 2019 ; 12 : 320 . DOI PubMed Google Scholar
- Sohrabi Y , Havelková H , Kobets T , Šíma M , Volkova V , Grekov I , et al. Mapping the genes for susceptibility and response to Leishmania tropica in mouse. PLoS Negl Trop Dis . 2013 ; 7 : e2282 . DOI PubMed Google Scholar
- Magill AJ , Grögl M , Gasser RA Jr , Sun W , Oster CN . Visceral infection caused by Leishmania tropica in veterans of Operation Desert Storm. N Engl J Med . 1993 ; 328 : 1383 – 7 . DOI PubMed Google Scholar
- Sacks DL , Kenney RT , Kreutzer RD , Jaffe CL , Gupta AK , Sharma MC , et al. Indian kala-azar caused by Leishmania tropica. Lancet . 1995 ; 345 : 959 – 61 . DOI PubMed Google Scholar
- Ghedin E , Zhang WW , Charest H , Sundar S , Kenney RT , Matlashewski G . Antibody response against a Leishmania donovani amastigote-stage-specific protein in patients with visceral leishmaniasis. Clin Diagn Lab Immunol . 1997 ; 4 : 530 – 5 . DOI PubMed Google Scholar
- Zhang WW , Matlashewski G . Characterization of the A2-A2rel gene cluster in Leishmania donovani : involvement of A2 in visceralization during infection. Mol Microbiol . 2001 ; 39 : 935 – 48 . DOI PubMed Google Scholar
- McCall LI , Matlashewski G . Localization and induction of the A2 virulence factor in Leishmania : evidence that A2 is a stress response protein. Mol Microbiol . 2010 ; 77 : 518 – 30 . DOI PubMed Google Scholar
- Al-Khalaifah HS . Major molecular factors related to Leishmania pathogenicity. Front Immunol . 2022 ; 13 : 847797 . DOI PubMed Google Scholar
- Khan NH , Llewellyn MS , Schönian G , Sutherland CJ . Variability of cutaneous leishmaniasis lesions is not associated with genetic diversity of Leishmania tropica in Khyber Pakhtunkhwa province of Pakistan. Am J Trop Med Hyg . 2017 ; 97 : 1489 – 97 . DOI PubMed Google Scholar
- De Silva NL , De Silva VNH , Deerasinghe ATH , Rathnapala UL , Itoh M , Takagi H , et al. Development of a highly sensitive nested PCR and its application for the diagnosis of cutaneous leishmaniasis in Sri Lanka. Microorganisms . 2022 ; 10 : 990 . DOI PubMed Google Scholar
- Figure 1 . Geographic locations of patients with cutaneous or mucocutaneous leishmaniasis in Sri Lanka. The mucocutaneous leishmaniasis patient was from the Puttalam district (A), Anamaduwa subdistrict. The cutaneous leishmaniasis patients were...
- Figure 2 . Phylogenetic analysis of Leishmania spp. clinical patient isolates from Sri Lanka and reference Leishmania spp. strains using sequences of the ribosomal RNA internal transcribed spacer (ITS). Sri Lanka isolates...
- Figure 3 . Highly conserved aneuploidy profiles within the cutaneous Leishmania tropica clade from Sri Lanka. A) Heat map visualization of Leishmania abnormal chromosome numbers in 27 patient isolates from Sri Lanka...
- Figure 5 . Phylogenetic network of all Leishmania isolates from Sri Lanka and Old World strains analyzed and visualized as a splits tree built using genomewide single-nucleotide polymorphisms in SplitsTree 6 (17)....
- Figure 6 . Leishmania tropica and L. donovani strains from the Indian subcontinent that share genetic markers with interspecies hybrids found in Sri Lanka. A) Circos plot (22) representation of the inheritance...
- Figure 7 . Representative nucleotide-level visualization of the inheritance of parental allelic markers on chromosomes 1 (upper panel) and 36 (lower panel) in L. donovani–L. tropica hybrid SRR66, L. donovani–L. major hybrid...
- Appendix 1 .
- Appendix 2 .
Suggested citation for this article : Silva H, Ferreira TR, Muneeswaran K, Samarasinghe SR, Alves-Ferreira EVC, Grigg ME, et al. Autochthonous leishmaniasis caused by Leishmania tropica , identified by using whole-genome sequencing, Sri Lanka. Emerg Infect Dis. 2024 September [ date cited ]. https://doi.org/10.3201/eid3009.231238
DOI: 10.3201/eid3009.231238
Original Publication Date: August 13, 2024
1 These authors contributed equally to this article.
Table of Contents – Volume 30, Number 9—September 2024
| EID Search Options |
|---|
| – Search articles by author and/or keyword. |
| – Search articles by the topic country. |
| – Search articles by article type and issue. |
Please use the form below to submit correspondence to the authors or contact them at the following address:
Nadira D. Karunaweera, University of Colombo, 25, Kynsey Road, Colombo 08, Sri Lanka
Comment submitted successfully, thank you for your feedback.
There was an unexpected error. Message not sent.
Metric Details
What is the altmetric attention score.
The Altmetric Attention Score for a research output provides an indicator of the amount of attention that it has received. The score is derived from an automated algorithm, and represents a weighted count of the amount of attention Altmetric picked up for a research output.
Sri Lanka Successfully Conducts Capacity Building Program in Clinical Management of Dengue– For Bangladeshi Health Staff
Dengue is a public health problem in Sri Lanka with over 50 000 cases reported each year in the recent past. The country has been successful in bringing down the Case Fatality Rate (CFR) over the last two decades which was around from 5% in 1996 to 1% in 2009 and has declined gradually over time to 0.07% in 2023. It shows the resilience and high capacity of the curative sector in managing of dengue patients. However, the country experiences rising cases during the rainy seasons in June-July and October-December every year. During the last quarter of 2023, almost all districts of the country have reported dengue cases, with Colombo, Gampaha and Kalutara districts in the Western Province having the highest case detection rates during this year.
/countries/sri-lanka/capaci-1.jpg?sfvrsn=4673449_10)
Sri Lanka’s achievement is due to multiple factors such as the availability of evidence-based clinical guidelines, continuous capacity building of clinical staff, and regular organization of dengue death review processes, which were streamlined from 2009 onwards. However, dengue continues to be a challenge for Sri Lanka.
National Institution of Infectious Diseases (NIID) which was established in 1926 is the pioneer infectious disease hospital in Sri Lanka. NIID rendered its valuable service during recent major events, notably during the Dengue 2017 epidemic and COVID-19 (2020-2021) pandemic. The hospital has modern treatment facilities (including a specialized dengue treatment unit), a highly skilled and dedicated staff, and a national level training facility for clinical management of dengue.
In 2022 and 2023 around 500 doctors and nurses were trained by NIID on clinical management of dengue. These programmes were conducted in collaboration with the National Dengue Control Unit (NDCU). The World Health Organization (WHO) has always given technical and financial support when requested for these training.
/countries/sri-lanka/capaci-3.jpg?sfvrsn=da0cf525_7)
The National Institute of Infectious Diseases in collaboration with the National Dengue Control Unit of the Ministry of Health, Sri Lanka, conducted the first international training on dengue case management from 22 to 28 July 2024. This training was designed for a group of selected doctors and nurses nominated by the Ministry of Health and Family Welfare, Bangladesh. In addition to the hands-on training, the participants also learnt on how health facilities need to be set up for treatment and monitoring of dengue patients and also gained an understanding on the leading roles of nurses in dengue case management and monitoring. The training comprised of presentations/lectures, discussions, hands-on training, clinical training, field visits and interactive sessions. Moreover, a symposium composed of knowledge sharing sessions was held with the Ministry of Health top officials, renowned clinicians, academicians, research staff and provincial and district level officials.
This initiative is set to significantly enhance the dengue case management in Bangladesh and strengthen healthcare ties between two countries in years to come.
Nepal, Bhutan and Myanmar have expressed their interests in receiving the training on dengue case management in Sri Lanka through NIID. Therefore, national efforts will continue to introduce regular capacity building programs for countries that showed interests.
/countries/sri-lanka/capaci-2.jpg?sfvrsn=74d1ab46_5)

13th Sri Lanka Economic Research Conference 2024: ‘Back to Basics’ Policy Stance as a Way Out of the Economic Crisis
- Posted by Admin
- Categories News
- Date August 9, 2024

The 13 th Sri Lanka Economic Research Conference (SLERC) 2024 of the Sri Lanka Forum of University Economists (SLFUE) was held at General Sir John Kotelawala Defence University, Sri Lanka, on 9 th August 2024.
The conference was held under the theme ‘Back to Basics’ Policy Stance as a Way Out of the Economic Crisis . The conference was proudly hosted by the Faculty of Management, Social Sciences and Humanities of KDU. The inauguration ceremony of the conference was held in the auditorium of the Faculty of Graduate Studies with grandeur and splendor. The ceremony was graced by the esteemed presence of Rear Admiral HGU Dammika Kumara, VSV, USP, psc, MMaritimePol, BSc (DS),Vice Chancellor of General Sir John Kotelawala Defence University, the Chief Guest of the occasion, alongside Dr. Chandranath Amarasekara, Assistant Governor of the Central Bank of Sri Lanka, the keynote speaker, Dr. Wasantha Premarathne, Chair, Sri Lanka Forum of University Economists 2024, Dr. Lakshika Liyanage, Dean, Faculty of Management, Social Sciences and Humanities, Dr. Tamara Jayasundera, Chair, 13 th Sri Lanka Economic Research Conference 2024. Economists from Sri Lankan state universities around the country added color to the inaugural event of 13 th SLERC 2024. Dr. Wasantha Premarathne, Chair of SLFUE 2024, welcomed the dignitaries and esteemed guests to the conference. Rear Admiral HGU Dammika Kumara, Vice Chancellor of KDU delivered the Speech of the Chief Guest. The eminent Dr. Chandranath Amarasekara, Assistant Governor of the Central Bank of Sri Lanka, delivered the keynote speech under the topic “Sri Lanka’s crisis, recovery and the way forward”. The inauguration ceremony of 13 th SLERC 2024 was followed by the panel discussion moderated by eminent Prof. N S Cooray. The panelists of the discussion, Senior Prof. Udith Jayasinghe-Vice Chancellor of the Wayamba University of Sri Lanka, Dr. Prasad Dharmasena-Director/CEO, National Institute of Plantation Management, Mr. Sheran De Alwis-Chief Compliance Officer, Ma’s Tropical Food Processing (Pvt) Ltd., and Mr. Upul Jayatissa-Former Managing Director of Sri Lanka Ports Authority conveyed valuable insights, discussing topics related to diversified economic approaches in dealing with the Sri Lankan economic landscape.
The technical sessions were held subsequently at the Faculty of Management, Social Sciences and Humanities of KDU. Presenters from Sri Lankan universities and corporate sector shared significant research insights under various tracks with the participants and were followed by thought-provoking discussions. The chairpersons of the sessions, Emeritus Prof. P Hewage, Prof. Ganganee Samaraweera, Prof. MMDR Deegahawature, Dr. AM Indika Gunarathna, Prof. AMM Mustafa, Ms. Sarojini Maheswaranathan, Prof. RA Rathnasiri, Mr. S Santhirakumar, Prof. SWGK Bulankulama, Dr. AAM Nufile, Dr. Tamara Jayasundera, Dr. Sashi Weerawansa, Dr. Abdul Cader Mohamed Hanas, Dr. RMNT Sirisoma, Dr. TK Karandakatiya, Prof. NS Cooray, Prof. Suresh Kanesh, Prof. HMA Herath, and Dr. W Premarathne, coordinated the sessions with expertise and exemplary leadership.
The topics of the parallel technical sessions were as follows: Agriculture and Rural Development, Digital Economy and Innovation, Education and Human Capital, Financial Infrastructure, Regulatory Framework and Governance, Labour Markets, Macroeconomics Fundamentals, Infrastructure Development, Social and Environmental Responsibility and Trade and Global Relations.
After successfully concluding the 13th SLERC 2024 of SLFUE, the 50th meeting of the SLFUE was conducted at the FMSH building. At the commencement of the meeting, the members of the SLFUE expressed their gratitude to Professor Lalithasiri Gunaruwan for his pioneering role as the co-founder of the SLFUE.

Previous post
You may also like

477th Committee of Vice Chancellors and Directors (CVCD) Meeting

Film Festival at KDU Celebrates Cinematic Arts with French Flair

COMMENTS
Call our award-winning support team 24/7 at +94 77 288 4021. 4.8/5 (472) . Discover expert assignment writing services at Assignment Lanka. Your trusted partner in Sri Lanka for essays & dissertations.
Our team of academic research expert and professional writers can help you write plagiarism-free academic research paper, conference paper, journals, report, assignments, essays, coursework, thesis & dissertations in the following fields: Information Technology & Computer Science Coursework. Information Technology & Computer Science Proposal ...
Professional Assignment Help for Sri Lankan Students. Assignment.lk offers unmatched assignment writing service for Sri Lankan students while being more than a decade within the industry through creating a new price era within the entire assignment writing service industry in Sri Lanka. Our vision is to "eliminate all assignment writing ...
The President's Awards for Scientific Research (PASR) for publication year 2019 & 2020. read more. 2nd Annual Research Symposium - 2023. ... Life Evaluation, Repair and Retrofitting of Existing Bridges in Sri Lanka Due to Overloading and Environmental Interaction. READ MORE. Snake Bite in Sri Lanka. Developing a Polyvalent Anti-Venom for ...
This is why BestAssignments.lk steps in to help students and employees to achieve their bigger dreams while enjoying a balanced life. ... Case studies/ Research papers, PPT. SUBJECTS. Accounting. Business Management. Business Psychology ... Sri Lanka Phone: +94763300991 Web: www.bestassignments.lk International inquiries: sales@bestassignments ...
The National Science Foundation (NSF) of Sri Lanka plays a pivotal role in supporting and strengthening the National Research, Development, and Innovation Ecosystem to promote wealth creation and ensure the wellbeing of the citizens of Sri Lanka. NSF, as a key government organization, has designed its programmes and initiatives to contribute to this endeavor at three different levels as shown ...
Assessing law & policy. Verité Research has a team of lawyers with expertise in constitutional law, labour law, trade and investment, human rights, international law, and the administration of justice. The team's research focuses on three main thematic areas. The first involves constitutional, legislative and judicial analysis.
The University of Colombo takes great pride in nurturing a strong dedication to cutting-edge research and our respected faculty, institutes, school, and campus across various disciplines actively contribute to high-quality research, making a positive impact both locally and internationally. Our researchers are dedicated to addressing pressing ...
We are a company based in Sri Lanka with the team of expert writers in Academic writing from countries around the globe. We provide legitimate and 100% trusted writing services in Sri Lanka. We offer services including Assignment Writing, Dissertation Writing, Essay Writing, Proposal Writing, Presentations, Thesis writing, Proof Reading, Web ...
The Research Team - Research Support Services in Sri Lanka. The Research Team - Research Support Services in Sri Lanka. 562 likes. This group consist of university undergraduates and students advancing their...
Research Support Centre. The main objective of setting up the RSC is to support trainees develop the generic skills related to research such as conducting a literature search, appropriate referencing, avoiding plagiarism, use of software packages for data analysis, applying for ethical approval and applying for research grants.
The NRC provides funds for Scientific Research Projects. Grants are open to any researcher of a Public R & D organization in Sri Lanka. Public R& D organizations are the National Research Organizations, Universities and Affiliated Colleges and any governmental and semi-governmental organization where a research option exists in the mandate.
The University of Colombo, in accordance with its commitment to promote, safeguard and increase the knowledge and scholarship in the fields of social sciences and the humanities and science and technology, established the "Center for Research and Development" [CRD] in 2016 through a by-law approved by the Senate and the Council of the University of Colombo.
For our clients, this means getting them the information that matters most to them in less time,through time efficient research and information services. Our Services. We currently offer macroeconomic advisory mainly in the form of presentations and reports, sectoral insights and information curations services. ... Sri Lanka. T: +94 11 4373477 ...
TK Research & Solutions is a Colombo Based Market Research Agency, we are one stop solution for all your market research needs. We help our clients discover their true potential audiences across the world with our research experts. Leading market research company in Sri Lanka, our services include data collection, retail census and much more.
A. M. A. S. M. Bandara, L. N. A. C. Jayawardena. Apr 27, 2023. 45 ( 2): 199-212. …. Sri Lanka Journal of Social Sciences (SLJSS) is published by the National Science Foundation of Sri Lanka. It publishes social science articles on topics relevant to Sri Lanka in particular and South Asia in general.
This research used CA to model the pattern of urban sprawl in the Kurunegala district in Sri Lanka, within the period from 2022 to 2027. The model was developed using land use land cover (LULC ...
DAAD Information Centre Colombo. Sri LankaColombo +94 11 231 43 64 / 67 (Ext. 210) +94 711625334. Address: 15th Floor, 127 W A D Ramanayake Mawatha, Colombo 00200, Sri Lanka.
A: Sri Lanka's efforts in reducing poverty have been praiseworthy. Excluding the Northern and Eastern provinces, headcount poverty fell from 22.7 percent to 6.1 percent between 2002 and 2012/13. In that same period, extreme poverty in Sri Lanka decreased from 13 percent to less than 3 percent in 2012/13— lower than many of Sri Lanka's ...
Notable among these are the Institute of Policy Studies, who promote policy-orientated economic research and aim to strengthen policy-analysis capacity in Sri Lanka; the Coconut Research Institute of Sri Lanka which was founded in 1928, making it the first ever research institute devoted to the study of the coconut industry; and the Medical ...
This paper stands to add a perspective from a developing Asian country to the existing literature and debate about the issue of public understanding of research. As Sri Lanka has higher health indicators and a better developed health system and infrastructure than most developing countries in Africa and Asia coupled with a high literacy rate ...
Showing 10 Publication (s) 13% primary expenditure rule proposed for Sri Lanka departs from economic theory and practice. The 13% primary expenditure rule proposed in a new public finance bill is at odds with established economic theory. It will undermine "good" public spending that enhances growth, efficiency, and social welfare.
PhD, MBA, SLIM & HND Assignment Writers Sri Lanka - Facebook
Sri Lanka is rapidly becoming a hub for transnational education. In 2022-2023, it emerged as the second-largest country for UK TNE, accounting for 10% of all UK TNE enrolments globally with a 50% surge in UK TNE—totalling almost 54,000. ... This research report highlights the immense potential of TNE in bridging the gap in higher education ...
This study examines how Sri Lanka, a lower-middle income country, managed its COVID-19 response and maintained health services. It draws on an extensive document review, key informant interviews and a national survey of public experience and opinion to assess what Sri Lanka did, its effectiveness and why. Owing to a strong health system and luck, Sri Lanka stopped the first wave of COVID-19 ...
Sri Lanka's parliament passed a new telecommunications bill last month, which amended the law for the first time in 28 years and paved the way for Starlink Lanka to enter the country.
Abstract. Cutaneous leishmaniasis is atypical in Sri Lanka because Leishmania donovani, which typically causes visceral disease, is the causative agent.The origins of recently described hybrids between L. donovani and other Leishmania spp. usually responsible for cutaneous leishmaniasis remain unknown. Other endemic dermotropic Leishmania spp. have not been reported in Sri Lanka.
Dengue is a public health problem in Sri Lanka with over 50 000 cases reported each year in the recent past. The country has been successful in bringing down the Case Fatality Rate (CFR) over the last two decades which was around from 5% in 1996 to 1% in 2009 and has declined gradually over time to 0.07% in 2023. It shows the resilience and high capacity of the curative sector in managing of ...
The 13 th Sri Lanka Economic Research Conference (SLERC) 2024 of the Sri Lanka Forum of University Economists (SLFUE) was held at General Sir John Kotelawala Defence University, Sri Lanka, on 9 th August 2024.. The conference was held under the theme 'Back to Basics' Policy Stance as a Way Out of the Economic Crisis.The conference was proudly hosted by the Faculty of Management, Social ...
COLOMBO (Reuters) - Sri Lanka's presidential election race gathered pace on Thursday, as 39 candidates submitted nomination papers to the Election Commission by the deadline ahead of the vote on ...